Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- Conclusion
- References
- Copyright
Analysis of Non-Invasive Devices and Techniques Involved in Continuous Monitoring of Interstitial Glucose of Patients with Type 1 Diabetes
Authors: Aaditi Singhal, Prerna Singhal
DOI Link: https://doi.org/10.22214/ijraset.2023.57784
Certificate: View Certificate
Abstract
There are 422 million diabetes patients worldwide according to 2023 census of WHO, and around 100 million cases in India. 8.4 million type 1 diabetes cases were recorded as of 2021. By 2040, it is projected that the number of people living with Type 1 Diabetes will reach 13.5–17.4 million. The surge in diabetes cases has created the critical need for regular glucose monitoring to effectively manage this prevalent health issue. Currently, glucose levels are predominantly measured invasively by pricking the finger for a blood sample and involves invasive methods, such as fingertip pricks, which can be uncomfortable and inconvenient, particularly for paediatric patients. This method utilizes blood glucose monitoring devices, which measure sugar levels in a small blood sample placed on a disposable test strip and have a certain degree of inaccuracy. Patients do not test as often as they should because of the pain and hassle of finger pricks and many do not achieve optimal glycaemic control. However, the shift toward non-invasive continuous glucose monitoring is becoming increasingly imperative and a promising alternative. With current biotechnological advances, many techniques offer a non-invasive, continuous means of monitoring glucose levels and have garnered significant attention in recent years. The objective is to consolidate and summarize recent advancements in non-invasive continuous glucose monitoring, emphasizing integration into wearable platforms for seamless and real-time monitoring. Furthermore, paediatric patients with Type 1 Diabetes face elevated risks of severe hypoglycaemic and hyperglycaemic events due to challenges in glycaemic control. Frequently, monitoring blood glucose is crucial to mitigate these risks and achieve optimal glycaemic management. The objective of ongoing research is to validate AI-based algorithms utilizing ECG signals collected through non-invasive devices to detect glycaemic events. These advancements, once commercially available, have the potential to revolutionize glucose monitoring, offering a convenient, efficient, and less intrusive approach, particularly benefiting paediatric patients and improving overall healthcare management. Despite substantial research and development, challenges persist, including standardizing sweat collection methods, addressing sample degradation, accounting for variations in sweat composition among individuals, optimizing diverse detection methods, improving glucose detection sensitivity, and ensuring overall commercial viability. Overcoming these challenges is paramount to bridge the gap between research and market availability, paving the way for a technological revolution in glucose monitoring. In this study, we compared potential non-invasive glucose monitoring devices and techniques to evaluate the most accurate, pain-free, fast, and cost-friendly device. Upon examination and survey, we have theorized the drawbacks persisting in the existing devices and hypothesized techniques. Looking forward this study has a broader application in not only understanding the limitations and creating more accurate devices but also in continuous glucose monitoring for diabetic patient care.
Introduction
I. INTRODUCTION
With increase of diabetes patients, World Health Organization reported approximately 422 million individuals suffering from diabetes worldwide, there is an urgent need of fitting devices and technology to garner the increasing demand. Wearable and digital technologies have revolutionized the way individuals monitor their fitness and health conditions, offering non-invasive tracking of various physiological parameters like heart rate and physical activity. However, these technologies often lack the capability to quantify crucial biochemical parameters essential for managing various health conditions. For instance, hypoglycaemia, where blood glucose levels drop below the normal range, poses a risk for diabetic patients, especially after intense exercise. Similarly, diabetes, a chronic illness, is characterized by an abnormal increase in blood sugar levels, leading to severe damage to vital organs like the heart, blood vessels, eyes, and kidneys.
Understanding how glucose levels fluctuate in response to different foods, medications, or physical activity is critical. Continuous monitoring of blood glucose has significantly enhanced diabetes management, ultimately curbing the escalation of diabetes and hypoglycaemia cases.
