Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Introduction
- Conclusion
- References
- Copyright
Asthma: A Comprehensive Outlook
Authors: Mr. Rakesh Dnyaneshwar Wagh, Miss. Pratiksha Khade, Dr. Hingane. L. D.
DOI Link: https://doi.org/10.22214/ijraset.2022.39893
Certificate: View Certificate
Abstract
Introduction
I. INTRODUCTION
Our current understanding of the pathophysiology of asthma and the availability of potent, effective therapies mean that asthma can be well controlled. However, to achieve this goal, optimal therapy must be prescribed and the patient must be taught how and when to use it. Pharmacists, as part of the health care team, help improve the pharmacologic management of asthma by teaching patients about their medications, how to use them, and the importance of using them as prescribed. Alerting physicians to suspected problems, such as under using anti-inflammatory therapy or overusing inhaled bronchodilators, will provide an opportunity for the physician to consider changes in a patient's management plan when appropriate. Acting in these educational and information-sharing roles, pharmacists contribute to improving the control of asthma and enabling patients to live full, active, and productive lives.
II. DEFINITION
Asthma is a chronic, episodic disease of the airways, and it is best viewed as a syndrome. In 1997, the National Heart, Lung, and Blood Institute (NHLBI) included the following features as integral to the definition of asthma, recurrent episodes of respiratory symptoms; variable airflow obstruction that is often reversible, either spontaneously or with treatment; presence of airway hyper reactivity; and, importantly, chronic airway inflammation in which many cells and cellular elements play a role, in particular, mast cells, eosinophils, T lymphocytes, macrophages, neutrophils, and epithelial cells. All of these features need not be present in any given asthmatic patient. Although the absolute "minimum criteria" to establish a diagnosis of asthma is not known or widely agreed upon, the presence of airway hyper reactivity is a common finding in patients with current symptoms and active asthma.
A. WHO Definition
Asthma is a chronic disease characterized by recurrent attacks of breathlessness and wheezing, which vary in severity and frequency from person to person. Symptoms may occur several times in a day or week in affected individuals, and for some people become worse during physical activity or at night. During an asthma attack, the lining of the bronchial tubes swell, causing the airways to narrow and reducing the flow of air into and out of the lungs. Recurrent asthma symptoms frequently cause sleeplessness, daytime fatigue, reduced activity levels and school and work absenteeism. Asthma has a relatively low fatality rate compared to other chronic diseases.
III. EPIDEMOLOGY
According to World Health Organization (WHO) estimates, 300 million people suffer from asthma and 255 000 people died of asthma in 2005.
Asthma is currently a worldwide problem, with increasing prevalence in both children and adults. Total prevalence is estimated to be 7.2% of the world's population (6% in adults, 10% in children). An hospital based study on 20,000 children under the age of 18 years from 1979,1984,1989,1994 and 1999 in the city of Bangalore showed a prevalence of 9%, 10.5%, 18.5%, 24.5% and 29.5% respectively. The increased prevalence correlated well with demographic changes of the city. Further to the hospital study, a school survey in 12 schools on 6550 children in the age group of 6 to 15 years was undertaken for prevalence of asthma and children were categorized into three groups depending upon the geographical situation of the school in relation to vehicular traffic and the socioeconomic group of children. Group I-Children from schools of heavy traffic area showed prevalence of 19.34%, Group II-Children from heavy traffic region and low socioeconomic population had 31.14% and Group III-Children from low traffic area school had 11.15% respectively. (P: I & II; II & III <0.001). A continuation of study in rural areas showed 5.7% in children of 6-15 years. The persistent asthma also showed an increase from 20% to 27.5% and persistent severe asthma 4% to 6.5% between 1994-99 .
Asthma is found in all countries but it is more prevalent in industrialized countries than in low-income countries. A recent survey estimates that in New Zealand, 25% of children from 13 to 14 years of age have asthma symptoms, 16% in the USA, 13% in Europe and Latin America and 10% in African cities.
The total number of people with asthma, however, is already higher in the developing world than in the industrialized countries. There are approximately 3 million asthmatics in Japan and in France, compared to an estimated more than 15 million in India and over 30 million in Africa.
IV. MORTALITY
Asthma was not generally considered to be a fatal illness and this was the teaching in medical schools well into the present century. It was not until the rise in deaths from asthma in the 1960s that attitudes began to change.
The increasing death rate during the 1980s has been particularly alarming. As shown in the following figure.
