Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- Conclusion
- References
- Copyright
HIV/AIDS Treatment & Prevention with Nano-Technology: A Review
Authors: Pallavi Singh, Dr. Sonia Duggal
DOI Link: https://doi.org/10.22214/ijraset.2023.52177
Certificate: View Certificate
Abstract
The HIV/AIDS epidemic remains unabated due to the lack of a cure or vaccine. Combination antiretroviral treatment has significantly improved patient outcomes, but it must be taken continuously, may have severe side effects, and is no longer effective for those whose viruses have developed resistance. Nanomedicine is a cutting-edge illustration of how nanotechnology, a multidisciplinary new science, is influencing healthcare in the twenty-first century. It might dramatically enhance HIV/AIDS treatment and prevention over time. In this paper, the challenges of the current HIV/AIDS treatment are examined, followed by a discussion of the amazing potential of nanotechnology to increase the effectiveness of antiretroviral therapy, and gene therapy.
Introduction
I. INTRODUCTION
Nanotechnology involves the development and manipulation of systems and materials with at least one feature measuring in the nanometre range, or on a scale of billionths of a metre. In terms of their physicochemical characteristics, particles in this size range differ from those of bulk materials (macroscopic or microscopic scale) or single atoms or molecules (the atomic scale). The interaction of nanoparticles with biological systems is significantly affected by their physicochemical properties. Other biological processes, such as immunological detection and the crossing of biological barriers, are also impacted by size concerns. Thus, medicines developed at the appropriate nanoscale dimensions may have distinct physicochemical and biological features that offer therapeutic benefits over traditional treatments. When problems with HIV and its treatment are resolved, nanotechnology research might help those who have the virus. More than 30 years have been spent attempting to develop a treatment for AIDS/HIV by scientists. Initially, antiretroviral medications were the focus of therapy, despite their inconsistent efficacy. The US Food and Drug Administration (FDA) has authorised 25 drugs since zidovudine in 1987; several of these drugs are available in fixed-dose combinations and generic formulations that are suitable for usage in low- resource areas (to date, only zidovudine and didanosine are available as true generics in the USA). However, HIV/AIDS treatment was completely transformed with the advent of protease inhibitors and triple-drug therapy in the middle of the 1990s. This marked the beginning of the era of highly active antiretroviral treatment (HAART), in which three or more different types of medication are administered at once to treat HIV. Patients' lifespans and overall quality of life have benefited greatly from the HAART treatment protocol, especially in developed countries. HAART, however, requires the permanent prescription of one or more drugs, and certain HAART regimens have substantial adverse effects. Individuals using many medications may acquire tolerance to their effects over time. The essential need for continued research into cutting-edge medicines for HIV/AIDS is highlighted by the fact that there is presently no comprehensive cure.
II. ABOUT NANO-TECHNOLOGY
Nanotechnology is a relatively young field of science and engineering that is already making important contributions to several aspects of healthcare. Knowledge of, skill in, and practise in working with atomic and molecular materials and structures are all part of this field. However, structures as big as several hundred nanometres can be used in nanotechnology. Nanomedicine, which is also called the medical use of nanotechnology, is the use of very small materials for prevention, treatment, and diagnosis. In the last few decades, nanomedicine has come a long way, especially when it comes to finding and treating cancer. In the past few years, nanotechnology has also been used to help prevent and treat HIV/AIDS, though at a lower level. Through new applications, nanotechnology may be able to improve current treatments and create new ones, like gene therapy and immunotherapy. Also, some nanomaterials can be used as medicines on their own. Nanotechnology could have a big impact on the way vaccines and microbicides are made. In this study, we look at how nanotechnology could be used to improve existing therapies, develop new therapies, and give options for making HIV/AIDS vaccines and microbicides.
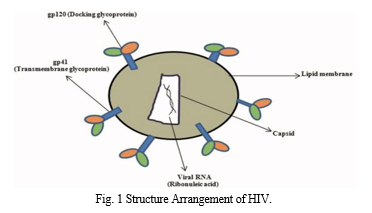
III. CURRENT HIV/AIDS TREATMENT
HAART is the most advanced treatment for HIV/AIDS right now. Patients take three or more antiretroviral drugs at the same time. Most of the time, medications that are used together are from different classes and work in different ways. Even though HAART therapy for HIV/AIDS has made a lot of progress, there are still some problems. The biggest problem has been that the therapy hasn't worked, which is often because patients didn't do what they were supposed to. Patients don't follow the treatment plan because they have to take the medicine every day for the rest of their lives. This means that the body doesn't get enough of the medicine and the virus starts to grow again.
