Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- Conclusion
- References
- Copyright
Clinicoradiological Correlation of Covid19 Patients in Western Uttar Pradesh, India: A Descriptive Study
Authors: Dr. Yasmeen Usmani
DOI Link: https://doi.org/10.22214/ijraset.2021.39411
Certificate: View Certificate
Abstract
A pilot study of 150 patients at premier medical institute of western Uttar Pradesh, INDIA. The purpose of this pictorial review article is to describe the most common manifestations and patterns of lung abnormality on CXR in COVID-19 in order to equip the medical community in its efforts to combat this pandemic. The varied spectra of COVID-19 presentation included fever, cough, shortness of breath, sore throat etc. Diabetes mellitus, hypertension, COPD/K-Chest and CAD were found as major comorbid conditions. Symptomatic presentation of COVID-19 was observed to be higher in patients with co morbid disease, especially if multiple. HRCT chest in COVID-19 patients had a major diagnostic and prognostic importance as positive CT findings were more prominent in symptomatic patients and co-morbid patients. Clinical symptoms of patients directly correlated with CT severity index. CT imaging was found to be useful in predicting clinical recovery of patients or progression of disease. Introduction: COVID-19 (coronavirus disease 2019) is a highly infectious disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), declared as a pandemic on 11th March 2020. The chest imaging findings are nonspecific and most commonly show atypical or organizing pneumonia, often with a bilateral, peripheral and bi-basal predominant distribution. Our study is concerned with the data of COVID positive patients admitted in the institute for the period of March 16- May 17, 2020. Aims and Objectives 1) To correlate clinical and radiological spectra of covid positive patients and their final outcome. 2) To describe the spectrum of lung parenchyma changes in the symptomatic as well as asymptomatic in COVID- 19 patients. Review of literature: This case report series presents a summary of key findings frequently associated with COVID-19, which will assist radiologists and clinicians in preliminary clinical evaluation (PCE). Materials and Methods: The data for the study is sourced from clinically suspected patients from the Covid Ward, LLRM Medical College, Meerut,(U.P.),INDIA which were subjected to chest radiography on 60mAh portable X-Ray machine. The patients are followed up to correlate the findings with clinical outcome. The study has been conducted on a minimum of 150 patients with portable Chest X-Ray machine. Observations & Discussion: The most frequent findings encountered are airspace opacities are viz- Hazy pulmonary opacities, Bilateral lower lobe consolidations, Peripheral air space opacities, Uncommon CXR findings, Diffuse air space disease. Conclusion: Based on our study, few inferences have been deduced; A significant proportion of the clinically symptomatic cases shows characteristic radiological changes on chest X-ray and also how chest radiography can be used as a tool not to substitute but supplement RTPCR in evaluation of COVID positive cases.
Introduction
I. INTRODUCTION
COVID-19 (coronavirus disease 2019) is a highly infectious disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The World Health Organization (WHO) originally called this illness "novel coronavirus-infected pneumonia (NCIP)", and the virus itself had been provisionally named "2019 novel coronavirus (2019-nCoV)". The origin of first case was reported from Wuhan; China, in December 2019 and subsequently there was a rapid global spread resulting it into being declared as a pandemic on 11th March 2020. The first case reported in India was in Thrissur, Kerala on January 29,2020. India has confirmed (needs update 101139 COVID cases with 3163 deaths (as at May 19, 2020) according to the Indian Council of Medical Research, India data.
Confirmed cases in the United States in May, 2020 have exceeded 200,000 with more than 4,400 deaths as per the online virus tracker created by The Lancet, and hosted by John Hopkins University. Radiographers, patient facing, frontline health professionals, have a key role in the diagnosis and management of COVID-19. Diagnosis of SARS-CoV-2 is confirmed by reverse transcription polymerase chain reaction (RT-PCR) of nasopharyngeal swabs. However, sensitivity is variable, reported to be 70% to 90% on initial swab and 90% on second swab at 72 h.
The staff in a medical imaging department is some of the first people to come in contact with COVID-19 patients and therefore clear infection control guidelines are extremely important for an imaging facility. Droplet-type precautions including medical mask, gown, gloves, and eye protection N95 masks and aprons should be donned routinely because of COVID-19.
II. REVIEW OF LITERATURE
COVID-19 (Corona Virus Disease-19) is a zoonotic illness first reported in China in December of 2019, linked to a seafood wholesale market in the city of Wuhan, the capital city of Hubei province . On March 11, 2020, COVID-19 was declared a global pandemic by World Health Organization (WHO), having rapidly spread by human to human contact across 177 territories, in 6 continents.
The radiological findings of COVID-19 on chest X-ray are those of atypical pneumonia [7] or organizing pneumonia [5,10]. Though chest CT scans are reported to be more sensitive than Chest X-rays, chest radiography still remains the first line imaging modality of choice used for patients with suspected COVID-19 because of it being cheap, readily accessible and can easily be sanitized. For ease of decontamination the use of portable radiography units are preferred. Chest radiographs are often normal in early or mild disease.
According to a study Of the patients with COVID-19 requiring hospitalization 69% had an abnormal chest radiograph at the initial time of admission, and 80% had radiographic abnormalities sometimes during hospitalization. The findings are reported to be most extensive about 10-12 days after symptom onset.
The most frequent radiographic findings are airspace consolidation or, less commonly, ground-glass opacity (GGO). The distribution is most often bilateral, peripheral, and lower zone predominant. Unlike parenchymal abnormalities, pleural effusion is rare (3%).