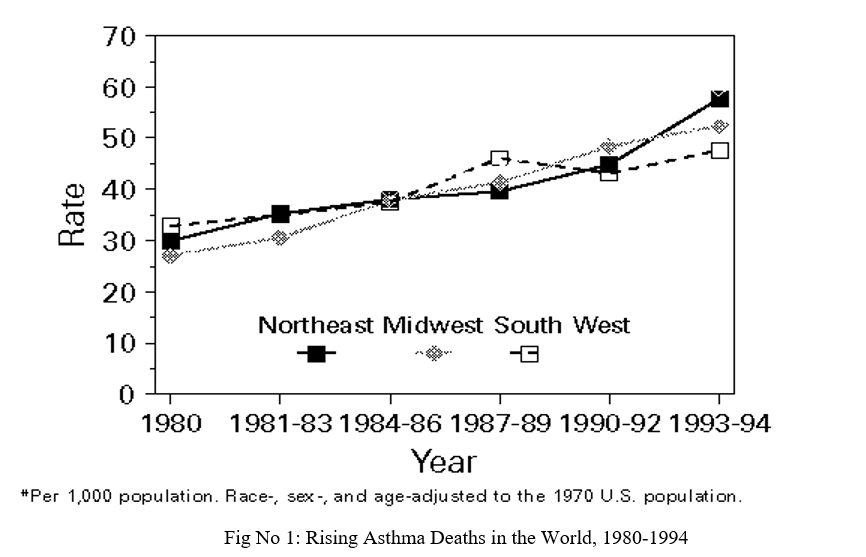
V. MORBIDITY
About 60% of all asthmatics visit their physician at least once a year regarding their condition. Office visits doubled from 1975-1994 (see table below). Emergency department (ED) visits and hospitalizations are also increasing, with 466,000 hospitalizations in 1993 and 1.9 million ED visits in 1995.
VI. ETIOLOGY
The complete causes of asthma are unknown. Heredity does seem to play a role, as do allergens and environmental factors. According to the latest Expert Panel Report (EPR) in 1997 from the National Heart, Lung, and Blood Institute's National Asthma Education and Prevention Program, "Atopy, the genetic predisposition for the development of an IgE-mediated response to common aeroallergens, is the strongest identifiable predisposing factor for developing asthma."
There are two categories of asthma: allergic or extrinsic and idiosyncratic or intrinsic. Allergic asthma is a result of an antigen\antibody reaction on mast cells in the respiratory tract. This reaction causes the release of inflammatory mediators from mast cells, which elicit the clinical response associated with an asthma attack. Idiosyncratic asthma is a result of neurological imbalances in the autonomic nervous system (ANS) in which the alpha and beta-adrenergic as well as the cholinergic sites of the ANS are not properly coordinated. Onset of asthma between the ages of 5 to 15 years usually indicates asthma with an allergic basis.3
Studies suggest a genetic basis for airway hyper responsiveness, including linkage to chromosomes 5q and 11q. However, asthma clearly does not result from a single genetic abnormality, but is rather a complex multigenic disease with a strong environmental contribution. For example, allergic potential to inhalant allergens (dust mites, mold spores, cat dander, etc) more commonly is found in asthmatic children as well as asthmatic adults whose asthma began in childhood, compared with adult-onset asthmatics.
Exposure to environmental allergens can trigger asthma symptoms. Among the most common allergens are microscopic droppings of dust mites and cockroaches, airborne pollens and molds, plants and plant proteins, enzymes, and pet dander (minute scales of hair, feathers, or skin). Exposure to a variety of occupational irritants (e.g., vapors, dust, gases, fumes, tobacco smoke, air pollution) also can worsen or cause asthma.
Certain medications may trigger asthma symptoms. These include beta-blockers, used to treat high blood pressure, heart disease, and glaucoma (in eye drops). About 5% to 20% of adults with asthma have attacks triggered by sensitivities or allergies to medications such as aspirin, ibuprofen, indomethacin, and naproxen. Others react to sulfites (chemicals commonly used to preserve foods such as tuna, salads, dried apples and raisins, and beverages such as lemon juice, grape juice, and wine).
Other factors that may contribute to asthma or worsen symptoms include sinus infections, gastro esophageal reflux disease (GERD), pregnancy, menstruation, and even the time of day. Asthma also can be induced by exercise or cold air.