Also, the virus becomes resistant to certain treatment combinations in some people who stick to their treatment plans well. HIV-1's huge genetic variety and constant change are two of the main reasons why it is so hard to treat. This problem is being fixed by giving each patient a personalised treatment plan. In this plan, resistance testing is used to choose the best combination of medicines that will work for each patient. Also, the harmful effects caused by the toxicity of the drugs are a worry. There have been claims that HAART makes patients more likely to get heart disease, diabetes, liver disease, cancer, and age faster. Most experts agree that these symptoms could be caused by HIV or co-infection with another virus, like hepatitis C virus co-infection that damages the liver. But it's possible that these side effects are caused by how toxic the HAART drugs are.
Our current methods of therapy have not allowed for a full elimination of the virus. "Latent reservoirs" of the virus are found in macrophage and monocyte progeny cells and memory CD4+ T cells. Macrophages have long been known to operate as latent repositories for viruses, but recent studies have shown that they also play a crucial role in the production of novel, difficult-to-detect mutant viral genotypes. Secondary lymphoid tissue, the testes, the liver, the kidney, the lungs, the gut, and the central nervous system are common locations for latent HIV-carrying cells to hide out. The virus must be eliminated from these sources for long-term therapy of HIV/AIDS patients to be successful. Thus, there is an urgent need to investigate innovative approaches to developing nontoxic, lower-dose therapy strategies that provide more continuous dosing coverage, efficiently eradicate viral reservoirs, and eliminate the need for treatment for life.
IV.HIV/AIDS TREATMENT WITH NANO- TECHNOLOGY
A. Nanotechnology for HIV Medication Distribution
Using nanotechnology platforms to get medicine to where it needs to go is changing many parts of how illness is treated. So far, cancer patients have gotten the most out of this revolution. There have been a lot of big steps forward in the past few decades. Several nanoscale cancer treatments have been approved by the FDA or are being tested in clinical trials. This huge achievement is made possible by the unique qualities that nanotechnology gives to drug delivery systems. With the help of nanotechnology, it is now possible to improve the distribution of medications that don't dissolve well in water, give drugs to specific cells or tissues, and get macromolecules into cells.
Nanotechnology-based drug delivery systems might provide a comparable advantage by distributing antiviral medications systemically. They may have prolonged half-lives in the blood at therapeutic concentrations if they are administered via controlled-release techniques. There may be far- reaching consequences for people's adherence to their medication regimens as a result of this. Nanoscale delivery devices improve and regulate the penetration and transport of both hydrophobic and hydrophilic drugs to their target regions.
This feature of nanoscale delivery devices seems to hold the greatest promise for combating HIV. It may be possible to ensure that antiretroviral medications reach the latent reservoirs by targeting CD4+ T cells and macrophages, as well as the brain and other organs. Drugs might be administered to particular targets over a longer time period and at larger dosages by adjusting the release characteristics of the delivery systems.
However, although the half-life of the free medication was just 38 hours, a single dosage of the treatment released slowly over three months in dogs and three weeks in mice. These findings highlight the potential of nanoscale medication delivery to decrease the frequency of dosing and boost patient adherence. Several experiments conducted by Dou et al. suggest that a surfactant system including Lipoid E80 may stabilise a nanosuspension of the medication indinavir, allowing for more uniform distribution to various tissues. Macrophages were injected with indinavir nanosuspensions, and their drug uptake was examined. Then, macrophage- loaded indinavir nanosuspensions were intravenously administered to the mice. As a result, the medication built up to dangerous levels in the body's organs such the lungs, liver, and spleen. Antiviral activity was high in the brain of a mouse model of HIV brain infection following a single intravenous dosage of the nanoparticle-loaded macrophages, and the medication was detectable in the blood for up to 14 days after treatment.
