Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- References
- Copyright
A Review: Pharmacogenomics and Personalized Medicine
Authors: Prof. Gutte V. P, Kumbhar Shivam, More Mohan, Jadhav Prasad
DOI Link: https://doi.org/10.22214/ijraset.2023.57183
Certificate: View Certificate
Abstract
Optimizing treatment effectiveness and reducing the risk of medication toxicity for each patient is the aim of customized medicine. It demonstrates the proper substance and dose, the appropriate patient, and the timely delivery of treatment. Molecular diagnosis and customized medication regimens based on each patient\'s unique genetic composition are the main goals of personalized medicine. This study\'s primary goal is to assess personalized medicine\'s uses, advantages, drawbacks, and consequences for healthcare. Prospective viewpoints and real-world clinical implementations. Personalized medicine promises to diagnose, stop, and treat disease. Pharmacogenomics (PGx) is the study of how genetic variation in an individual\'s reaction to medication occurs. It is the newest branch of medicine and is rapidly developing as a field of study. The pharmaceutical business is learning how to apply it, include it into the process of developing new drugs, and better handle the expectations of the medical community. Pharmacogenomics can provide more effective and less adverse effect treatments by customizing medications to a patient\'s genetic composition. Big pharma corporations have not embraced individualized medicine despite these advantages.
Introduction
I. INTRODUCTION
Pharmacogenomics: - It is the study of genetic variants between individuals that affects their response to drugs, both therapeutically and in terms of side effects. It is defined as the analysis of the drug which is used to treat on the any one disease and also study and analysis of our body and treat the personalized medicines. Pharmacogenetics is the study of the interaction between a person’s genes and the drug. They are taking. The term 2 is almost 60 years old 2,3, but it is only in the last 15 years that our Ability to test and understand the function of these genes, together with the accumulating Evidence of utility from clinical trials, have brought pharmacogenetics into clinical practice. Within the last 10 years, more than 21,000 articles on pharmacogenetics have been cited in PubMed, with the volume now growing at 200 articles per month. The clinical significance of Pharmacogenetics is recognized by the FDA which includes pharmacogenetic information on ~15% of drug labels.
Three elements of an individual's reaction to a medication are related to pharmacogenetics:
- The drug's genetic target in the patient;
- The genetic control of the drug's metabolism within the patient
- The genetic predisposition of the patient to a serious drug reaction.
Gene variations that are inherited can alter one or more of these three characteristics. When it comes to medications intended to treat tumors, somatic or "non-heritable" mutations in cancer can alter the genetically defined target. This Statement focuses on the inherited genetic factors associated with these three aspects; it does not address the clinical significance of somatic mutations in cancer as targets for targeted chemotherapy.
The use of genetics to enhance drug discovery and development is referred to as pharmacogenomics. This phrase generally refers to customized medications or personalized medicine, which develops the appropriate medication for the appropriate patient. Molecular pharmacology and functional genomics are the marriage of personalized medicine.
The goal of pharmacogenomics is to identify and interpret relationships between a patient's genotypes, or genetic profile, and how well they respond to treatment. These correlations are used by pharmacogenomics to find novel, highly effective treatments based on a patient's genetic makeup. The procedure entails identifying genes and the protein offspring that they produce as putative therapeutic targets, followed by an understanding of the gene variations.. Growing evidence that an individual's genetic profile is and will remain the primary predictor of the efficacy of specific therapies is driving interest in and funding for pharmacogenomics.
The study of pharmacogenomics focuses on the significant clinical impacts of individual gene variations in small groups of patients. To find variants, pharmacogenomics, on the other a wide range of genomic loci, including the entire genome and major biological pathways.
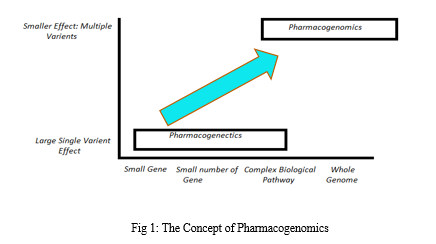
The first study on pharmacogenetics was transformed into pharmacogenomics in the concept of pharmacogenomics. Additionally, the small and large effects, as well as the few and large number of genes, are depicted in this figure. the entire gene study and small-to-large variance effect.