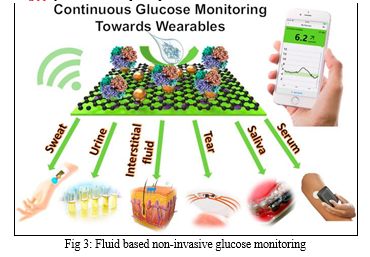
Minimally Invasive technologies involve extracting fluid from the body (tears, saliva, sweat, and interstitial fluid) to enzymatically measure glucose concentration. In invasive monitoring, glucose is directly detected in the blood. In non-invasive or minimally invasive methods, biological fluids containing glucose in concentrations correlating with blood are analysed. These alternative biofluids have become novel analytes of interest for painless glucose monitoring.
However, current BG tracking techniques are invasive, uncomfortable, and painful, typically relying on finger-prick tests using enzyme-based analysis. This method, while effective, demands strict compliance, which can be affected by factors like time constraints or pain. Moreover, it's not continuous, necessitating multiple tests daily to manage elevated glucose levels, especially after exercise, meals, or insulin dosing. Implantable glucose monitoring systems offer regular glucose monitoring but are invasive and may exhibit inaccuracies.
Thus, there is a high demand for a persistent, non-invasive glucose monitoring framework that can measure glucose levels without frequent calibrations.
While blood remains the most studied body fluid in invasive methods, non-invasive approaches require careful consideration to ensure accurate glucose concentration measurements from biofluids like tears, ISF, saliva, and sweat. Sweat-based glucose sensors are considered one of the least intrusive solutions for indirect blood sugar estimation.
This review article provides a comprehensive update on the state-of-the-art in continuous sweat glucose monitoring and its commercial prospects. It extensively covers sweat collection mechanisms and various sweat glucose sensing methods, focusing on detection and transduction. Considering the low levels of sweat glucose and the need for higher sensitivity, electrochemical sensing methods, mature from their use in BG sensors, exhibit significant potential for commercialization.
The study highlights recent breakthroughs in the development of non-invasive electrochemical glucose biosensors worn on the skin, emphasizing their prospects and limitations for enhanced glycaemic management.
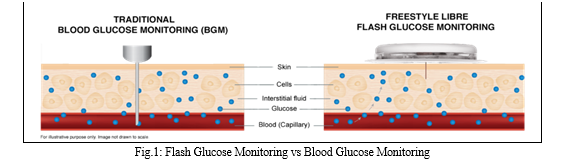
Table 1: Blood Glucose and ISG glucose sensing
|
glucose sensing in blood |
glucose sensing in ISF |
|
On the rise, the Blood Glucose value is greater than the Sensor Glucose that follows behind it. |
When moving down the tracks, the Blood Glucose in front is now less than the Sensor Glucose value. |
|
BGM provides a glucose value for the specific point in time [2] |
CGM gives you a more complete picture of where your glucose is going [2] |
|
Blood glucose readings tend to be about 5 to 10 minutes faster |
Lag time (Glucose first enters the bloodstream before being absorbed by the interstitial fluid. This means there may be a few minutes delay in your sensor (interstitial fluid) glucose readings compared with blood glucose readings) is longer. |
|
blood is (relatively) easily accessible |
ISF is tricky to access |
|
BG levels can be measured with a high reliability [1] |
ISF levels can be measured with a less reliability [1] |
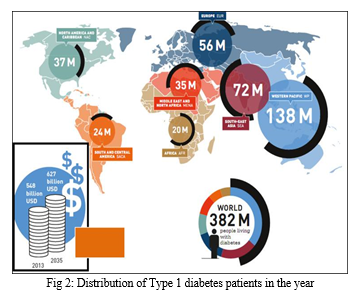
The primary target demographic for CGM technology remains Type 1 diabetes patients who require continuous monitoring of their blood glucose levels to effectively manage their condition.