According to the Center for Disease Control (CDC), even if a chest CT or X-ray suggests COVID-19, viral testing is the only specific method for diagnosis. In addition CDC also said,’With the COVID-19 pandemic threatening to overwhelm healthcare systems globally, chest X-ray radiographs should be considered a useful tool for identifying COVID-19’.
Preliminary clinical evaluation (PCE) by radiologists & clinicians at time of image acquisition is an expected competency of practitioners in many regions of the World including India, the United States of America, the United Kingdom and Australia. As radiologists are almost invariably the first practitioner to see the diagnostic image, it follows that a radiologist’s PCE and triage for an immediate clinical report plays a vital role in identifying possible COVID-19 patients.
There are increasing case reports of patients presenting to hospital without classical symptoms of COVID-19 (fever, cough), including abdominal symptoms and may be referred for non-COVID diagnostic workup without respiratory precautions in place. Rapid radiologists’ PCE and triage will facilitate prompt reporting of the investigation, aid patient diagnosis and management decisions in a timely way.
This rapid triage also allows for the potential of all imaging to be performed during a single hospital attendance and, more crucially, immediate appropriate decontamination of imaging equipment. It is crucial that radiographers, radiologists and referring clinicians are aware that a normal imaging investigation (CXR or CT) does not exclude COVID-19 in high risk patients. Thus, a ‘completion’ chest CT to identify COVID-19 when the lung bases are normal on a routine CT abdomen in a patient who has no COVID-19 respiratory symptoms is not advocated.
Also, personal protective equipment (PPE) and infection control precautions should continue, based on clinical suspicion. When imaging is abnormal, findings are frequently non-specific and need to be incorporated with the relevant clinical symptoms and findings on blood tests (most notably elevated C-reactive protein (CRP) and lymphopenia <1100 m/L)
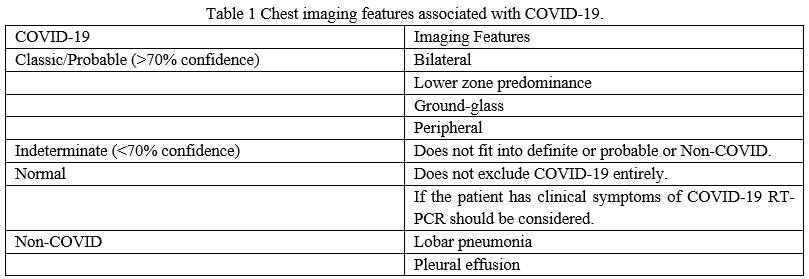
This case report series presents a summary of key findings frequently associated with COVID-19 and will assist radiologists PCE. Chest imaging features associated with COVID-19 (ref BSTI reporting template) are presented in Table 1.
Common clinical symptoms of patients infected with COVID-19, include fever, fatigue, dry cough, nasal congestion, runny nose, sore throat, and diarrhea. In severe cases, patients present with dyspnea and / or hypoxemia one week after the onset of the disease, and rapidly deteriorate to acute respiratory distress syndrome, septic shock, metabolic acidosis and coagulation abnormalities.
It was found that there was no statistical difference in clinical features in patients with COVID-19 pneumonia and those with non-COVID-19 infection except for leukocyte and platelet counts. Patients with positive reverse transcription polymerase chain reaction (RT-PCR) results had lower median leukocyte and platelet counts than those with negative results. Although viral nucleic acid detection using RTPCR remains the gold standard of diagnosis, imaging may play a vital role in reinforcing the diagnosis, can assess disease progression, and identify complications that may need additional procedures or changes in management. This case series aims to outline the clinical features, illustrates the most common reported imaging findings of COVID-19 infection, and demonstrates different management plans used.
III. RADIOGRAPHIC FEATURES
The Centers for Disease Control (CDC) does not currently recommend CXR or CT to diagnose COVID-19. Viral testing remains the only specific method of diagnosis. Confirmation with the viral test is required, even if radiologic findings are suggestive of COVID-19 on CXR or CT.
The primary findings of COVID-19 on chest radiograph and CT are those of atypical pneumonia or organizing pneumonia.(Table-1)
However imaging has limited sensitivity for COVID-19, as up to 18% demonstrate normal chest radiographs or CT when mild or early in the disease course, but this decreases to 3% in severe disease. Bilateral and/or multilobar involvement is common.
The current recommendation of many learned societies and professional radiological associations is that imaging should not be employed as a screening/diagnostic tool for COVID-19, but reserved for the evaluation of complications.
Although less sensitive than chest CT, chest radiography is typically the first-line imaging modality used for patients with suspected COVID-1997. For ease of decontamination, use of portable radiography units is preferred.
Chest radiographs may be normal in early or mild disease. Of patients with COVID-19 requiring hospitalization, 69% had an abnormal chest radiograph at the initial time of admission, and 80% had radiographic abnormalities sometime during hospitalization. Findings are most extensive about 10-12 days after symptom onset .
The most frequent findings are airspace opacities, whether described as consolidation or, less commonly, GGO. The distribution is most often bilateral, peripheral, and lower zone predominant.