- Respiratory Infection: Respiratory syncytial virus (RSV), rhinovirus, influenza,parainfluenza, Mycoplasma pneumonia
- Allergens: Airborne pollens (grass, trees, weeds), house-dust mites, animal danders, cockroaches, fungal spores.
- Environment: Cold air, fog, ozone, sulfur dioxide, nitrogen dioxide, tobacco smoke, wood smoke.
- Emotions: Anxiety, stress, laughter.
- Exercise: Particularly in cold, dry climate
- Drugs/Preservatives: Aspirin, NSAIDS (Cyclooxygenase inhibitors), sulfites, benzalkonium chloride, Beta-blockers
- Occupational Stimuli: Bakers (flour dust); farmers (hay mold); spice and enzyme workers; printers (Arabic gum);
Chemical workers (azo dyes, anthraquinone, polyvinyl chloride); plastic, rubber and wood workers; (Formaldehyde, western cedar, dimethylethanolamine, anhydrides)
VII. PATHOPHYSIOLOGY
Airway inflammation is the primary problem in asthma. An initial event in asthma appears to be the release of inflammatory mediators (e.g., histamine, tryptase, leukotrienes and prostaglandins) triggered by exposure to allergens, irritants, cold air or exercise. The mediators are released from bronchial mast cells, alveolar macrophages, T lymphocytes and epithelial cells. Some mediators directly cause acute bronchoconstriction, termed the "early-phase asthmatic response." The inflammatory mediators also direct the activation of eosinophils and neutrophils, and their migration to the airways, where they cause injury. This so-called "late-phase asthmatic response" results in epithelial damage, airway edema, mucus hyper secretion and hyper responsiveness of bronchial smooth muscle (Figure No 2 ). Varying airflow obstruction leads to recurrent episodes of wheezing, breathlessness, chest tightness and cough.
According to the current view, several inflammatory cells interact in a complex manner and release multiple inflammatory mediators that act on various target cells in the airways to produce the characteristic pathophysiology of asthma.
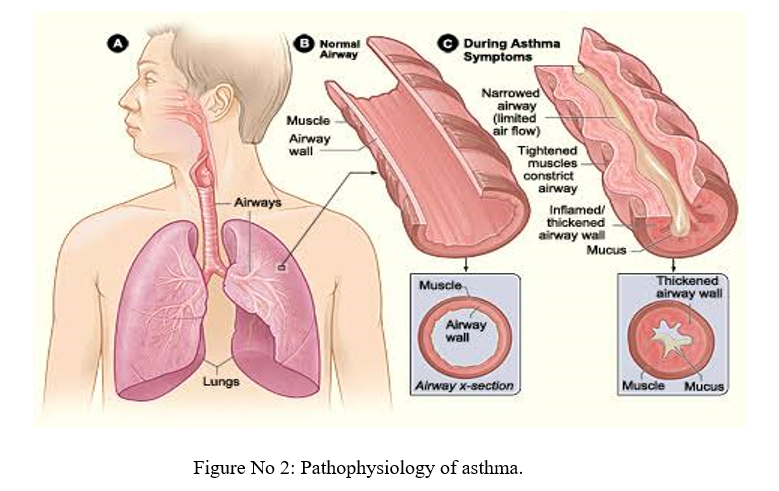
VIII. CLASSIFICATION
A. Mild Intermittent Asthma
Symptoms of cough, wheeze, chest tightness or difficulty breathing less than twice a week
Flare-ups-brief, but intensity may vary
Nighttime symptoms less than twice a month
No symptoms between flare-ups
Lung function test FEV1 equal to or above 80 percent of normal values
Peak flow less than 20 percent variability AM-to-AM or AM-to-PM, day-to-day.
B. Mild Persistent Asthma
Symptoms of cough, wheeze, chest tightness or difficulty breathing three to six times a week
Flare-ups-may affect activity level
Nighttime symptoms three to four times a month
Lung function test FEV1 equal to or above 80 percent of normal values Peak flow less than 20 to 30 percent variability.
C. Moderate Persistent Asthma
Symptoms of cough, wheeze, chest tightness or difficulty breathing daily
Flare-ups-may affect activity level
Nighttime symptoms 5 or more times a month
Lung function test FEV1 above 60 percent but below 80 percent of normal values Peak flow more than 30 percent variability.
D. Severe Persistent Asthma
Symptoms of cough, wheeze, chest tightness or difficulty breathing continual
Nighttime symptoms frequently
Lung function test FEV1 less than or equal to 60 percent of normal values Peak flow more than 30 percent variability.