II. MATERIALS AND METHODS
In this section, we provide a detailed account of the methodologies employed for our comparative study encompassing non-invasive Continuous Glucose Monitoring (CGM) systems. This entails a description of the CGM systems studied, both fluid-based and optical, as well as an overview of the methodologies adopted for reviewing the associated challenges. Generally, a CGM consists of Transmitter, Sensor, and Receiver / Reader. Limitations pertaining to CGMs are Magnetic imaging, CT scan, Diathermy (high frequency electrical heat), and Scuba diving - check with your respective CGM company for specific specs on water use.
Additionally, we outline the inclusion criteria, elucidate the data collection process, delineate the analysis techniques utilized, and expound on any statistical methods employed for a comprehensive understanding of our comparative study.
A. Non-Invasive CGM Systems Studied
Our study extensively focused on both fluid-based and optical non-invasive Continuous Glucose Monitoring (CGM) systems. The fluid-based systems involved methods such as sweat analysis, saliva analysis, and interstitial fluid (ISF) analysis. These approaches provided valuable insights into glucose levels without the need for invasive blood sampling.
In parallel, we explored optical methods which utilized various spectroscopic techniques to estimate glucose concentrations non-invasively. These included Raman spectroscopy, infrared spectroscopy, and other emerging optical technologies that hold promise for non-invasive glucose monitoring.
B. Methodologies for Reviewing Challenges
To comprehensively understand the challenges associated with non-invasive CGM systems, a rigorous review methodology was employed. This involved a thorough literature review of relevant research articles, scholarly publications, and established sources in the field of glucose monitoring technologies. The aim was to extract challenges, limitations, and advancements related to non-invasive CGM systems.
C. Inclusion Criteria
The inclusion criteria for selecting studies encompassed recent research articles, reviews, and publications focusing on non-invasive CGM technologies. Only studies published within a specified time frame were included to ensure relevance and up-to-date information. Additionally, emphasis was placed on studies with a strong experimental and analytical foundation.
D. stematic approach was employed for data collection. Pertinent information related to non-invasive CGM systems, challenges, and advancements was meticulously gathered from selected literature. This involved categorizing and organizing data to facilitate a structured comparative analysis.
E. Analysis Techniques
The gathered data was subjected to a comprehensive analysis, employing both qualitative and quantitative approaches. Qualitative analysis involved identifying patterns, trends, and recurring themes across the literature. Concurrently, quantitative analysis involves the statistical interpretation of relevant data to derive meaningful insights.
F. Statistical Methods
Statistical methods were employed to analyse quantitative data wherever applicable. This included measures of central tendency, variance analysis, and correlation analyses to ascertain relationships and trends within the collected data.
In summary, our methodological approach encompassed a thorough study of non-invasive CGM systems, a rigorous review of associated challenges, adherence to defined inclusion criteria, systematic data collection, and a judicious mix of qualitative and quantitative analyses to present a comprehensive comparative study.
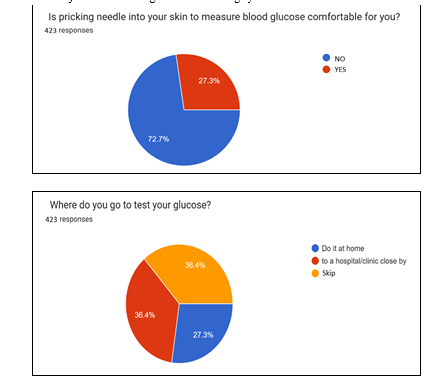
Survey conducted on Diabetic patients' view on glucose monitoring systems:
A total of 423 participants took the survey conducted in August 2023. There are 422 million diabetes patients worldwide according to 2023 census of WHO, and 8.4 million type 1 diabetes cases as per records of 2021. By 2040, it is projected that the number of people living with T1DM will reach 13.5–17.4 million.