One of the most unique and somewhat specific features of COVID-19 pneumonia is the high frequency of peripheral lung involvement, often mirroring other inflammatory processes such as organizing pneumonia. It was reported that 33% of COVID-19 chest CTs had peripheral lung distribution and an even greater incidence of up to 86% on chest CT
A. Peripheral Lower zone Consolidations(U/L,B/L)
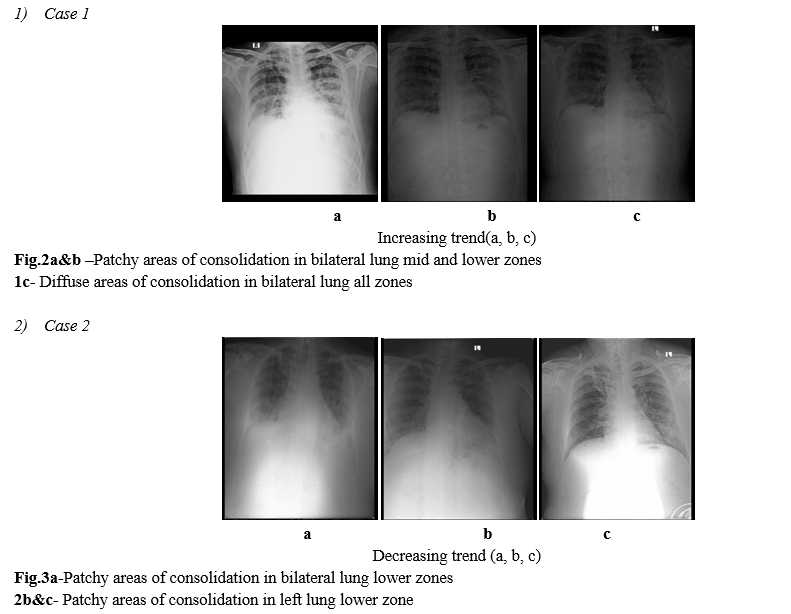
CXR is a less sensitive modality in the detection of COVID-19 lung disease compared to CT, with a reported baseline CXR sensitivity of 69%. The most common reported CXR and CT findings of COVID-19 include lung consolidation and ground glass opacities. Ground glass densities observed on CT may often have a correlate that is extremely difficult to detect on CXR (Figs. 1, 2).
Often, reticular opacities accompanying regions of ground glass attenuation are more easily appreciable on standard CXR
B. Peripheral Middle-lower zone consolidations (U/L,B/L)
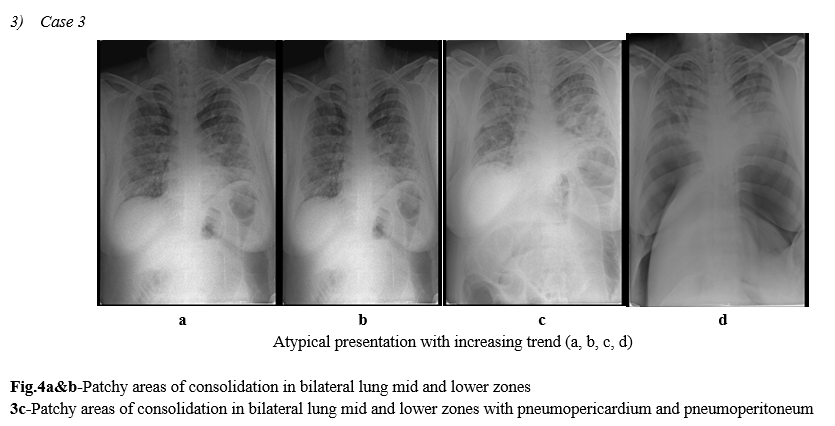
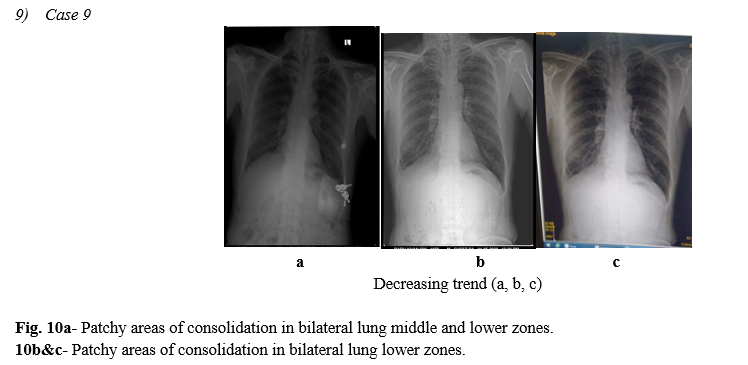
As opposed to community acquired bacterial pneumonia which tends to be unilateral and involving a single lobe, COVID-19 and other viral pneumonias typically produce lung opacities in more than one lobe. Identifying multifocal air-space disease on CXR can be a significant clue to COVID-19 pneumonia.(FIG.3,4) Early COVID-19 investigators have noted that the air-space disease tends to have a lower lung distribution and is most frequently bilateral.(ref.1)
C. Diffuse Air Space Disease
Diffuse lung opacities in patients with COVID-19 have a similar CXR pattern (Fig. 7) as other widespread infectious or inflammatory processes including acute respiratory distress syndrome (ARDS).