The study of different genomic data, such as polymorphisms, gene expression, copy number, methylation, and protein profiles, to determine how differently drugs react to patients is known as pharmacogenomics. Detecting evidence of variation in response to drug action and factors influencing the chemical agents' absorption, distribution, metabolism, and excretion are the goals of these analyses. The next frontier in research is pharmacogenomics, which is thought to be an outgrowth of the human genome project. A large amount of industrial investment is expected in this area.
II. SCIENTIFIC BACKGROUND
A number of genetically regulated processes affect how a chemical affects a person's body when they consume it. Since each person has a different set of genes involved in those processes, so too can the effects of each chemical on an individual. These guidelines apply to the consumption of any substance, including poisons and pharmaceuticals. The genetic variation underlying these steps most likely represents adaptive responses to various environmental toxins. The clinical significance of these variations has shifted from understanding differences in responses to toxins to understanding differences in responses to drugs with the advent of pharmaceutical therapies.
Broadly speaking, the differences in how a medicine is metabolized by the body can comprise:
- modification of the drug by the liver, yielding metabolites which may have reduced or enhanced biological effect
- transport of the drug and metabolites from the blood into specific organs and cells
- binding of the drug and metabolites to a biological target in the cell; this includes the potential binding of the drug and its metabolites to immune cells which trigger an adverse reaction
- active excretion of the drug and metabolites from the cell into the blood stream
- active excretion from blood into bile, faeces, or urine.
- absorption of the drug through the intestinal wall.
Pharmacogenetics' main objective is to prevent these negative effects by analyzing the genes that cause individual differences in how they respond to medications. One benefit of genetic analysis is that it can use widely available conventional procedures for DNA analysis, making pharmacogenetic testing more accessible to patients. This includes using pharmacogenetics to whole genome sequencing, which analyzes and reports a patient's complete genetic code.
However, it can be difficult to generate precise forecasts based solely on genetic study due to the complexity mentioned above. It is likely to be more accurate to include statistical modeling of pharmacokinetics (also known as "Bayesian dosing") and studies of numerous drug metabolites (also known as "pharmaco-metabolomics"). Individuals who have a congenital metabolic condition, such as G6PD deficiency, may also be susceptible.
III. PHARMACOGENOMICS IN USE
Nowadays, pharmacogenomics is used to a limited extent. The liver enzymes belonging to the cytochrome P450 (CYP) family are in charge of dissolving over thirty distinct drug classes. Variations in the DNA of the genes encoding these enzymes can affect how well they metabolize specific medications. Patients may overdose on medicines if they have less active or inactive types of CYP enzymes, which are unable to effectively break down and remove drugs from the body. Genetic assays for cytochrome P450 gene variants are now used by clinical trials researchers to evaluate and track participants. Furthermore, a lot of pharmaceutical businesses test their chemical compounds to evaluate how efficiently different CYP enzyme variants can break them down.
Thiopurine methyl-transferase (TPMT) is an additional enzyme that breaks down a class of medicinal chemicals called thiopurines, which is useful in the chemotherapeutic treatment of common childhood leukemia. A tiny proportion of Caucasians are genetically predisposed to be unable to produce this protein in an active form. Because the inactive version of TMPT is unable to break down the medicine, thiopurines rise to hazardous levels in the patient. TMPT activity is monitored to determine appropriate thiopurine dosage levels, and clinicians may already screen patients for this deficit using a genetic test14. scientific frontier and substantial industrial investment is predicted in this arena.
A. Pharmacogenomics in Clinical Practice
It is now possible to include pharmacogenomics into clinical practice. The US Food and Drug Administration (FDA) has started the process of licensing the use of pharmacogenomic data for dose selection in cancer treatment, in addition to genotype-guided clinical trials. UGT1A1 expression is changed by a dinucleotide TA repeat in a TATA box in the UGT1A1 promoter. The number of TA repeats varies from five to eight copies. The most frequent allele, or wild-type UGT1A1 expression, is represented by six TA repeats, while the most common variant allele, or reduced UGT1A1 expression, is represented by seven TA repeats (UGT1A1*28). A higher risk of toxicity from irinotecan therapy, such as severe diarrhea and neutropenia, is associated with reduced UGT1A1 expression. A prospective study administered irinotecan to 66 patients with advanced disease. UGT1A1*28 genotype and haplotypes containing UGT1A1*28 were correlated with irinotecan pharmacology and the occurrence of severe toxicity. Patients homozygous for UGT1A1*28 had a significantly greater risk of grade IV neutropenia compared with heterozygous or homozygous wild-type patients. In 2005 the FDA approved a genetic test for UGT1A1*28 and included toxicity and dosing warnings relating to the UGT1A1*28 allele in the irinotecan package insert, marking a significant step towards the integration of pharmacogenomics into clinical practice.