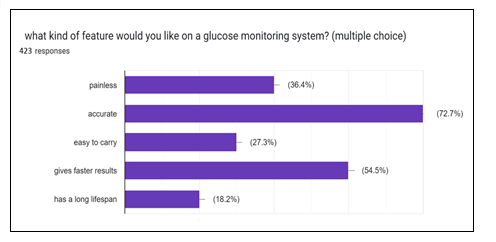
We conducted a survey to understand mass perspective and back up our claims through practical evidences. It is clearly evident that patients suffering from diabetes are looking for superior devices and often skip or try to avoid testing, which is problem. Not monitoring glucose levels at desired intervals can create sugar imbalance leading to deteriorating health.
Therefore, there is an urgent need of accurate, fast, pain-free, and easily accessible glucose monitoring systems. In all, the survey results are consistent with are objective for better glucose monitoring systems.
III. HYPOTHESIZED RESULTS
In this section, we delineate the anticipated outcomes and hypothesized results based on the methodologies employed in our comparative study of non-invasive Continuous Glucose Monitoring (CGM) systems. These predictions are derived from a careful consideration of the methods and techniques utilized.
A. Minimally-Invasive Glucose Monitoring
- A responsive hydrogel-based microneedle system
The patch consisted of a transparent substrate of photocurable resin and microneedles made of a pH-responsive and glucose-responsive hydrogel. The responsive hydrogel was composed of a photocrosslinkable hydrogel of gelatine methacrylate (GelMA) together with a pH-responsive nanogel (nano (CMC-pHEA)) and glucose oxidase (GOx).
The composite hydrogel showed fast response and high sensitivity to glucose levels in physiological range, mainly due to the ionization of CMC-pHEA component and proton balance. The microneedles showed sufficient mechanical strength to penetrate the skin of mice with minimal invasion, and achieved in situ extraction of glucose in interstitial fluid (ISF) and in situ glucose-responsive reaction. We demonstrated the rapid glucose monitoring by microneedle patch system in skin-mimicking gels in vitro and in diabetic mice in vivo. The microneedles quickly and sensitively responded to glucose concentrations, allowing quantitative readouts of glucose levels through the changes of microneedle heights and swelling ratios.
B. Fluid-Based Non-Invasive CGM Systems
- Sweat Analysis
We expect that the sweat-based non-invasive CGM systems will exhibit notable potential in accurately estimating glucose levels. The advancements in absorbent materials and microfluidic channels for effective sweat sampling are likely to enhance the sensitivity and specificity of the measurements. However, challenges related to sweat sample quantities and skin-surface contamination might affect the precision of readings, necessitating further refinement in sampling techniques.
2. Saliva Analysis
Saliva-based CGM systems are expected to provide a reliable estimation of glucose levels. The use of suitable sensing substances and advancements in the stability of sensors will contribute to enhanced accuracy. Nevertheless, challenges associated with dilution effects in saliva and the need for higher sensitivity may be encountered, demanding focused research in overcoming these obstacles.
3. Interstitial Fluid (ISF) Analysis
Analysis of interstitial fluid is anticipated to offer precise glucose level estimations owing to its proximity to blood glucose levels. The sensors designed for ISF analysis are expected to demonstrate a high degree of sensitivity and accuracy. Challenges related to invasiveness in obtaining ISF samples may, however, impact the widespread adoption of this approach.
a. Non-invasive monitoring of interstitial fluid lactate through an epidermal iontophoretic device a wearable, soft epidermal adhesive patch that integrates a reverse iontophoretic (RI) system, and an amperometric lactate biosensor placed on the anodic electrode with a porous hydrogel reservoir, for simultaneous ISF lactate extraction and quantification via electrochemical sensing, respectively. The iontophoretic system includes agarose hydrogels for preventing skin electrocution, while a porous polyvinyl alcohol-based hydrogel facilitates the effective transport of lactate from skin to the biosensor. The flexible skin-worn device tested on healthy individuals at rest showed rapid lactate collection from the ISF after 10 min of reverse iontophoresis with no evidence of discomfort or irritation to the skin.
Limitations: They claim to be non-invasive; they actually inject electrical current through the skin.