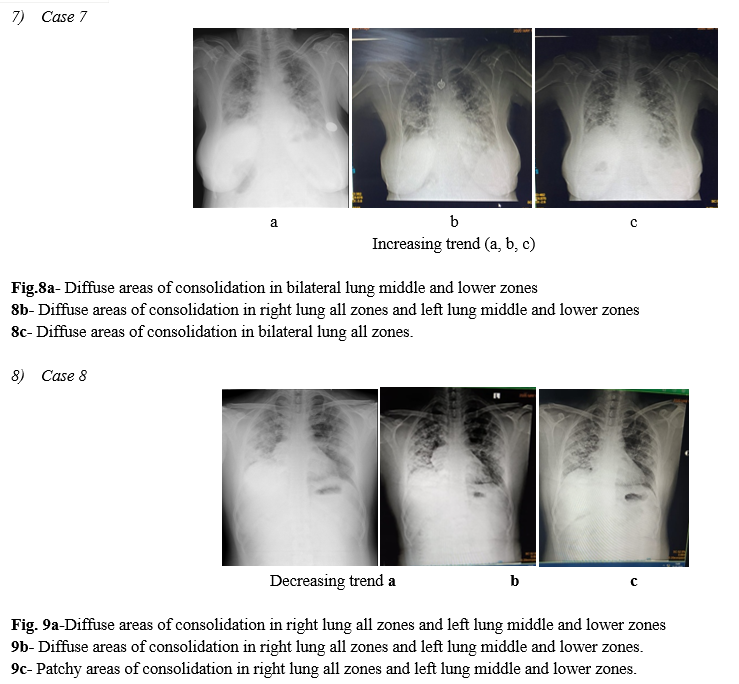
When lung disease involves the majority of the pulmonary parenchyma, patients are typically hypoxic and require intubation with mechanical intubation (Fig. 8).
D. Atypical/Uncommon CXR findings
Pleural effusions have been reported as exceedingly rare on CXR and CT in COVID-19 infected patients, and when present are most often identified late in the disease course.
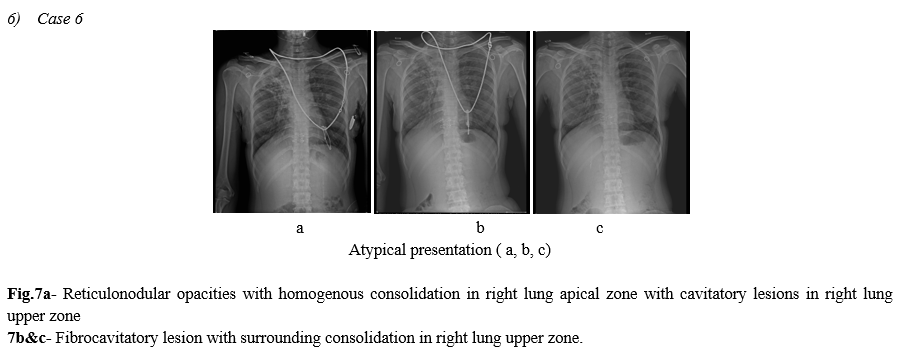
Lung cavitation and pneumothorax are also rare findings in COVID- 19 patients but can occur (Fig. 11).
Localized large nodules have yet to be reported in the literature to this date.
Diffuse chest wall subcutaneous emphysema and pneumomedias- tinum after intubation in the setting of COVID-19 infection has been described in one case report.(ref.2)
IV. AIMS AND OBJECTIVES
- To correlate clinical and radiological spectra of covid positive patients and their final outcome.
- To describe the spectrum of lung parenchyma changes in the symptomatic as well as asymptomatic in COVID- 19 patients.
V. MATERIALS AND METHODS
The main source of data for the study are clinically suspected patients from the Covid Ward, LLRM Medical College, Meerut undergoing imaging in Department of Radio diagnosis, LLRM Medical College, Meerut.
All patients admitted in covid ward, LLRM Medical College, Meerut were subjected to chest radiography on Portable X-Ray machine. The patients are followed up to correlate the findings with clinical outcome.
The study will be conducted on a minimum of 150 patients with portable Chest X-Ray machine. The patient will be followed up to co relate the findings with clinical outcome.
A. Inclusion criteria
All covid positive patients admitted in the hospital.
B. Exclusion criteria
Clinically positive and radiologically negative patients.
C. Machine Used: Portable X-ray machine.
D. CR System: Fujifilm Table top CR system, FCR Prima
VI. OBSERVATION AND DISCUSSION
COVID-19, a member of the Beta coronavirus Genus, is an enveloped, single stranded RNA virus. It is the seventh member of the family of coronaviruses infecting humans, along with the zoonosis middle east respiratory syndrome- coronavirus (MERS-CoV) and severe acute respiratory syndrome coronavirus (SARS-CoV) 1 . The COVID-19 outbreak has resulted in a global health emergency, with morbidity and mortality exceeding the outbreaks of SARS in 2003 and MERS in 2012. (ref.3)Despite radiologic similarities to SARS and MERS pneumonia, significantly fewer number of patients with COVID-19 infection have abnormalities on the initial chest radiographs 7–9 . Chest radiographs remain the initial imaging tool of choice but have a limited role in the diagnosis of disease. It was found that consolidation was the most common finding on chest radiographs in COVID-19 patients with a peripheral, lower zone predominance 10 . The typical features are peripheral bilateral GGOs, rounded GGOs and reverse halo sign of organizing pneumonia (OP).