The level of asthma severity will determine the types of medicine required to get asthma under control.
Another type of classification commonly seen is
- Chronic asthma
- Acute severe asthma
- Allergic asthma
- Exercise induced asthma
- Nocturnal asthma
IX. DIAGNOSIS
A diagnosis of asthma usually is based on the patient's symptoms, medical history, a physical examination, and laboratory tests that measure pulmonary (lung) function. Doctors typically look for signs that the patient's airflow is obstructed and that the obstruction is at least partially reversible.
Factors that trigger symptoms may be evident, such as exercise, cold air, and exposure to an allergen; however, the precipitating factors may not be clearly identified.
Evidence of reversible airway obstruction is often detected in the physical examination or by physiologic testing. Physiologic testing generally is recommended to confirm the diagnosis. During an asthma attack, wheezing can be heard by listening to the chest with a stethoscope. The airway obstruction is considered reversible if the wheezing disappears in response to treatment, or when the suspected triggering factor is removed or resolved.
A. Spirometry
B. Peak Expiratory flow
C. Bronchial Provocation
D. Other Tests
Spirometry uses a measuring device called a spirometer that is connected by a flexible tube to a disposable cardboard mouthpiece. The patient exhales and inhales deeply, then seals his or her lips around the mouthpiece and blows as forcefully and for as long as possible until all the air is exhaled from the lungs.
Ideally, the patient should exhale for at least 6 seconds. The spirometer measures the amount of air exhaled and the length of time it took to exhale it. The amount of air exhaled in the first second, expressed as "FEV1," is measured and compared to the total amount exhaled. If the amount exhaled in 1 second is disproportionately low to the total exhaled, the patient has an obstruction. To test for reversibility, the patient then inhales a bronchodilator (i.e., a drug that widens the airways in the lungs) and the spirometry is repeated. If the values of the test performed after administration of the bronchodilator are significantly better than the prebronchodilator values, the obstruction is considered reversible.
Sometimes a patient with asthma does not demonstrate reversibility after the inhalation of a bronchodilator. In this case, the patient may be treated for a few weeks with anti-inflammatory medications and then returns for another spirometry test. If the post-treatment spirometry results are better than the initial results, the obstruction is considered reversible.

Because asthma symptoms vary, it is not unusual for a patient with chronic asthma to have normal spirometry. In such cases, peak expiratory flow (PEF) rate monitoring may be used to demonstrate reversible airway obstruction. A peak flow meter is a portable device that can be carried by the patient. It consists of a small tube with a gauge that measures the maximum force with which one can blow air through the tube. The patient performs the peak flow meter test twice a day for about 2 weeks and records the results for review in a follow up appointment. The first test should be performed after waking in the morning, before taking bronchodilator medications. The patient should perform the peak expiratory flow maneuver 3 times and record the highest measurement. The second test should be done in the afternoon or early evening after taking a bronchodilator. Peak flows vary during the day and the early morning peak is lower than the evening peak. A variability greater than 20% indicates a reversible airway obstruction.
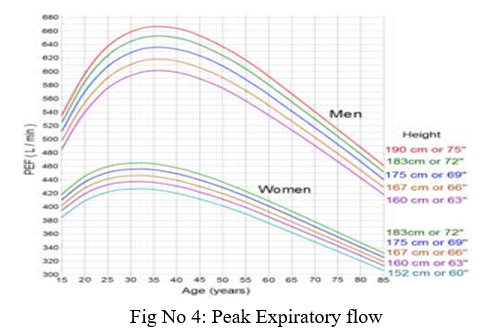
Occasionally, a patient with a suspected asthma-related airway obstruction does not demonstrate obstruction in spirometry or peak flow monitoring. In this circumstance, the diagnosis of airway obstruction may be provided by bronchial provocation.
Bronchial provocation, also known as bronchoprovocation and bronchial challenge, identifies and characterizes hyperresponsive airways by having the patient inhale an aerosolized chemical, called a broncho-spastic agonist that triggers a hyperresponsive reaction. The chemicals most often used are histamine and methacholine.
Patients perform spirometry without inhaling the agent and then inhale increasingly higher doses of the agent. After each incremental dose inhalation, spirometry is performed. Patients who demonstrate a reduction in FEV1 of 20% with a low dose of methacholine or histamine have nonspecific hyperresponsiveness. Although some patients without asthma demonstrate hyperresponsiveness, most patients with a positive reaction have asthma.
