Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- Conclusion
- References
- Copyright
Role of Medicinal Plants in Male Erectile Dysfunction
Authors: Ashish ., Dr. Gurdeep Singh
DOI Link: https://doi.org/10.22214/ijraset.2022.44012
Certificate: View Certificate
Abstract
“Erectile dysfunction (ED) or male impermanence” can be portrayed as a condition that causes sexual dysfunction and is characterized by the powerlessness to make and keep an erection in the penis. Globally, ED affects over 152 million men. By 2025, it is expected to reach 322 million. Insufficient physical activity, mental stress and other aetiological factors are all contributing to a decrease in the enjoyment of sexual pleasure. For the treatment and recovery of ED, there are many options, including nonpharmacological and pharmacological treatments such as alprostadil and penile prosthesis surgery and phosphodiesterase inhibitors. Allopathic prescriptions used to treat sexual dysfunction can cause secondary effects that influence other physiological cycles and eventually your overall wellbeing. Because of the availability and affordability of natural supplements from medicinal plants, there is a greater demand for them. Although there are many plants that have been used as aphrodisiacs, only a few of these plants have been scientifically proven to be effective in the controlling & curing of male erectile disorder. This detailed review directs on the aetiology and risk factors that lead to ED and the mechanisms that underlie it. Also, it includes the medicinal properties of plants which have been proved efficient to treat ED. This data could prove useful in the near future when it comes to research into developing more natural medicines that do not have negative side effects.
Introduction
ACKNOWLEDGEMENT
I have taken efforts in this project report. However, it would not have been possible without the kind support and help of many individuals either directly or indirectly. I would like to extend my sincere thanks to all of them.
I am highly indebted to Dr. Gurdeep Singh, Assistant Professor, Lovely Institute of Technology (Pharmacy) Lovely Professional University for his guidance and constant supervision as well as for providing necessary information regarding the project & also for his support in completing the project.
I would like to express my special gratitude and thanks to my teachers for giving me such attention, time, and necessary information for the completion of this project.
My thanks and appreciations also go to my parents and colleague in developing the project and people who have willingly helped me out with their abilities.
I dedicate this project to my parents and friends. It was their encouragement, constant inspiration, support, and blessings which helped me to take the audacious tasks as a challenge and finally to compete it.
Date: 21-05-2022
Place: Lovely Professional University, Phagwara (Punjab)
STATEMENT BY THE CANDIDATE
This is to submit that this written submission in my project report entitled “Role of Medicinal Plants in Male Erectile Dysfunction” represents original ideas in my own words and where others’ ideas or words have been included, I have adequately cited and referenced the original sources. I also declare that I have stuck to all principles of academic honesty and integrity and have not misrepresented or fabricated or falsified any idea/data/fact/source in my submission. I understand that any violation of the above will be cause for disciplinary action by the school and can also evoke penal action from the sources which have thus not been properly cited or from whom proper permission has not been taken when required.
I assure and hold full responsibility for its genuineness.
CERTIFICATE BY SUPERVISOR
The work described in this project report entitled “Role of Medicinal Plants in Male Erectile Dysfunction” has been carried out by Ashish under my supervision. I certify that this is his bonafide work. The work described is original and has not been submitted for any degree to this or any other university.
Date: 21-05-2022
Place: Lovely Professional University, Punjab (India) Dr. Gurdeep Singh
Assistant Professor,
Lovely Institute of Technology (Pharmacy)
Lovely Professional University,
Punjab, India.
CERTIFICATE BY SCHOOL
This is certified that the work described in this project report entitled “Role of Medicinal Plants in Male Erectile Dysfunction” submitted by Ashish under the guidance of Dr. Gurdeep Singh being duly certified and approved by the guide and accepted for submission to Lovely Professional University in partial fulfillment of the requirements for the award of the degree of bachelor’s in pharmacy in pharmaceutics.