Based on the results of these investigations, we know that indinavir can cross the blood-brain barrier and remain there for as long as 14 days. The half-life of a standard dosage of indinavir is rather short, at around 2 hours. In the future, it may be simpler to transport more medications to the brain using nanoparticles if it is shown that macrophages can be utilised to target pharmaceuticals to the brain.
Antiretroviral medications have also been delivered with the use of active targeting. Most HIV is stored in macrophages. Receptors on their surface, including formyl peptide, mannose, galactose, and Fc receptors, might be employed for receptor- mediated internalisation. Stavudine was encased in mannose- and galactose-linked liposomes ranging in size from 120 to 200 nm. This resulted in increased drug concentrations in the liver, spleen, and lungs compared to those seen with free drug or simple liposomes. A medicine called stavudine, which has a short half-life in serum and dissolves in water (1 h).
Thus, tailored liposomes are far superior than free medicine due to their enhanced cellular uptake and prolonged tissue retention. Zidovudine, a medication with a short half-life and poor solubility, was encapsulated in a stearylamine-based mannose- targeted liposome to improve its delivery to the lymph nodes and spleen. Stavudine and zidovudine are two examples of nucleoside medicines with relatively short serum half-lives, but where they really shine as treatments is in their triphosphate intracellular form. Based on intracellular pharmacokinetics and clinical efficacy data, zidovudine is administered twice daily despite its short half-life in the blood. It will be necessary in the future for delivery methods based on nanotechnology to demonstrate significant increases in the half-lives of the drugs contained inside the capsules. This will make it possible to space out dosing intervals to once a week, once a month, or farther.
Separate studies used a mannose-targeted poly (propyleneimine) dendrimer nanocarrier to deliver efavirenz to human monocytes/macrophages in vitro. The targeted nanocarriers were 12 times more effective at getting into cells than the untargeted ones. Similarly, lamivudine was administered in vitro. Dendrimer systems, both targeted and non- targeted, demonstrated much higher anti-HIV efficacy compared to placebos. In a recent work, the medication efavirenz was targeted to in vitro macrophages by attaching the tetra-peptide tuftsin (Thr-Lys-Pro-Arg) to the same dendrimer. By using a customised dendrimer strategy, sustained release was boosted by a factor of six, cellular absorption by a factor of 34, and anti-HIV activity by a factor of seven compared to the free medicine. A peptide nanocarrier model was developed as a novel strategy for targeting HIV reservoirs in macrophages. A medication is linked to the PEG backbone in this scenario, and the PEG is then targeted by a bacterial peptide sequence for which macrophages produce a receptor. The study shown that macrophages in the liver, kidney, and spleen are more likely to take up peptide-PEG nanocarriers targeted to fMLF than nontargeted nanocarriers.
V.THE USE OF NANOTECHNOLOGY IN THE DELIVERY OF ANTIRETROVIRAL DRUGS FOR HIV/AIDS
Pharmaceutical medicine distribution has undergone a technical revolution thanks to nanotechnology. Nanotechnology's core concept is to modify a molecule's pharmacokinetics so that it may be used effectively in the eradication of HIV. When an anti- HIV drug is encapsulated in a nano-system, its pharmacokinetics (how quickly and how far the drug travels in the body), pharmacodynamics (how well it works in the body), and physicochemical properties (particularly the size and molecules that are exposed to the surface) are all regulated by the nano-system (Li and Huang 2008, LaVan et al. 2002). Potentially altering the distribution of medicines across tissues by targeting HIV reservoirs and extending their half-lives, nanotechnology's use to ARV drug delivery holds promise for the treatment of HIV (Amiji et al. 2006).