The other common bronchoprovocation test is the exercise challenge test, which is used primarily with patients whose asthma is triggered by exercise. The patient performs spirometry and then exercises, usually on a treadmill or exercise cycle. The exercise test should resemble as closely as possible the conditions under which the symptoms are usually triggered. After the patient exercises, spirometry is repeated. This may be done several times, immediately after exercise and periodically, until there is a drop in the FEV1 greater than 20% or until 30 minutes have elapsed.
Tests may be employed to exclude other diseases and to evaluate conditions that worsen the asthmatic condition. These include the following:
Chest x-rays are often obtained initially to rule out other health conditions.
Allergy testing, either by skin testing or by measuring antibodies in the blood, sometimes is performed to determine if the asthma is allergy induced, and if so, what specific allergens are involved.
X-rays of the sinuses is often done to exclude sinusitis as a factor.
Evaluation for gastroesophageal reflux disease is often performed to evaluate its contribution to the control of asthma.
Episodic symptoms of airflow obstruction
- Difficulty breathing
- Chest tightness
- Cough (worse at night)
Symptoms occurring or worsening at night, awakening the patient
Symptoms occurring or worsening with exercise, viral infections, changes in weather, strong emotions, or menses; or in the presence of animals, dust mites, mold, smoke, pollen, or chemicals
Wheezing
Airflow obstruction at least partially reversible
Diurnal variation in PEF of more than 20 percent over one to two weeks
Increase of at least 12 percent and 200 mL in FEV1 after bronchodilator use (indicates reversibility)
Reduced FEV1 and FEV1/FVC ratio using spirometry (indicates obstruction)
PEF = peak expiratory flow; FEV1 = forced expiratory volume in one second; FVC = forced vital capacity.
X. SYMPTOMS
People with asthma have symptoms when the airways are narrowed (bronchospasm), swollen (inflamed), or filled with mucus. Common symptoms of asthma include:
A. Coughing, especially at night
B. Wheezing
C. Shortness of breath
D. Chest tightness, pain, or pressure
The symptoms might also vary from one asthma episode to the next, being mild during one asthma episode and severe during another. Mild asthma episodes are generally more common. Usually, the airways open up within a few minutes to a few hours. Severe episodes are less common, but last longer and require immediate medical help. It is important to recognize and treat even mild symptoms to help you prevent severe episodes and keep asthma in better control.
XI. COMPLICATIONS
Those with asthma are at increased risk of developing problems associated with acid reflux, including the development of gastroesophogeal reflux disease. Avoiding acid reflux can be aided by avoiding food or drink for several hours prior to bedtime and sleeping with the head slightly elevated.
A. Pharmacotherapy
For completeness, this section on the primary prevention of asthma should mention pharmacological trials of treatments designed to prevent onset of the disease. Children given ketotifen (206 infants, in two trials) showed significantly less asthma at one and three-year follow-up compared with those receiving placebo. In the third study, using cetirizine, Months' treatment had no effect in the intention to treat population but significantly reduced asthma in children with atopic dermatitis sensitised to either grass pollen or house dust mite. Cetirizine had additional benefits for atopic dermatitis alone and reduced the frequency of urticaria.
B. Classes of Drugs
A classification of asthma drugs based on current knowledge of their mode of action is represented.
- Preventors: Anti-inflammatory
- Relievers: Short-acting bronchodilators that provide acute relief of symptoms
- Controllers: A sustained bronchodilator action with unproven or mild anti-inflammatory action
Prescribers should be acquainted with the trade names, formulations, dosage and mode of administration of each preparation. In general, duplication of drugs within one group should be avoided. Combinations such as the regular use of controllers like long-acting b2 agonists (Salmeterol or Formoterol) with a short-acting b2 agonist as rescue medication may be used and are discussed below. The combination of a short-acting b2 agonist inhaler with ipratropium bromide is not recommended for routine use in asthma.
The chlorofluoro carbons (CFC) propellants in pressurised metered dose inhalers (MDIs) are currently being replaced with alternatives like hydrofluoroalkanes (HFA) as part of the global strategy to protect the atmospheric ozone layer.