Signature of HOD Signature of HOS
Dr. Sheetu Dr. Monika Gulati
Senior Dean
School of Pharmaceutical Sciences
I. INTRODUCTION
As per a study conducted by the “World Health Organization (WHO),” in 1987, nearly half of infertile couples had a deficient male reproductive capacity. Congenital, immunological, and iatrogenic reasons are the determining aspects that limit the likelihood of pregnancy in the female companion. In many situations, difficulty to conceive is due to oligozoospermia and sexual dysfunction (Chauhan et al., 2014). The lack of ability to achieve and sustain adequate penile tumescence to allow for erotic intercourse is known as male ED aka impotence (Masuku et al., 2020a). It is still a major health problem worldwide. This can be attributed to aging, diabetes mellitus and smoking, as well as previous operations, psychological factors, and drugs (Birowo et al., 2019; Mobley et al., 2017b). ED affects more than 152 million men worldwide (Eleazu et al., 2017a). Previously, 52% of ED among men occurred between the ages of 40 and 70 (Mobley et al., 2017b). Recent studies have shown that ED is increasing in prevalence even among those under 40 (Minh Tue Nguyen et al., 2017b). In Africa, nearly 71.45 percent people diagnosed with diabetes also confirmed to the development of ED (Shiferaw et al., 2020). Diagnosed with varying grades of ED, nearly 60 percent of diabetes patients in Ethiopia didn't get any medications (Hurisa & Negera, 2020). Even worse, if this continues, 322 million ED cases worldwide will be reported by 2025 (Aydin & Senel, 2020). Erectile dysfunction can have detrimental impacts on men's well-being; the majority of sufferers experience symptoms of anxiety and depression that are in relation to sexual activity (Shiferaw et al., 2020). Men diagnosed with ED were more likely to seek medical attention as ED led to conflict in relationships that destructively affected the couple’s well-being & physical health (Muneer, Kalsi, Nazareth, & Arya, 2014). Your social record should include your past history of smoking alcohol, drinking or alcohol, diet, exercise, as well as other factors (Patel et al., 2017). An extensive history of sexuality will be open-ended and need the patient's input regarding their sexuality, their past and present relationships, as in addition to their sexual health (Hatzimouratidis et al., 2010; Patel et al., 2017).
Erectile dysfunction can be treated non-pharmacologically by reducing stress, quitting smoking, limiting or eliminating alcohol consumption, increasing physical activity, and maintaining a healthy lifestyle (Diniz et al., 2020; Wassersug & Wibowo, 2017). Treatment can also be started with appropriate medical therapies, such as “phosphodiesterase type 5-Is (PDE5Is) like sildenafil, vardenafil, and tadalafil; anomorphine; synthetic prostaglandin E1 or alprostadil; phentol” (Diniz et al., 2020; S. Kim et al., 2021). PDE5-Is can cause headaches, myalgia, and facial flushing.
In addition, PDE5-Is have lost efficacy in cases of disease conditions that affect the upstream Nitric Oxide pathways (S. Kim et al., 2021). Thus, it is important to discover alternative agents that can unravel these constraints. It is practiced in many countries. Traditional medicine has been a part of Indian culture and religion for centuries (Malviya et al., 2016a). Traditional medicine refers to the practice and knowledge of holistic health care. In recent years, the medicinal plants have been subjective to extensive investigation in order to identify novel medications and determine whether their traditional usage can be aided by pharmacological evidence (Fabricant & Farnsworth, 2001). The pharmaceutical industry's R&D concentration is on developing new pharmaceuticals, remodelling regional procedures for existing drugs, and developing herbal drugs by pursuing leads from established medical procedures (Bhushan Patwardhan et al., 2004). Approximately 25 percent of all modern date medicine prescriptions are still constituted of extraordinary amount of active ingredients found in traditional herbs (Johari & Karki, 1999; Sharma et al., 2010a, 2010b). Moreover, thorough appraisals of scientific literature on the experimental proofs for therapeutic plants that help treat erectile dysfunction are inadequate. This is why a pharmacological assessment is so important.
As indicated by the ongoing concentrate on restorative plants for the regulation and management of male ED, an assortment of therapeutic plant species and bioactive mixtures were liked as treatment choices. They're all-regular, copious, effectively open, cheap, and have barely any, destructive aftereffects (Sin et al., 2021). PDE5 inhibitors can be found in many herbs that were used traditionally as aphrodisiacs (Anand Ganapathy et al., 2021). They have been shown to be effective in vivo as well as in vitro in the treatment and mitigation of ED. Potential healing properties are the reason for promising medicinal plants' activity in treating male ED. Traditional aphrodisiacs for ED include Panax ginseng and Myrica rubra (Masuku et al., 2021; Sin et al., 2021). Based on the “International Index of Erectile Function (IIEF),” a systematic examination of alternative medicine and herbal medicines for ED treatment indicated that there was encouraging evidence supporting the use of Panax ginseng and Tribulus terrestris, pycnogenol, and Prelox as ED therapies (Leisegang & Finelli, 2021). ED therapeutics, for example, nanoparticles laden with sialorphin, natural medicine, nitric oxide, or sonic hedgehog, as well as nanoparticle-related fat tissue-derived stem cells, have likewise been created utilizing nanotechnology (Masuku et al., 2020b). Despite the fact that herbal medicine and therapeutic plants have been revealed to be useful in the treatment of ED, additional clinical study is needed to validate their efficacy.