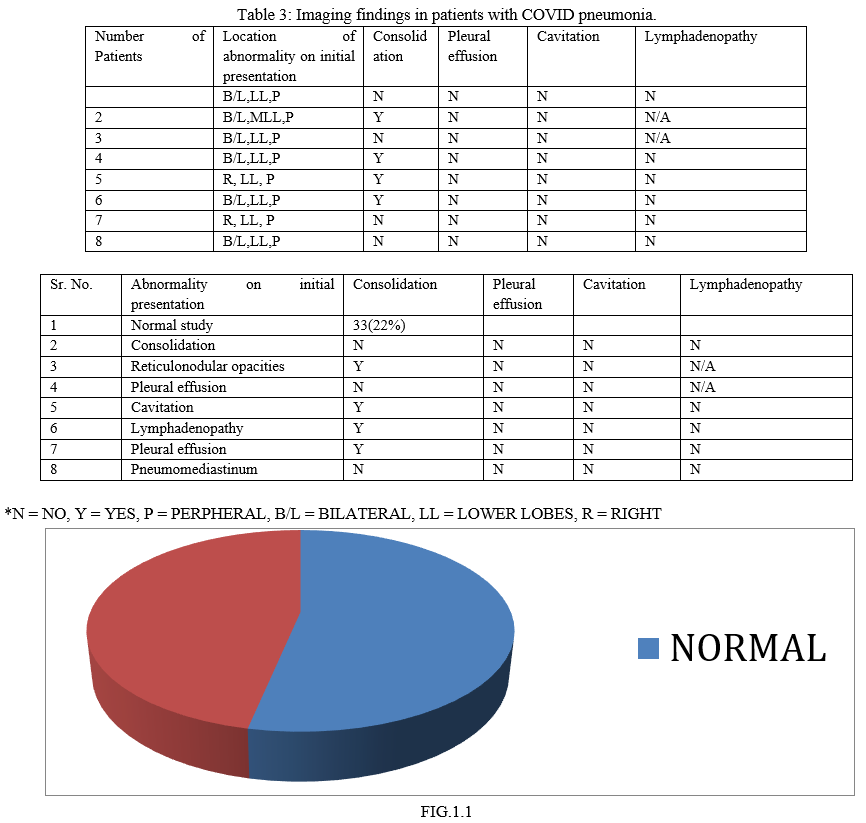
Indeterminate features include multifocal, diffuse, perihilar or unilateral GGOs with non-rounded, non-peripheral distribution. Atypical features include isolated consolidations, tree-in-bud opacities, cavitation and smooth interlobular septal thickening with pleural effusion. CT can be used to better assess the extent of disease, identify complications and monitor treatment response12. In the early stages of the disease, the abnormalities on CT are localized to the sub pleural or peri-bronchovascular regions of one or both lungs, and manifest as pure GGOs with or without vascular enlargement 13 . Disease progression is associated with increasing GGOs, and multilobar involvement 14 . Progression to bilateral consolidations is often seen in hospitalized patients 15, due to development of ARDS. Interlobular septal thickening, crazy-paving pattern and air bronchograms are common. Pleural effusion and mediastinal lymphadenopathy are rarely seen and most likely favor alternative etiologies.(Table-3)
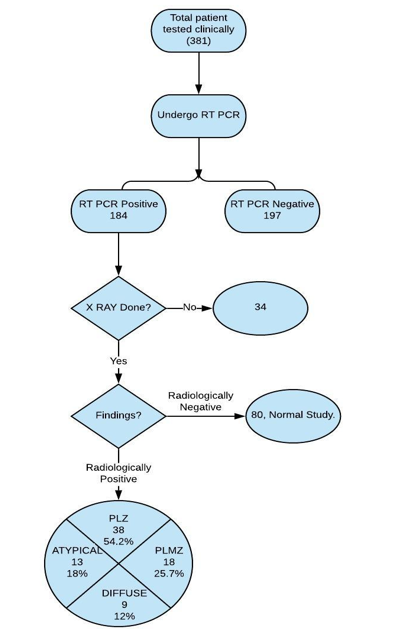
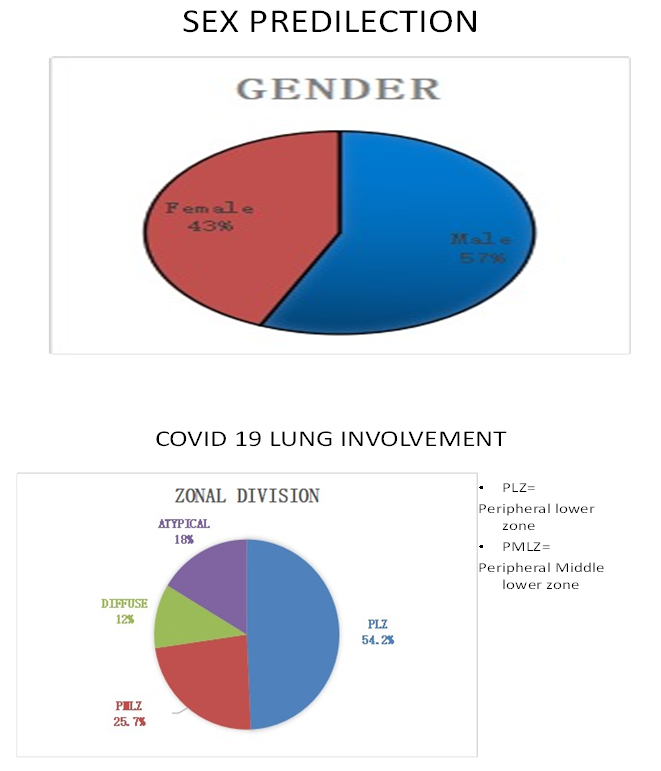
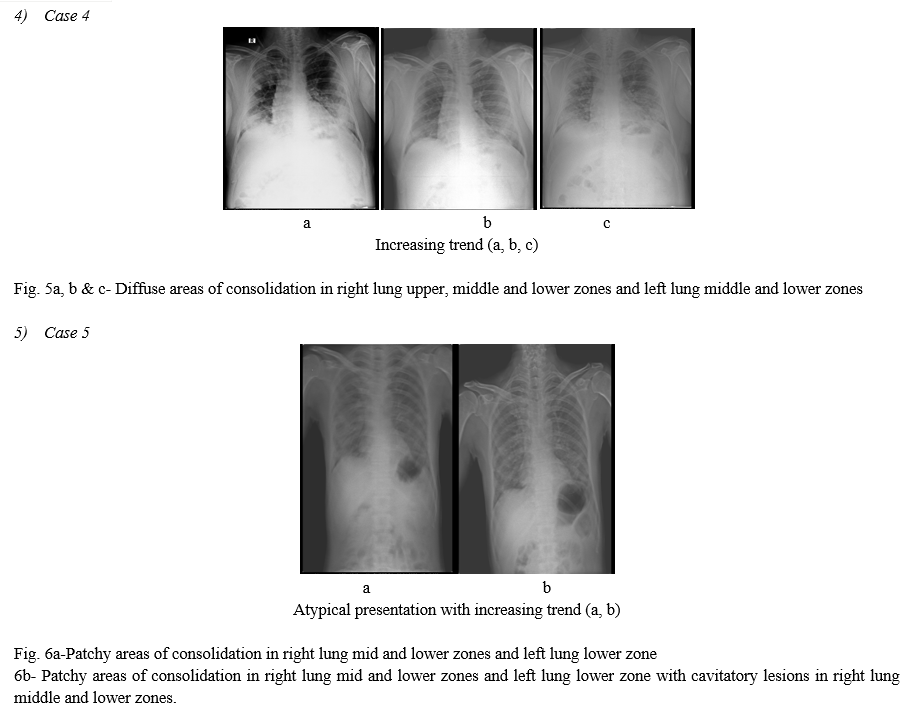
Our 150 patient case series (Table 1) (64 females, 86 males) included patients who acquired the infection from travel and community spread. 7 of the 150 patients expired from respiratory and non-respiratory issues, and the remaining individuals are responding to treatment. Associated co-morbidities were present in few of the patients. In addition to the commonly reported imaging manifestations (Table 2), which include patchy peripheral GGOs with lower lobe predominance,(FIG.5,6) we encountered one patient with a pneumothorax, and asymmetric involvement at initial