A. Liposomes
A liposome is a kind of microscopic vesicle that typically has an aqueous core that is surrounded by one or more phospholipid bilayers. The average size of a liposome is 25 nanometers, however some may be as large as several microns. Phospholipids, either natural or synthetic, as well as cholesterol, are employed in the manufacturing process of these substances. In addition to it, they could also include various other lipids or proteins. To improve the liposomes' ability to localise in the lymphatic system, especially in the lymph nodes and the spleen, the surface of the liposomes were modified by the integration of charges (either positive or negative) and a site-specific ligand (mannose). Using stearyl amine (SA) and diacetyl phosphate (DCP), respectively, positively and negatively charged nano-sized SE liposomes were synthesised. On the other hand, ligand-coated SE liposomes were created using mannose-terminated SA (mannose conjugate). Liposomes are recognised as foreign substances the moment they enter the human body, which prompts mononuclear phagocytic cells to pick them up as soon as possible and remove them. Liposomes are an efficient delivery mechanism for anti-HIV drugs due to the fact that HIV is located in the mononuclear phagocytic cells of individuals who are infected with HIV. Liposomes have the potential to improve the efficacy of anti-HIV drugs while also reducing the risk of their side effects.
B. Nanoparticles
Nanoparticles, or nanoparticles, are solid colloidal particles between 10 and 1 billionth of a metre in size. Their colloidal size and polymeric composition determines their ability to deliver medications precisely where they need to go and for how long. Polymeric nanoparticles, solid lipid nanoparticles and nanostructured lipid carriers, and inorganic nanoparticles are the most common types of nanoparticles used in HIV therapy. Nanoparticles are also being studied to overcome physical barriers in drug formulation, such as poor stability and poor solubility. Research on ARVs' delayed drug release kinetics and more precise targeted delivery to HIV-infected cells is ongoing. Increased efficacy, decreased resistance, decreased dosage, less systemic toxicity and side effects, and better patient compliance may all arise from drug encapsulation into such systems.
C. Niosomes
Niosomes are also known as vesicles of non-ionic surfactant. They are generated by the self-assembly of hydrated synthetic non-ionic surfactant monomers and may contain a range of drugs. Niosomes have been regarded a feasible alternative to liposomes. The water-soluble drug molecules are present in the aqueous compartments between the bilayers of niosomes, whereas the insoluble drug molecules are contained inside the bilayer matrix. Niosome-mediated drug delivery has the ability to alter biodistribution in a manner that enables more accurate targeting of the medication to certain tissues. After intravenous administration, the MPS recognises the size and shape of niosomes and absorbs more of them. These niosomes are subsequently deposited in organs with dense macrophage populations, such as the liver, spleen, and lungs.Since anti-HIV drugs have inherent elimination and metabolism issues, which are a crucial phenomenon for the delivery of anti-HIV drugs, the deficiencies of conventional dosage forms provide researchers with enormous opportunities to design and develop novel drug delivery systems to address these issues.
D. Polymeric Micelles
Polymeric micelles are nanostructures with a diameter of less than 100 nm. They have been used to improve the drug molecules' capacity to target specific disease sites, transit through the intestines, and dissolve in water. The core-shell structure of polymeric micelles, which are made up of block polymers, is similar to that of surfactant micelles. While shell bricks are hydrophilic, core blocks are hydrophobic. Thus, polymeric micelles provide a number of advantages, such as the solubilization of medications that are not easily soluble in water, resistance to chemical deterioration, and controlled
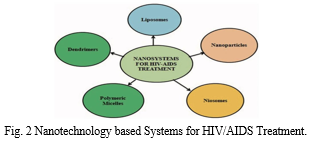
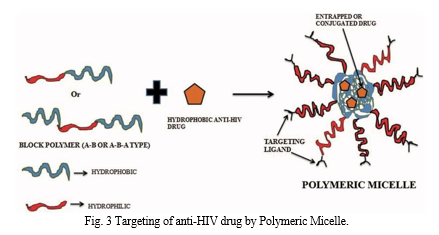
drug release. Micelle structure and its involvement in anti-HIV medication targeting. Additionally, the surface features of micelles may be changed by connecting hydrophilic blocks to antibodies or other ligands appropriate for the kind of receptors present at the location of the illness, such as in HIV/AIDS (Nagasaki et al . 2001).
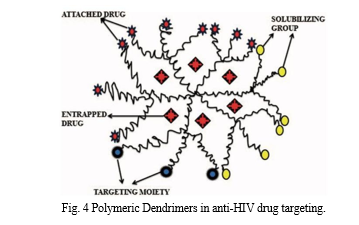
E. Dendrimers
Dendrimers are nanoscale (100 nm) polymeric structures that are organised around a central unit. The development, size, and microenvironment of the dendrimer are all determined by the layered arrangement of the branching units surrounding the core units.