The sensors degrade over time and the technology is expensive.
4. Tear Analysis
Soft and transparent smart contact lenses which could detect glucose in tears with high sensitivity. The smart contact lenses were prepared by immobilizing a sensitive glucose fluorescent probe and another reference fluorescent dye into the hydrogel network of the contact lenses. With the increase of glucose concentration, the fluorescent colour of the smart contact lenses changed from pink to blue. The fluorescent images could be collected by a smartphone and transformed into RGB signals to quantify the glucose levels. These smart contact lenses could successfully monitor glucose level of 23 μM–1.0 mM in tears by a smart phone. The animal experiments further demonstrate the biosafety of smart contact lenses and the potential application of glucose monitoring. The fluorescence sensor platform is expected to be a new method for painless glucose monitoring. The detection limit of the contact lenses for glucose is as low as 9.3 μM by fluorescence spectrophotometer.
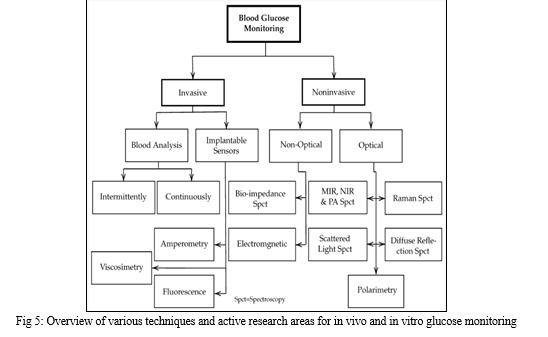
C. Optical Non-Invasive CGM Systems
- Raman Spectroscopy and Infrared Spectroscopy
Optical CGM systems employing Raman and infrared spectroscopy are likely to exhibit promising results. These spectroscopic techniques have the potential to provide accurate and real-time glucose measurements. Challenges related to calibration and specificity may be addressed through advancements in sensor technologies and calibration processes.
2. Chip less printable sensor based on split ring microwave resonators
The design and testing of a novel non-invasive wearable glucose monitoring sensor with zero power consumption and high sensitivity that is based on microwave planar resonator technology. The sensor is actually a metallic trace which could be taped over the skin. The impressive performance of the sensor, which removes many barriers against utilization of microwave resonator sensors for biomedical applications and especially wearable electronics, have been attained as the results of its improved design. Any electrolyte variation effects, over a physiological range of concentrations, resulted in a negligible frequency shift of the sensor. Also, the confounding effects of low to moderate dehydration was very low but became significant for severe dehydration.
3. Photoacoustic Method
A photoacoustic system has been developed using a single wavelength quantum cascade laser, lasing at a glucose fingerprint for non-invasive glucose monitoring. The system has been examined using artificial skin phantoms, covering the normal and hyperglycaemia blood glucose ranges. The detection sensitivity of the system has been improved to ±25mg/dL using a single wavelength for the entire range of blood glucose. Machine learning has been employed to detect glucose levels using photoacoustic spectroscopy in skin samples.
Artificial biomedical skin phantoms, having similar properties to real human skin, have been prepared to cover the normal and hyperglycaemia blood glucose range. The SNR of the system has been effectively enhanced by introducing acoustic absorption panels and pressure sensors. The pressure level applied to the skin phantoms plays a critical role in detecting glucose differences in the PA signals. The PA signals of the highest glucose concentration sample have to be lower than the amplification limit of the PA cell in order to detect the glucose differences.
4. Optical Coherence Tomography (OCT)
Optical coherence tomography (OCT)-based system for non-invasive, accurate, and continuous monitoring of blood (as opposed to interstitial) glucose concentration in subjects with diabetes. OCT uses low coherence light with precise depth focusing ability to measure changes in the microvasculature structure for glucose detection. They use light waves to take cross-section pictures of your retina. Future efforts will evaluate the accuracy of the system in the hypoglycaemic range.