presentation. Pattern of GGOs and consolidative opacities seen in COVID-19 patients can mimic those of other viral pneumonias, particularly influenza, and organizing pneumonia due to other causes such as bacterial infection, drug toxicity, inhalation injury, connective tissue disease, and idiopathic. Imaging features can also be seen synchronously with chronic abnormalities like granulomatous disease or malignancies 16. This case series hopefully adds to the knowledge base that is evolving and helps in the understanding of this relatively new and unknown viral pandemic.(ref.4)


VII. TYPICAL PATIENTS
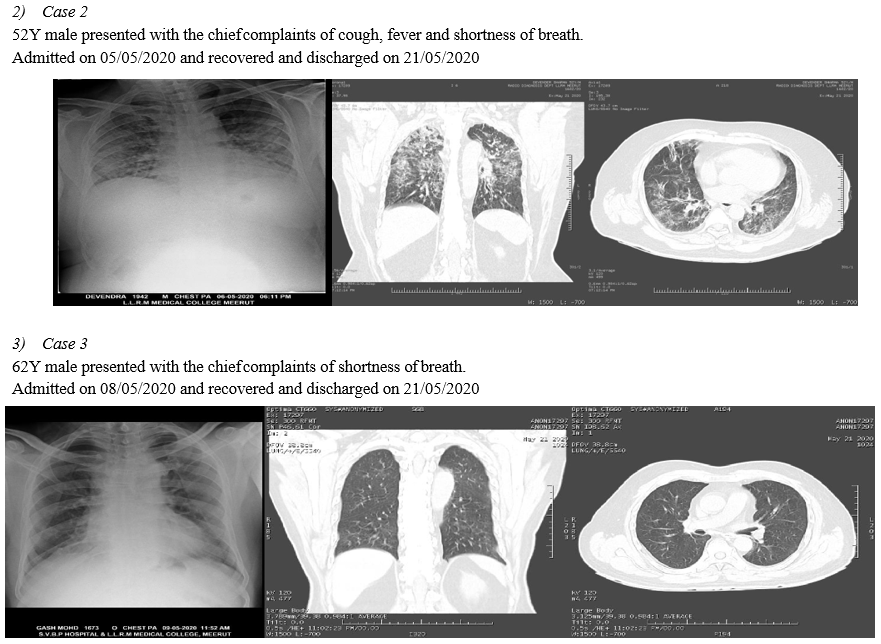
A. CT Chest of RT-PCR Negative Patients
In 10 Symptomatic RT-PCR negative patients HRCT THORAX is done, in the context of typical clinical presentation and exposure history, patients present with negative results of RT-PCR for COVID-19 but have characteristic imaging features of COVID-19 on chest CT. Thus, in patients at high risk for COVID-19, chest CT evidence of viral pneumonia may precede negative RT-PCR test results and present as an important warning signal. Imaging examination (CHEST RADIOLOGY AND CHEST CT) has become the indispensable means not only in the early detection and diagnosis but viral nucleic acid testing is an important diagnostic criterion; however, it has some limitations. False negatives from viral nucleic acid testing arise from the uneven quantity of detection technology, disease characteristics (asymptomatic patients), and status of epidemic prevention and control, as well as errors in clinical sampling. The challenges in identification of pathogens by viral nucleic acid testing and able to overcome the problem of overlapping structures forming composite shadows as well.(Ref.5)