In practice, once an assay has been validated for clinical use, parameters cannot be changed without re-validation. This also represents a major challenge when NGS technology is continuously evolving, which relates to yet another challenge, namely that reproducing results may not be possible over time given the rapidity with which the technology is changing. FIn practice, once an assay has been validated for clinical use, parameters cannot be changed without re-validation. This also represents a major challenge when NGS technology is continuously evolving, which relates to yet another challenge, namely that reproducing results may not be possible over time given the rapidity with which the technology is changing (5)
The USA CDC working group Nex-StoCT II, CAP/AMP, ACMG, FDA, the UK organization ACGS, the Dutch Genome Diagnostic Laboratories, and the Korean Society of Pathologists have all released best practice guidelines for clinical NGS.Newer guidelines do not include the requirement for orthogonal validation of all reported variants, which is likely because of growing evidence that most variants do not require it. This means that labs can now be more selective about which variants they choose to confirm using an orthogonal method
Numerous pharmacological classes, such as immunosuppressants, psychotropics, antimicrobials, antidepressants, selective oestrogen receptor modulators, beta blockers, statins, proton pump inhibitors, anticoagulants, and antiplatelet medicines, have a large number of identified gene-drug combinations. Gene variant frequencies (4–74%) and medication toxicity severity vary significantly amongst genes. Poor medication metabolism in six patients can lead to toxicities that range from moderate to severe, necessitating hospitalization, admission to an intensive care unit, or even death. By looking for genetic variations linked to the tolerance of certain drugs, we can forecast a patient's metabolic reaction and modify their pharmaceutical regimen accordingly, enabling individualized dosing.

Challenges:-Pharmacogenomics is a developing research field that is still in its infancy. Several of the following barriers will have to be overcome before many pharmacy.
Table 2: Challenges of Pharmacogenomics"
|
Challenge |
Potential Approaches |
|
Establishing that drug responses are heritable
|
Twin studies; family studies Linkage between drug response and genomic loci in cell lines, or model Organisms |
|
Defining candidate genes
|
Pharmacokinetic Pharmacodynamic Drug targets biological milieu in which drugs act Disease genes and pathways Whole genome approaches |
|
Defining drug responses
|
Biomarkers Surrogates "Hard" end points |
|
Data management, including uniform representation of phenotypic data
|
Improved informatics Centralized, Web-accessible public database relating genetic variants a drug response: www.PharmGKB.org |
|
Reproducibility |
Replication sets Statistical analysis of associations |
|
Statistical analysis of associations |
New statistical methods, including consideration of haplotypes. |
|
Interrogating very large sets of polymorphisms in large numbers of patients |
New platforms (e.g, chip- or bead-based) |
|
Moving to practice |
Reproducible study results Cost-effectiveness Health care provider education. |
IV. LIMITATIONS
Reaction to a medicine is likely to be influenced by multiple genes. This implies that targeting distinct medications could be exceedingly intricate. Everybody has slight differences in their genes that have no effect on how the gene functions. These changes would need to be discovered 40 because they might affect how the illness develops or how drugs are metabolized.
A. Anticipated Benefits of Pharmacogenomics
- More Potent Medications: Drug manufacturers are able to develop medications based on proteins, enzymes, and RNA molecules connected to genes and illnesses. This will speed up the search for new drugs and enable producers to create treatments that are more specialized to particular illnesses. This precision will minimize harm to neighbouring healthy cells in addition to optimizing therapeutic benefits.
- Safer, Better Drugs:Physicians will have the ability to evaluate a patient's genetic profile and recommend the optimum drug therapy from the start, replacing the current trial-and-error approach of matching patients with the appropriate medications. This will not only remove uncertainty from selecting the appropriate medication, but it will also expedite recuperation and enhance security by removing the possibility of negative responses.