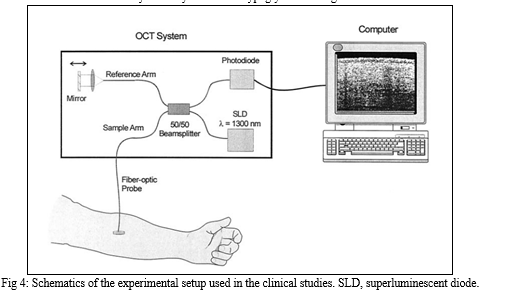
Table 2: Non-invasive CGM Systems
|
Optical non-invasive CGM systems |
Fluid based non-invasive CGM systems |
|
They utilize light-based techniques to measure glucose levels through the skin. |
They focus on sampling glucose from bodily fluids other than blood |
|
Limitations: accuracy and consistency due to skin pigmentation, tissue density, etc. |
Limitations: Accuracy as compared to blood glucose monitoring due to difference in glucose concentrations and dynamics in bodily fluids as compared to blood |
|
Examples: Raman Spectroscopy and Infrared Spectroscopy, Chip less printable sensor based on split ring microwave resonators, photoacoustic method, tomography, etc |
Examples: Tear analysis, sweat analysis, Interstitial Fluid analysis, saliva analysis, etc. |
D. Comparative Study Predictions
Based on our thorough comparative study, we anticipate that both fluid-based and optical non-invasive CGM systems will present their own set of advantages and challenges. Fluid-based systems might excel in terms of ease of use and continuous monitoring, while optical systems may offer higher precision and real-time data. The choice of the most suitable CGM system will depend on the specific requirements and preferences of individuals, considering factors such as accuracy, invasiveness, and ease of integration into daily life.
In conclusion, our hypothesized results align with the innovative potential of non-invasive CGM systems. The forthcoming outcomes of our comparative study are expected to shed light on the advancements and challenges within these technologies, steering the field towards improved glucose monitoring solutions.
IV. DISCUSSION
A. Challenges and Opportunities in Wearable Sweat Analysis
The analysis of sweat presents a valuable avenue for non-invasive monitoring of various biomarkers. However, it comes with its set of challenges and potential opportunities for improvement within the domain of wearable technology.
B. Limited Sample Quantities
The current methods of inducing sweat often yield limited quantities, necessitating intense exercises or iontophoresis. Even in these cases, the secretion rates may fall short, especially in inactive settings. Addressing this limitation requires the development of sensors that can efficiently function at lower sweat levels. Moreover, innovative and efficient biomarker extraction methods are essential to overcome this constraint.
C. Reducing Skin-Surface Contamination
Contamination from the skin and its surroundings significantly impacts the accuracy of sensor readings. Efforts to isolate sweat from the skin surface, such as using a protective layer, show promise in mitigating this challenge. Additionally, careful consideration of sampling methods, ensuring minimal sliding of sensors on the skin, and maintaining close sensor-skin contact can effectively minimize contamination.
Wearable sweat glucose sensors typically have a limited operational lifespan, typically around 14 days. Prolonging the sensor's shelf life is essential for cost-effectiveness and practicality. Enhancements in bioreceptor stability and accuracy, potentially through innovative materials and bioengineering, can contribute to longer sensor longevity.
D. Technological Challenges
- Large-Scale Sensor Manufacturing: Developing cost-effective and scalable manufacturing techniques is imperative for widespread adoption.
- Stability of the Sensor: Maintaining stability in non-invasive enzymatic sweat glucose sensors is crucial to ensure accurate and reliable readings over extended periods.
- Reusability and Longevity: Exploring novel materials and manufacturing techniques to enhance adhesives and ensure longer sensor reusability and durability.
- Specificity and Sensitivity: Ultra-sensitive sensors, coupled with pre-concentration technologies, are necessary to overcome the challenge of diluted sweat and maintain specificity in biomarker detection.