VIII. CHEST IMAGING OF RT-PCR NEGATIVE PATIENTS

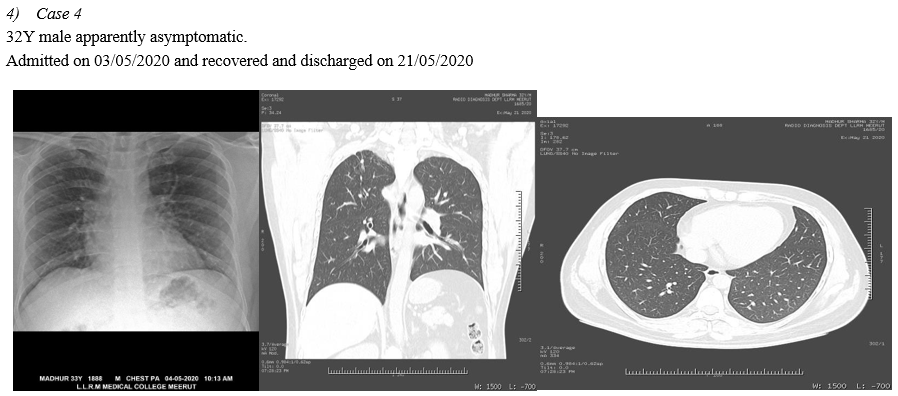
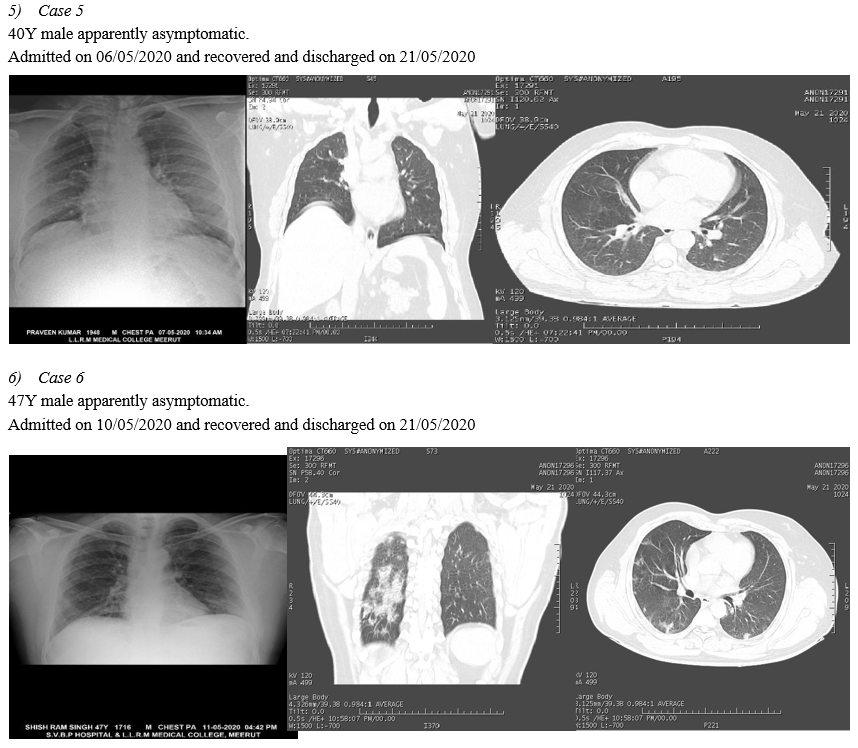
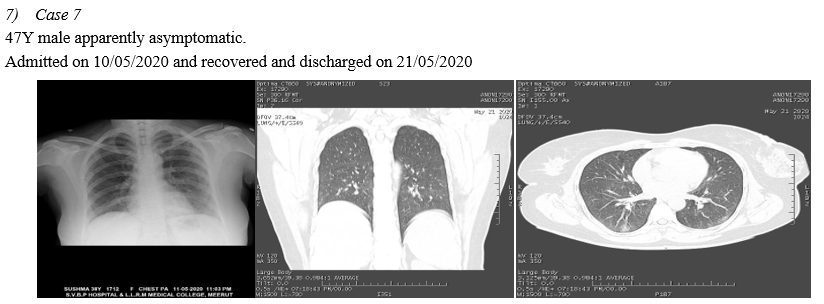
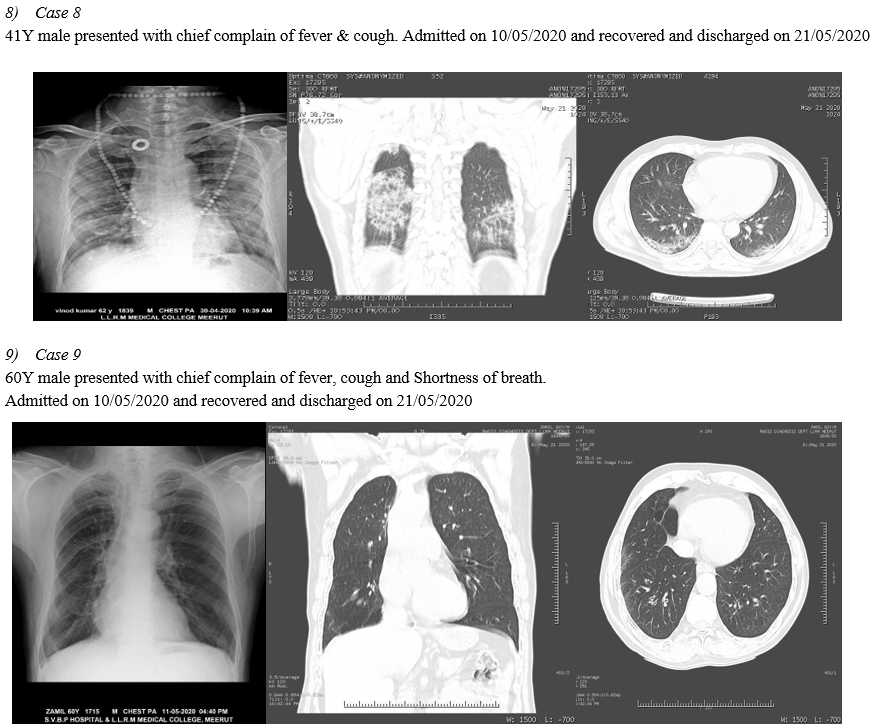
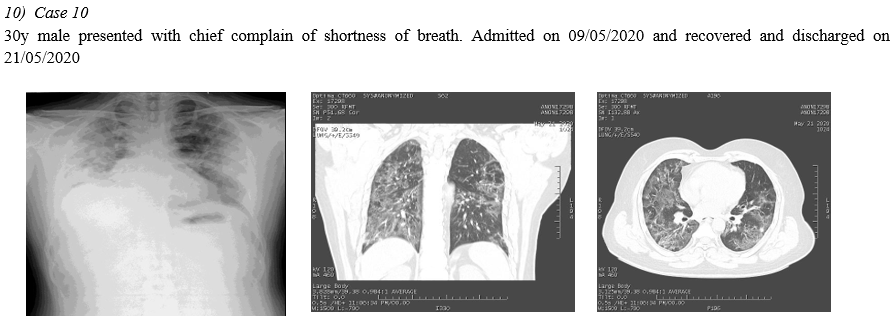
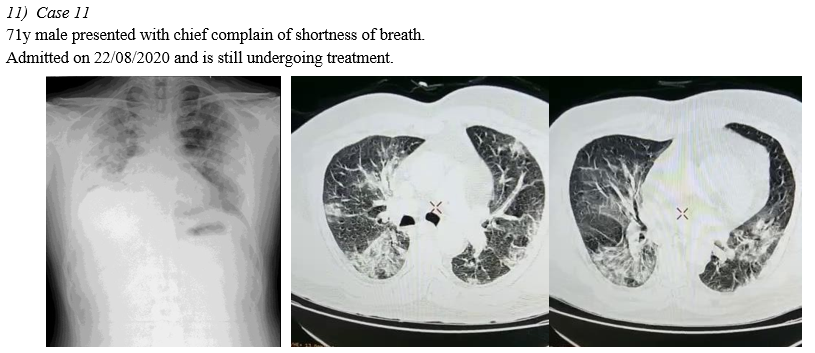
Conclusion
As the global pandemic of coronavirus disease-19 (COVID-19) progresses, many physicians in a wide variety of specialties continue to play pivotal roles in diagnosis and management. In radiology, much of the literature to date has focused on chest CT manifestations of COVID-19. However, due to infection control issues related to patient transport to CT suites, the inefficiencies introduced in CT room de- contamination, and lack of CT availability in parts of the world, portable chest radiography (CXR) will likely be the most commonly utilized modality for identification and follow up of lung abnormalities. CT decontamination required after scanning COVID-19 patients may disrupt radiological service availability and suggests that portable chest radiography may be considered to minimize the risk of cross-infection. Furthermore, in cases of high clinical suspicion for COVID-19, a positive CXR may obviate the need for CT. Additionally, CXR utilization for early disease detection may also play a vital role in areas around the world with limited access to reliable real-time reverse transcription polymerase chain reaction (RT-PCR) COVID testing. Patterns of COVID-19 lung disease can be identified on conventional chest radiography as well as chest CT. Typical verbiage when reporting patients with, or suspected COVID-19 on CXR include terms such as irregular, patchy, hazy, reticular, and widespread ground glass