This article reviews the aetiology and risk factors for ED and the mechanisms that underlie it. It also discusses treatment options, including the use of medicinal plants that have been scientifically proven to be effective in reducing or treating ED in men. This study could provide information that can be used to develop more natural drugs without side effects in drug discovery.
II. MALE SEXUAL DYSFUNCTION
Male sexual dysfunction is the failure to get a typical sexual relationship over and again in an assortment of structures like untimely discharge slow, retrograde, or hindered discharge sexual brokenness, excitement issues (diminished sexual drive), impulsive sexual way of behaving orgasmic problem, and powerlessness to detumescence. Sexual dysfunction in men is expanding on the planet because of maturing populaces as well as other development factors (MT et al., 2007). ED or male impermanence can be portrayed as a condition that causes sexual dysfunction and is characterized by the powerlessness to make and keep an erection in the penis (Malviya et al., 2016b).
The purposes behind ED can be either physiological or mental (I-S Hwang et al., 1992). Penile erection is a muddled cycle including hormonal and psychogenic contributions along with a noncholinergic neurovascular system. The fundamental vasoactive, noncholinergic noradrenergic synapse and compound middle person for penile erection is nitric oxide (NO). The most widely recognized reason for ED is an absence of NO bioactivity (Burnett, 2006; Kaminetsky, 2008). To treat ED the use of folk remedies has been widely used and advertised extensively from the 1930s (Harnack et al., 2001). In the late 1990s, the first pharmacologically authorised therapy for impotence, sildenafil (brand name Viagra), received a lot of public attention, thanks to a lot of advertising (Drewes et al., 2003). There are a variety of herbal remedies that have been utilized by those suffering from ED with different levels of success (Adaikan et al., 2000; Kamatenesi-Mugisha & Oryem-Origa, 2005).
A. Male ED
- Penis Physiology
One of the most important parts of the male reproductive systems is the penis. It is made out of “three erectile tissues (huge), two corpora cavernosa, and a corpus spongiosum.” The penis was connected to the urinary tract by the urethra. Foreskin and prepuce are used to cover the glans, head of penis, or deep penile artery (Patton & Thibodeau, 2013; Rizzo, 2015; Sherwood, 2006; Widmaier et al., 2008).
2. Male ED Aetiology
a. ED Induced Endocrinopathies: Common endocrine diseases that are linked with ED include hypogonadism and diabetes, hypothyroidism, hypothyroidism, and hyperthyroidism (Papagiannopoulos et al., 2015). Hypogonadism in men is when the testes don't produce enough testosterone (Bayram et al., 2015). Primary hypogonadism is caused by gonadal abnormalities, while secondary hypogonadism is caused by hypothalamic-pituitary dysfunction (Bendre et al., 2025). Type 2 diabetes is also associated with low testosterone production (Defeudis et al., 2015). In the study by Haffner and colleagues (Haffner et al., 1996), blood insulin, sexhormone-bindingglobulin (SHBG), total testosterone, and free testosterone were all measured. Blood samples from 176 diabetic males were then compared to controls. Patient elements connected to the advancement of type II diabetes in men were studied and lower levels of complete testosterone, free testosterone, and SHBG, while higher insulin levels were found. These (Haffner et al., 1996). The study by Grossmann and Witter supported this finding (Grossmann & Wittert, 2012). They discovered a link between type-2 diabetes and significantly lower testosterone levels. Another study indicated that diabetic males became more resistant to insulin when administered with testosterone replacement therapy (Kapoor et al., 2006). In hyperthyroidism, the thyroid gland generates extreme levels of thyroid hormone in blood (Keller et al., 2012) and free thyroxine and thyroid-stimulating hormone blood tests are done regularly to confirm functioning of thyroid gland (Corona et al., 2012). To establish ED & thyroid disorder relationship, researchers employed the “European Male Aging Study,” which included 40 to 79 years aged 3369 men. The UNIFI trial included 3203 male patients aged 51.8+- 13.0 years who were treated at the “Andrology and Sexual Medicine Outpatient Clinic at the University of Florence.” In the EMAS study and UNIFI study, decreased TSH and higher FT4 were found, respectively, at 0.3 % & 0.2 %. The study also found a link between ED and TSH levels. Hyperthyroidism can also increase serum levels SHBG, which in turn reduces the free testosterone levels (Irwin, 2019). =In a study of 109 ED males, Chen and colleagues discovered that 66.06 percent had hypothyroidism. Another 29.36 percent had subclinical hypothyroidism. Thyroid-stimulating hormone, free thyroxine, and serum prolactin levels were higher in hypothyroid ED patients than in euthyroid individuals.