- Various Sweat Analyte Extensions: Future wearable sensors should be capable of monitoring a broader range of sweat analytes to enhance their utility and applications.
E. Addressing Calibration Challenges
Implementing robust auto-calibration systems based on extensive testing is crucial. These systems must be capable of adapting to environmental variations, individual differences, and lifestyle factors that can influence sweat composition and sensor readings.
- Dynamic Relationship between Blood Glucose and Sensor Signal: The dynamic and potentially time-varying relationship between capillary blood glucose and subcutaneous sensor signals introduces uncertainty into the accuracy of the blood glucose estimator.
- Lag Time and Closed-Loop Challenges: The time lag between blood and interstitial fluid glucose measurements could impact the real-time responsiveness of closed-loop systems. Delays in detecting changes in blood glucose levels may lead to suboptimal control and increased risk of hypoglycaemia or hyperglycaemia.
- Sensor Longevity and Biocompatibility: The current technology faces issues and have a general time span of 14 days along with sensors irritability to various skin types.
- Portable device: not all systems yet can be carried easily or around all the time.
- Minimally Invasive devices discomfort: still cause discomfort or irritation during skin penetration.
- Accuracy, calibration and consistency: can be encountered due to various reasons like skin pigmentation, tissue density, difference in glucose concentrations and dynamics in bodily fluids, etc.
- Availability and costs: Not all systems are available in the market at low cost and there is comparatively very less awareness and knowledge about the devices that are available in the market.
In conclusion, tackling these challenges will pave the way for the successful commercialization of wearable sweat-sensing devices. As technology advances and these hurdles are overcome, wearable sweat devices hold the potential to revolutionize bio detection, enabling more personalized and predictive healthcare. Further research and innovation in this domain are essential to realize the full potential of sweat analysis in wearable technologies.
V. ACKNOWLEDGEMENT
We would like to express our gratitude to Dr. Roshan Padmanabhan, Senior Bioinformatics Scientist with a Ph.D. in Infectious Disease and Bioinformatics from Aix-Marseille University, France, for mentoring us throughout the course of our research and for the vital and consistent guidance and instruction throughout the research. Additionally, we extend our heartfelt thanks to our families for believing in us and supporting our academic and scientific journey.
Conclusion
In this comprehensive review, we\'ve delved into the realm of non-invasive continuous glucose monitoring (CGM), with a focal point on sweat-based CGM while briefly exploring other non-invasive techniques. Wearable sweat devices present a convenient and continuous means to monitor crucial electrolytes and metabolites. This is achieved through innovative sampling approaches like modified absorbent materials, super hydrophobic/super hydrophilic surfaces, or epidermal microfluidic channels. Recent years have witnessed a substantial surge in research towards real-time detection of varying concentrations of sweat analytes. Advancements in manufacturing processes and materials science have allowed the integration of multiple sensors with on-site circuits and wireless data transmission into flexible multiplex systems. Customized materials, such as nanofibers or nanoparticle-modified electrodes, have significantly improved sensor performance, boasting high sensitivity, low limits of detection (LoD), and a wide linear range. Doping with conductive nanoparticles has proven effective, especially in creating non-enzymatic electronic sensors with superior LoDs, sensitivity, and stability compared to enzyme sensors. Sweat, with its array of metabolites and electrolytes, holds promise for monitoring various significant health conditions. However, to make meaningful medical applications, in vivo validation experiments are imperative to establish the correlation of sweat analytes with blood readings. Integrated wearable devices have now transcended mere sweat collection and can induce iontophoresis for sweat stimulation, eliminating the need for collection and even administering on-demand blood glucose medication for hypoglycaemia. While novel sampling methods enhance sensor sensitivity, hurdles remain for real-time, non-invasive sweat monitoring in future applications. The review has outlined the benefits and limitations of various sweat sampling methods, shedding light on optical and electromechanical approaches. A critical need exists for introducing calibration-free sensors associated with specific diseases to enhance the usability of these devices in integrated multiplexed systems. As of now, wearable sweat devices for clinical applications have not yet made their commercial debut, primarily due to these limitations. Looking ahead, the trajectory is set towards creating wearables that can detect multiple analytes in sweat simultaneously. Recent designs of wearable sweat sensors showcase the potential to test various analytes of interest using an array of biosensors. The next frontier involves achieving simultaneous and multiplex scanning to capture the full spectrum of biomarkers accurately. Implementing auto-calibration techniques, validated through extensive testing, is essential to address the impact of environmental factors and individual variations on sensor results. These limitations, while challenging, underscore the immense promise that wearable sweat glucose sensors hold. They call upon researchers to redouble efforts, propelling these wearable sensors into the commercial domain. Beyond the electrochemically based sensing approach, the collective aim is to advance biological detection, providing tailored, predictive, real-time healthcare, and point-of-care services. Addressing these challenges is the key to unlocking the potential of non-invasive wearable sweat technologies.