Large numbers of tiny components called dendrons make up dendrimers. A dendron is formed when the central units are eliminated; it is then sectioned into a core (which does not exist), an interior (made up of branching units), and an exterior (end groups). Dendrons' internal voids provide a promising new venue for the entrapment of medicinal molecules for purposes like solubilization, controlled release, targeting, and defence against degradation.
F. Antiretroviral Therapy
Patients with HIV may choose from more than 25 anti-retroviral medications across at least six different molecular classes. Among them are inhibitors of reverse transcriptase, either nucleoside or non-nucleoside, as well as inhibitors of proteases, fusion proteins, CCR5 antagonists, and integrase strand transfer. However, none of these medications are curative since they cannot eliminate viral reservoirs, and the current objective of therapy is lifetime treatment with lasting viral suppression. Some of these problems may be alleviated by the development of, or access to, the following aspects made possible by the merging of pharmacology and nanotechnology:
- The use of antiretroviral drug delivery systems that regulate the tissue distribution and bioavailability of currently available antiretroviral medications, therefore reducing the potential for side effects.
- Extended half-life pharmaceuticals reduce dose frequency and pill load.
- Targeted medication delivery with an enhanced profile of adverse effects.
- Systems for decreasing drug-drug interactions.
- Methods for the administration of recognised antivirals through other pathways (e.g., transdermal delivery).
- Co-administration of antiretroviral drugs, hence enhancing adherence.
- New medications for the treatment of HIV infection: Using nanotechnology, antiretroviral compounds that would not otherwise be clinically useful due to solubility difficulties may be turned water-soluble.
- Protecting the nucleic acid from degradation and lowering its immunogenicity, the delivery vehicle facilitates the administration of otherwise difficult- to-administer anti-HIV medicines like siRNA and DNA therapies.
- Drugs with new ways of working that don't work against known agents.
- Drugs that go after viral reservoirs and kill them.
G. Gene Therapy
Therapeutic approaches based on RNA show great promise for treating HIV and many other illnesses, both infectious and otherwise. Some examples of such strategies include the use of ribozymes, antisense RNAs, RNA aptamers, RNA decoys, human ribonuclease P, modified small nuclear RNA, and small interfering RNAs.
Numerous non-viral methods of transporting therapeutic DNA and RNA to cells have been explored by scientists. Specifically, nanosized drug carrier systems have been developed that may be able to address a variety of issues associated with nucleic acid delivery, such as: increased safety (due to biocompatibility and renal clearance by the reticuloendothelial system), targeted delivery and controlled release, enhanced uptake by overcoming the electrostatic repulsion between negatively charged RNA or DNA and cell membranes, enhanced stability in physiological fluids, and pharming.
VI. THE CLINICAL PROMISE OF NANOTECHNOLOGY-BASED SOLUTIONS FOR HIV/AIDS THERAPY
The major factor that impacts the efficiency of antiretroviral treatment is the concentration of ARV medicine acquired at the targets, such as lymph node macrophages, spleen macrophages, lung pulmonary alveolar macrophages, and brain microglial cells, after delivery.
Clinical usefulness Frequent dosing increases the likelihood that the medication will accumulate to therapeutic levels in the intended tissue. The patient may have significant toxicity if an ARV drug is given to them often. Therefore, nanotechnology- based medicine delivery systems have opened up a new door for the efficient and precise elimination of HIV/AIDS. Nanotechnology-based methods provide more flexibility in repackaging and dosing these drugs to maximise bioavailability in the intended setting. Nanotechnology-based systems improve the capacity of antiretroviral drugs to pass through biological barriers (including the blood- brain barrier), reduce the number of times a patient must take a prescription, raise patient adherence, and lessen the risk of side effects. A liposomal version of AZT was studied by Deutsc et al. for its potential therapeutic utility (1993). Seven males who were HIV positive took part in the study. The mean age was 42,4 (range, 31–50). None of the patients could tolerate 500 milligrammes of AZT per day orally, despite receiving therapy for a mean of 17.4 months (range, 300–1200). Tolerance problems with oral medications stemmed from tummy troubles, low red blood cell counts, and muscle weakness. I.V. infusions of liposomal AZT ranging from 110 mg phospholipid/10 mg AZT to 660 mg phospholipid/60 mg AZT were given once weekly for up to six weeks. Before starting therapy with liposomal AZT, all patients had varying degrees of anaemia and leukopenia, ranging from moderate to severe. Platelet counts increased in this group (from a mean of 18510(9)/L at baseline to a mean of 21410(9)/L following treatment), which is consistent with the effects of oral AZT. The examination did not uncover any changes to the immune system. Two people had transient fever right after the injection, but no other negative effects were seen. Patients showed no signs of toxicity while on the liposomal treatment (Deutsc et al. 1993). This study demonstrated the efficacy of liposomal technology in clinical practise. Not a single report of a clinical study's results was added to the body of knowledge after that.