b. Neurogenic ED: Both the somatic as well as the autonomic nervous system regulate penile erection (Krassioukov & Elliott, 2017; Robert C. Dean & Tom F. Lue, 2005). Parasympathetic neurotransmitters include NO, acetylcholine, and prostaglandins (Krassioukov & Elliott, 2017). The cavernosal smooth muscles relax and the penile blood vessels dilate as a result of parasympathetic activity. Sympathetic stimulation triggers the smooth muscles and blood vessels of the penile to contract (Krassioukov & Elliott, 2017; Robert C. Dean & Tom F. Lue, 2005). This system releases neurotransmitters like vasopressin & angiotensin as well as norepinephrine & endothelin. The central nervous system (CNS) receives impulses from glans penis & transmits to the penis via somatic nervous system containing motor & sensory nerves. The penis' tactile stimulus triggers neuronal signals that are transmitted to the spinal cord's erection-generating center. This activates the autonomic nervous systems and then penile erection (Giuliano et al., 1997; Robert C. Dean & Tom F. Lue, 2005). The physiological response to sexual stimulation is impaired by neurological disorders. Patients with ED have been shown to be more likely to suffer from spinal cord injury, multiple sclerosis, and epilepsy. The erectile function can be interfered by these conditions (Avasthi et al., 2017; L. Chen, Shi, rui Huang, et al., 2019; Yafi et al., 2016).
c. Vasculogenic ED: Regular erection of penis depends on blood flow to the penis erectile tissues. Any impairment causes ED (E. D. Kim et al., 2015). Vasculogenic ED may be caused by atherosclerosis. This results in the occlusion or narrowing of blood vessels that supply the corpora cavernosa of penis. This causes perfusion of penis to be impaired and subsequently reduces penis erectile rigidity (Minh Tue Nguyen et al., 2017a; Robert C. Dean & Tom F. Lue, 2005). Atherosclerosis can be early in its development. Endothelial dysfunction is a critical factor. Hypertension and diabetes can cause impaired endothelial function (Yousef Kamel Qawqzeh et al., 2012).
3. Male ED Risk Factors
a. Diabetes Mellitus: Diabetes, a disorder caused by a shortage of insulin or tissue resistance to insulin & is defined by abnormal high blood glucose levels (O’Flaherty & Matsushita-Fournier, 2017; Ogurtsova et al., 2017). The most frequent kinds of diabetes are type 1 and type 2. Type 1 diabetes accounts for about ten to fifteen percent of all diabetes cases. Around 80% of people have type 2 diabetes (Boitard, 2012). Juvenile-onset diabetes or Type-1 Diabetes is triggered by damage to the pancreatic-islets β-cells that generate insulin (Pociot & Lernmark, 2016). It is more frequent in children, but it can affect people of all ages. T lymphocytes attack islet-b-cells in this autoimmune disease (Rewers & Ludvigsson, 2016; Zhou & Melton, 2018). Exposition to toxins, diet, or infections may trigger an autoimmune response (Rewers & Ludvigsson, 2016). Hyperglycemia can be caused by b-cell damage. Insufficient insulin levels are produced to slow down blood glucose levels. Type 1 diabetics must use exogenous insulin to compensate the insulin deficiency and maintain appropriate plasma glucose levels (J. Chen et al., 2018). An abnormal rise in blood glucose is observed as a result of insulin resistance in malfunctioning pancreatic cells & tissue (Zheng et al., 2017). Family history, age, and a poor diet are all factors in Type 2. It can also be caused by nutritional factors like high sugar intake, low fruit and vegetable consumption, and a higher intake of red meat and processed beef (Forouhi, 2010; Zheng et al., 2017). ED can be a complication or a symptom of diabetes. Seeing the current trends, frequency of ED is thrice in diabetic men when evaluated to non-diabetic individuals. ED is a common condition in between 35 and 90% of diabetic men(DeLay et al., 2016). ED can become more severe as we age and also depends on how long we have had diabetes (Kalter-Leibovici et al., 2005). Diabetic males who have ED respond less to medical treatment than non-diabetic men without ED (Binmoammar et al., 2016).