opacities. Grading disease severity based on total lung involvement is also important to relay to the clinicians. As the pandemic progresses, the medical community will frequently rely on portable CXR due to its widespread availability and reduced infection control issues that currently limit CT utilization. This is the third corona virus pandemic in recent years with tremendous impact on the global health and economy. CT is used only in specific clinical indications, and not for screening COVID-19 patients due to low specificity and problems with infection control 17 . Nevertheless, the global implications of the pandemic make it important for radiologists, trainees and clinicians to be familiar with the varying radiographic features of coronavirus lung disease to assist in difficult clinical decisions and manage the care of their patients.
References
[1] Zhou S., Wang Y., Zhu T., Xia L. CT features of coronavirus disease 2019 (COVID-19) pneumonia in 62 patients in Wuhan, China. Am J Roentgenol. 2020:1–8. March. [2] Chung M., Bernheim A., Mei X. CT imaging features of 2019 novel coronavirus (2019-nCoV) Radiology. February 2020;200230 [3] ACR recommendations for the use of chest radiography and computed tomography (CT) for suspected COVID-19 infection|American College of Radiology. [4] Wong H.Y.F., Lam H.Y.S., Fong A.H. Frequency and distribution of chest radiographic findings in COVID-19 positive patients. Radiology. 2019:201160. Mar 27 [5] Vilar J., Domingo M.L., Soto C. Radiology of bacterial pneumonia. J Eur J Radiol. 2004 Aug;51(2):102–113.
Copyright
Copyright © 2022 Dr. Yasmeen Usmani. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET39411
Publish Date : 2021-12-13
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