- More Accurate Methods of Determining Appropriate Drug Dosages: Current methods of basing dosages on weight and age will be replaced with dosages based on a person's genetics--how well the body processes the medicine and the time it takes to metabolize it. This will maximize the therapy's value and decrease the likelihood of overdose.
- Advanced Screening for Disease: Knowing one's genetic code will allow a person to make adequate lifestyle and environmental changes at an early age so as to avoid or lessen the severity of a genetic disease. Likewise, advance knowledge of a particular disease susceptibility will allow careful monitoring, and treatments can be introduced at the most appropriate stage to maximize their therapy.
- Better Vaccines: Vaccines made of genetic material, either DNA or RNA, promise all the benefits of existing vaccines without all the risks. They will activate the immune system but will be unable to cause infections. They will be inexpensive, stable, easy to store, and capable of being engineered to carry several strains of a pathogen at once.
B. Polygenic Pharmacogenomics
Strategies Although there are several published exemplifications of clinically applicable polymorphisms, it's clear that assessing a single polymorphism in a single gene won’t give all of the information needed to directly elect remedy in advance of treatment. Whilst UGT1A1 * 28 is easily associated with the prevalence of toxin from irinotecan, not all cases who witness toxin carry the UGT1A1 * 28 polymorphism.
Genotyping of fresh polymorphisms within UGT1A1, especially in populations with low prevalence of UGT1A1 * 28, may give a clearer picture of toxin threat. In addition, several other genes could contribute to irinotecan toxin. For illustration, genotyping of tagSNPs in themulti-drug transporter ABCC2 may also be of significance to prognosticate cases at threat for irinotecan toxin. medicine exertion and efficacity is doubtful to ever be defined by the conduct of a single gene, or a single polymorphism within a gene. Once comprehensive assessment of seeker genes and polymorphisms has been completed, panels of labels will need to be linked for each treatment combination to make a comprehensive pharmacogenomic profile for each case. important progress has been made in pharmacogenomics over the once decade, but there's a considerable quantum of work remaining before pharmacogenomics is completely integrated into clinical practice.
V. PERSONALIZED MEDICINE
Individualized drugs be a remedial strategy targeted too individual cases or cluster of cases. Are frequently outline as a blend of progressive molecular identification and ancient strategies, for opinion and remedial ways exactly acclimatized to individual cases like case history. ( 5)
The impact of biomarker technology and biomarker strategies in pharmaceutical development is still in its immaturity; but the impact is formerly proving significant. Biomarker strategy forms the base for personalised drug, the assiduity/ nonsupervisory focus centres on perfecting the success rate and reducing the high waste rate frequently encountered in early phases of clinical exploration. The depth and breadth of knowledge needed to successfully apply biomarkers into medicine development is generating company collaborations and addition of professionals that haven't traditionally been part of medicine product development.
The approach depends on scientific development in our appreciation of still a person’s distinctive molecular and heritable profile makes them liable to set conditions.4 According to the EU Administrative analysis Service( EPRS 2015), it refers to Associate in Nursing “ arising- evolving approach to medicine ” that uses scientific perceptivity into the heritable and molecular base of health and illness brought on by the sequencing of the mortal order, to guide in connection the prophecy , prevention, identification and treatment of illness.
The advancement of molecular profile technology to get access on RNA, DNA and protein will potentiate the individualized drug for managing the complaint. Precision drug having colourful advantages over conventional drug like optimum remedy needed, increase safety and efficacity, drop adverse medicine response, enhance patient compliance, reduce cost, time and clinical trials failure rate. individualized drug is a type of targeted treatment and it's helpful for wide diapason of conditions like lung cancer, brain excrescence, prostate cancer, rheumatoid arthritis, autoimmune conditions etc. This technology is also called for coming generation sequencing (NGS). It's an evolving field where croakers use some individual test for treating the case and after combining both tests and medical history of cases, they can fluently develop targeted drug for individual case.
A. Basics
Every person has a unique variation of the mortal genome. Although utmost of the variation between individualities has no effect on health, an existent's health stems from inheritable variation with actions and influences from the terrain. ultramodern advances in individualized drug calculate on technology that confirms a case's abecedarian biology, DNA, RNA, or protein, which eventually leads to attesting complaint. For illustration, personalized ways similar as genome sequencing can reveal mutations in DNA that impact conditions ranging from cystic fibrosis to cancer. Another system, called RNA seq, can show which RNA motes are involved with specific conditions. Unlike DNA, situations of RNA can change in response to the terrain. thus, sequencing RNA can give a broader understanding of a person's state of health. Recent studies have linked inheritable differences between individualities to RNA expression, restatement, and protein situations.