Conclusion
Potentially novel approaches to HIV/AIDS therapy and prevention might be influenced by nanotechnology. Delivery of antiviral drugs through nanotechnology platforms may improve current treatment options. It is possible that improved therapeutic effectiveness might result from increased patient adherence to prescribed medication schedules made possible by controlled and prolonged pharmaceutical release. Antiviral reservoirs may be treated more effectively in the future if many drugs are delivered simultaneously in a nanoparticle delivery system. Researchers in our group and another have developed nanoparticles that can co-deliver hydrophobic and hydrophilic medications or genes, which might provide delivery options for antiviral drugs. Nanomaterials have shown the capacity to inhibit viral replication, and this is in addition to their use in antiviral drugs. Gold nanoparticles, like silver nanoparticles and fullerenes and dendrimers, all have antiviral capabilities or may boost the antiviral activities of other compounds. Today\'s therapeutic strategies, such as gene therapy and immunotherapy, may be improved by the use of nanotechnology. One of the most active research areas in nanotechnology is the nonviral dissemination of siRNA. Research is still needed to develop a safe and effective nanotechnology for RNA interference (RNAi) that may be used to treat HIV/AIDS, however the delivery of siRNA to HIV- specific cells is now a reality. Nanotechnology has the potential to have a significant effect on immunotherapy, another vital area. Nano immunotherapy, which is now being tested with the DermaVir Patch in Phase II clinical trials, has the potential to be the first nanotechnology-based treatment for HIV/AIDS. Since the most seriously afflicted and sensitive individuals reside in underdeveloped and economically deprived countries, the economic component is another crucial consideration when pursuing nanotechnology-based remedies for HIV/AIDS. As a result of nanotechnology, the price of antiretroviral therapy may rise, reducing its overall value. Nano-therapeutics may be more expensive than conventional treatments, but their potential benefits may more than outweigh the costs if they improve patient adherence by reducing the number of times a treatment is administered and if they are successful in eliminating viral reservoirs, leading to sterile immunity. Nanomedicine has the potential to reduce the overall cost of developing and implementing novel treatment approaches like gene therapy and immunotherapy. Nano-therapeutics shouldn\'t be more costly than existing methods, though, especially in the context of preventive medicine. Developing nanotechnology-enhanced vaccines might be a cost-effective strategy for combating the worldwide HIV/AIDS epidemic, since massive quantities of immunisations are extensively distributed by government organisations. Nanotechnology-enabled microbicides may further need assistance from government or non-government entities for effective distribution in economically challenged regions. As a whole, the pace of scientific discovery has never been faster, and this is especially true in the realm of nanotechnology. There is widespread agreement that medicine and the HIV/AIDS field will reap long- term benefits from investments in nanotechnology.
References
[1] Kumar , L., Verma , S., Prasad , D. N., Bhardwaj , A., Vaidya , B., & Jain , A. K. (2014). Nanotechnology: A magic bullet for HIV AIDS treatment. 71-86 . [2] Mamo, T., E Ashley Moseman, Nagesh Kolishetti, Carolina Salvador- Morales, Jinjun Shi, Daniel R Kuritzkes, . . . Omid C Farokhzad. (2010 ). Emerging nanotechnology approaches for HIV/AIDS treatment and prevention.
Copyright
Copyright © 2023 Pallavi Singh, Dr. Sonia Duggal. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET52177
Publish Date : 2023-05-13
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