References
[1] Gabbay2008OpticalCT, Optical coherence tomography-based continuous noninvasive glucose monitoring in patients with diabetes, Robert A. Gabbay and Surendra Sivarajah, Diabetes technology & therapeutics, 2008 [2] Baghelani, M., Abbasi, Z., Daneshmand, M. et al. Non-invasive continuous-time glucose monitoring system using a chipless printable sensor based on split ring microwave resonators. Sci Rep 10, 12980 (2020) [3] Aloraynan, A.; Rassel, S.; Xu, C.; Ban, D. A Single Wavelength Mid-Infrared Photoacoustic Spectroscopy for Noninvasive Glucose Detection Using Machine Learning. Biosensors 2022, 12, 166. [4] Siegmund T, Heinemann L, Kolassa R, Thomas A. Discrepancies Between Blood Glucose and Interstitial Glucose-Technological Artifacts or Physiology: Implications for Selection of the Appropriate Therapeutic Target. J Diabetes Sci Technol. 2017 Jul;11(4):766-772. [5] Alva, S., Brazg, R., Castorino, K. et al. Accuracy of the Third Generation of a 14-Day Continuous Glucose Monitoring System. Diabetes Ther 14, 767–776 (2023). [6] Mengyu Deng, Guangjie Song, Ke Zhong, Zhanchen Wang, Xi Xia, Yanqing Tian, Wearable fluorescent contact lenses for monitoring glucose via a smartphone, Sensors and Actuators B: Chemical, Volume 352, Part 2,2022,131067, ISSN 0925-4005, [7] Rishikesh Pandey, Santosh Kumar Paidi, Tulio A. Valdez, Chi Zhang, Nicolas Spegazzini, Ramachandra Rao Dasari, and Ishan Barman Accounts of Chemical Research 2017 50 (2), 264-272 [8] Afeef, S.; Tolfrey, K.; Zakrzewski-Fruer, J.K.; Barrett, L.A. Performance of the FreeStyle Libre Flash Glucose Monitoring System during an Oral Glucose Tolerance Test and Exercise in Healthy Adolescents. Sensors 2023, 23, 4249. [9] Ajjan R, et al. Adv Ther 2019;36:579-596. [10] American Diabetes Association. Standards of medical care in diabetes—2020. Diabetes Care. 2020;43(1): S77-S88. [11] Brixner D, et al. Clinical Therapeutics 2019;41(2):303-313. [12] Foster NC, et al. Diabetes Technol Ther 2019;21(2):66-72. [13] Lee WC, et al. J Med Econ 2014;17(3):167-175. [14] Unger J, et al. Postgraduate Medicine 2020;132:305-313. [15] Vincze G, et al. Diabetes Educ 2004;30(1):112-125. [16] Wagner J, et al. J Diabetes Technol Ther 2005;7(4):612-619.
Copyright
Copyright © 2024 Aaditi Singhal, Prerna Singhal. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET57784
Publish Date : 2023-12-28
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