Conclusion
Asthma is a complicated disease with a multitude of clinical presentations. The exact defect in asthma has not been defined, and it may be that asthma is a common presentation of heterogenous group of diseases. Asthma is defined and characterized by excessive reactivity of the bronchial tree to a wide variety of noxious stimuli. The reaction is characterized by bronchospasm, excessive mucus production, and inflammation. The central role of inflammation in inducing and maintaining BHR is now becoming widely appreciated and studied. The goal of asthma therapy is to normalize, ass much as possible, the patient\'s life and prevent chronic irreversible lung changes. Drugs are the mainstay of asthma therapy. The goal of drug therapy is to use the minimum amount possible to completely control the disease. In chronic asthma, therapy should be aimed at both bronchospasm and inflammation in order to produce the best results. Patients should be followed and nonitored diligently for toxicities. Although death from asthma is an uncommon event, the most common cause of death is underassessment of the severity of obstruction either by the patient or by the clinician; the next common cause is undertreatment. A corner stone of any therapy is education and the realization that most asthma deaths are avoidable.
References
[1] Lugogo, N., Que, L.G., Fertel, D., Kraft, M.,2010. Asthma. In: Mason, R.J., Broaddus, V.C., Martin, T.R., (Ed.) Murray & Nadel\'s Textbook of Respiratory Medicine. Saunders Elsevier, Philadelphia. 5th Edn. pp. 258-267. [2] Brozek, J.L., Bousquet, J., Baena-Cagnani, C.E., Bonini, S., Canonica, G.W., Casale, T.B., 2010. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J. Allergy Clin. Immunol. 126(3), 466-76. [3] National Asthma Education and Prevention Program Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma.Rockville, MD. National Heart, Lung, and Blood Institute, US Dept of Health and Human Services, 2007. NIH publication 08-4051. [4] Wechsler, M.E., 2009. Managing asthma in primary care: putting new guideline recommendations into context. Mayo Clin. Proc. 84, 707-717. [5] Fanta, C.H., 2009. Asthma. N. Engl. J. Med. 360, 1002-1014. [6] Turner MO, Taylor D, Bennett R, FitzGerald JM. A randomized trial comparing peak expiratory flow and symptom self-management plans for patients with asthma attending a primary care clinic. Am J Respir Crit Care Med 1998;157(2):540-6. [7] Sommaruga M, Spanevello A, Migliori GB, Neri M, Callegari S,Majani G. The effects of a cognitive behavioural intervention in asthmatic patients. Monaldi Arch Chest Dis 1995;50(5):398-402. [8] Cowie RL, Revitt SG, Underwood MF, Field SK. The effect of apeak flow-based action plan in the prevention of exacerbations of asthma. Chest 1997;112(6):1534-8. [9] Kohler CL, Davies SL, Bailey WC. How to implement an asthma education program. Clin Chest Med 1995;16(4):557-65. [10] Bailey WC, Richards JM, Jr., Brooks CM, Soong SJ, Windsor RA, Manzella BA. A randomized trial to improve self management practices of adults with asthma. Arch Intern Med 1990;150(8):1664-8. [11] Murphy VE, Gibson PG, Talbot PI, Kessell CG, Clifton VL.Asthma self-management skills and the use of asthma education during pregnancy. Eur Respir J 2005;26(3):435-41. [12] Shah S, Peat JK, Mazurski EJ, Wang H, Sindhusake D, Bruce C, et al. Effect of peer led programme for asthma education in adolescents: cluster randomised controlled trial. BMJ 2001;322(7286):583-5. [13] Guevara JP, Wolf FM, Grum CM, Clark NM. Effects of educational interventions for self management of asthma in children and adolescents: systematic review and meta-analysis.BMJ 2003;326(7402):1308-9. [14] Griffiths C, Foster G, Barnes N, Eldridge S, Tate H, Begum S,et al. Specialist nurse intervention to reduce unscheduled asthma care in a deprived multiethnic area: the east London randomised controlled trial for high risk asthma (ELECTRA). BMJ 2004;328(7432):144. [15] Powell H, Gibson PG. Options for self-management education for adults with asthma. Cochrane Database Syst Rev2003(1):CD004107. [16] Gibson PG, Powell H, Coughlan J, Wilson AJ, Abramson M,Haywood P, et al. Self-management education and regular practitioner review for adults with asthma. Cochrane Database Syst Rev 2003(1):CD001117. [17] Haby MM, Waters E, Robertson CF, Gibson PG, Ducharme FM. Interventions for educating children who have attended the emergency room for asthma. Cochrane Database Syst Rev 2001;1.
Copyright
Copyright © 2022 Mr. Rakesh Dnyaneshwar Wagh, Miss. Pratiksha Khade, Dr. Hingane. L. D.. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET39893
Publish Date : 2022-01-11
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