The generalities of personalized drug can be applied to new and transformative approaches to health care. Personalized health care is grounded on the dynamics of systems biology and uses prophetic tools to estimate health pitfalls and to design personalized health plans to help cases alleviate pitfalls, help complaint and to treat it with perfection when it occurs. The generalities of personalized health care are entering adding acceptance with the stagers Administration committing to personalized, visionary case driven care for all stagers. In some case personalized health care can be acclimatized to the luxury of the complaint causing agent rather of the case's inheritable luxury; exemplifications are medicine resistant bacteria or contagions.
PM aims to fete which interventions will be most effective on the complaint outgrowth of an affected existent grounded on environmental/ epigenetic ecology, and their inheritable and molecular geography. This encompasses the dimension of complaint predilection, webbing and early opinion, prognostic assessment, pharmacogenomic measures, and complaint course monitoring. All of these interventions might be suitable to target given populations limiting the burden of the complaint, and in some cases (8).
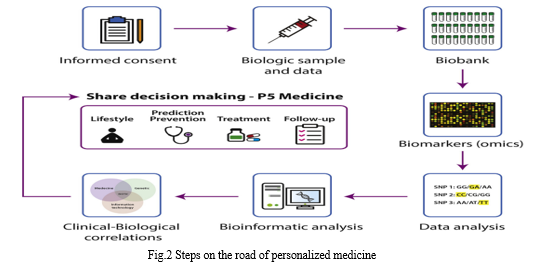
B. Application of Personalized Medicine
- Diagnosing disease earlier in development using optimal surveillance, thereby allowing more effective interventions or treatment options.
- Avoiding preventable drug related complications and side effects resulting from generic “one size fits all” drug prescribing.
- By ensuring appropriate drug is used and that the dosing regimen takes into consideration any genetic variants enhance the therapeutic efficacy which may affect metabolism of the drug.
- If someone is at increased risk of developing a disease, followed by promotion of and support for compliance with available prevention strategies.
C. Advantages of Personalized Medicine
- Decreased health care cost.
- Due to better targeted therapies, there will be higher probability to get desired outcomes.
- Mainly focus on prevention and prediction of diseases rather than reaction.
- Probability of negative side effects can be reduced.
- Disease intervention will be earlier in comparison to the past.
D. The Promise and Hype of Personalized Medicine
This account is, still, not the primary factor the final public would conceivably suppose after they hear of ‘individualized drug’. rather, the most specialize in the particular in customized drug would conceivably induce Associate in Nursing air of insolvable guarantees and prospect relating to drugs and coverings completely acclimatized to each individual person. The commitment nature of drug throughout this field is that the main target for the papers inside the first section of this volume.
The authors specialize in still clinical, business and indispensable sectors mention customized drug what guarantees area unit made; to whom area unit they made; will they be fulfilled; what drives the creating of pledges? still area unit we have got a fraudulent to assess whether or not or not substance, if it exists, is good, dangerous or just necessary thus on keep the show on the road? These queries area unit parade throughout a environment inside that a significant gap has surfaced between the pledge of progress created by business, analyzers and politicians on the one hand and jointly the verity of biomarker- grounded customized drug in analysis findings and clinical follow on the volition. This raises issues with every literal and current clinical significance.
E. An Elusive Goal
Biotechnology is leading the means in revamp the geography of medicines and thus the pharmaceutical business. Twenty- five times since the preface of recombinant mortal endocrine, biotechnology has gained instigation in driving inventions in medical specialty. Regenerative medicines and inheritable medicines square measure 2 similar exemplifications at the van of biotechnology. Biotechnology is not solely a force of rearmost medicines, still is also a motorist for revolutionizing medicine development.
VI. TESTING PERSONALIZED MEDICINES
Although we've argued that individualized drug is embedded in a great number of heritage perceptivity and literal precedents, substantially related to genetics and rare conditions, its recognition as a paradigm that should be embraced astronomically by the biomedical exploration and clinical communities is fairly recent. This suggests that not enough time has ceased since the time of this recognition for experimenters to show that individualized drug actually works in a wide enough variety of settings to motivate its broad relinquishment. In this light, questions of how the community can vet or test the mileage of individualized drug arise.
A. Digital Therapeutics and Personalized
App Content The ubiquity of smart phones has attracted the interest of numerous experimenters in the health professions as a vehicle for not only collecting health data through colorful apps but also to give advice, feedback, coaching, imagery, music, textbook- dispatches, or connections with other coffers, that could profit an individual with a particular condition or complaint. This has led to the emergence of the conception of a ‘digital remedial’; a smart phone app designed to treat and bring relief to an individual affected by a medical or cerebral condition. The content handed by a digital remedial app to an existent could vary depending on what's learned about that individual and his or her response to content handed in the app. In this way, the app can be substantiated. numerous digital rectifiers have experienced evaluation for their capability to engage druggies and profit them. The FDA has created guidelines for registering digital rectifiers as bona- fide, insurance- reimbursable, approved health technologies, and has begun assessing and approving numerous of them. The first approved digital remedial, an app for substance abuse, was approved by the FDA in 2017. How fluently digital rectifiers will be assimilated into the care sluice is an open question
Conclusion: The medical community is starting to benefit from pharmacogenomics. Despite widespread acceptance of pharmacogenomics' scientific value, the industry still has many doubters. Some claim that pharmacogenomics is too intricate. Some contend that despite the enormous promise of pharmacogenomics, people are also impatient in our quest to fulfill its potential. Pharmacogenomics is going to play a significant role in the future of medicine, but warns that due to the lengthy research and development processes in the field, we must exercise patience before reaping the rewards of pharmaceutical genomics. In the healthcare system, PM is regarded as innovative. The application of evidence-based medicine in the quickly evolving fields of medicine and healthcare after the completion of other and human genomics. The latest technologies based on genomes and Tools for bioinformatics provide enormous potential for the diagnosis is the revolution. The DNA-derived evidence that is available to healthcare professionals professionals, is reliable, precise, and tailored or restricted to the small number of patients groups. A relatively recent medical paradigm for categorizing, comprehending, treating, and preventing disease is called personalized medicine (PM). data and details regarding each person's biological and variations in the surroundings.
References
[1] Utilization of Pharmacogenetics in health case. [2] Fakruddin Md., Ahijit Chowdhury Pharmacogenomics- The promis of personalized medicine, Article in Bangladesh Journal of medicine science, DOI: 10.3329/bjms.v12i4.11041. [3] Cassandra White, Rodney Scott, Christine L paul, Stephen P Ackland.Pharmacogenomics in the era of personalized medicine.Priority Research centre for health behaviour ,University of Newcastle,NSW. [4] S. Marsh Washington University, Division of Molecular Oncology, St Louis, USA Pharmacogenomics Symposium Article, DOI: 10.1093/annonc/mdm289. [5] Sayali R. Gajare*, Amol S. Deshmukh, Chetana K. Shinde, Personalized Medicine, Dept. of Pharmaceutics, S.M.B.T College of Pharmacy, Dhamangaon, Nashik, India.DOI: 10.47583/ijpsrr.2021.v69i01.023. [6] EPA Europian Pharmaceutical Article https://www.europeanpharmaceuticalreview.com/article/1093/personalised-medicine-are-we-ready-for-the-revolution [7] Vijay Mishra, Puja Chanda, Murtaza M. Tambuwala, Ashish Suttee, Personlized Medicine: An review article International Journal of Pharmaceutical Quality Assurance 2019,DOI: 10.25258/ijpqa.10.2.13. [8] Personalized medicine Personalized medicine - Wikipedia [9] Juan MA, Rey CD, Bardey D, etal., Personalized Medicine. Closing the gap between knowledge and clinical practice, Autoimmunity Reviews, 2016;15(8):833-842. DOI NO: 10.1016/j.autrev.2016.06.005; PMID: 27302209 [10] Laura H.Goetz M.D.a, Nicholas J.Schork Ph.D.Personalized medicine: motivation, challenges, and progress,Fertility and sterility Article.
Copyright
Copyright © 2023 Prof. Gutte V. P, Kumbhar Shivam, More Mohan, Jadhav Prasad. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET57183
Publish Date : 2023-11-29
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