b. Hypertension: 1.39 billion persons suffer from hypertension, a significant medical disease. In the low and middle worlds, hypertension affects about 31.5 percent and 28.5 percent of people, respectively (Mills et al., 2016). Globally, CVDs are one of the leading causes for death. They account for 17.3 million deaths and by 2030s the prevalence of CVDs is projected to rise to 23.6 million. In both low- and high-income countries, CVDs mortality is about 8% (Ibrahim et al., 2018). The leading causes of death are heart attack, stroke, chest pain, heart failure, heart attack, heart attacks, heart failure, congenital heart disease, and heart attack (Williams et al., 2014). There is a substantial link between CVDs and ED, according to research. Because it raises the chance of developing cardiovascular diseases (CVDs), ED is regarded to be the earliest indication of them (Mobley et al., 2017a; Viigimaa et al., 2014). This link has been validated by Uddin and his colleagues (Uddin et al., 2018). Over the course of 45.6 months, 1757 individuals with ED and no CVDs participated in a multi-ethnic study on atherosclerosis. Strokes and fatalities from strokes were also included (Uddin et al., 2018). Obesity, diabetes, smoking, hyperlipidaemia, and high blood pressure have all been linked to the development of CVDs and ED (Mobley et al., 2017a; Viigimaa et al., 2014) Endothelial function is harmed, NO generation is reduced, and ED is caused by these risk factors. Managing these factors will thus aid in the prevention of ED and other consequences. An aid in decreasing BP and restoring sexual performance can be achieved by a nutritious diet and regular physical exercise (Mills et al., 2016).
c. Obesity: Obesity refers to a condition where the body's mass index is abnormally high, at least 30 kg/m2 (Karadag et al., 2014). There are 30 percent more chances of developing ED in a male with a BMI greater than 28.7 kg/m2, when compared to a normal BMI of <= 25kg/m2 (Esposito et al., 2008). A second study found that ED is more common in younger men who have a BMI greater than 30 kg/m2 (Andersen et al., 2008). Patients with a BMI of >= 21kg/m2 were found to be more likely to develop high BP, dyslipidemia, and diabetes (Esposito et al., 2008). There is a substantial link between diet, obesity, and the development of ED (Abdullah et al., 2018; Esposito et al., 2006; La et al., 2018). Men with a reduced intake of fruits, vegetables, and fish, as well as one with eating processed meats, red meat, sugary and salty foods, high-refine grains, & milk products, are at greater risk for developing ED (La et al., 2018). Males without ED have reported an increase in vegetable, fruit, nuts, whole grains, fish, and decreased intake in those with ED. Men with ED consume less processed and red meat, as well as refined cereals (Esposito et al., 2006). Ramirez & co. also found that males with ED had lower dietary intakes of vegetables and fruits, as well as other lifestyle factors like smoking, alcohol consumption, and inactivity (Ramírez et al., 2016). An individual eating regimen wealthy in whole grains, natural products, legumes, nuts, and fish has been connected to a lower occurrence of ED (La et al., 2018).
d. Lack of Physical Activity: It has been shown that ED is strongly linked to a sedentary lifestyle (Duca et al., 2019). Physically inactive males are more likely to get ED than physically active guys. In physically active guys, exercise can increase sexual function (Duca et al., 2019). It increases endothelial NO production and testosterone synthesis and insulin sensitivity. Cardiovascular diseases are closely linked to ED. High blood pressure, smoking, diabetes, and obesity are all factors that can be linked to the association (Dong et al., 2011). Patients with ED frequently have problems with their cardiovascular system. Regular exercise can help with both cardiovascular and erectile problems. Exercise and medicine can also be used to treat ED (MS Allen, 2019).
e. Alcoholism: It is believed that low levels of alcohol consumption can increase sexual desire and erection. This level of alcohol consumption is thought to reduce anxiety and relax the muscles. Drinking large amounts of alcohol can cause a reduction in sexual desire and ED (Eleazu et al., 2017a). In males, excessive alcohol use can lead to gonad atrophy and decreased sexual drive (Piché et al., 2018). Despite the notion that alcohol can impair the central nervous system, Furukawa's study revealed no link between alcohol consumption and sexual arousal (Furukawa et al., 2016). Connor and colleagues conducted a survey on men and women aged 38 about their sexual history due to alcohol consumption (Connor et al., 2015). The results showed that both 77.3 percent men & 79.9 percent women drank alcohol together before having sexual intercourse, whereas 82.1 percent women & 82.9 percent men did not drink alcohol to induce sexual activity. The same study also revealed that 8.3 percent (men) and 7.1 percent (women), used alcohol to enhance their sexual performance (Connor et al., 2015). It has been shown that extreme alcohol consumption and incessant abuse of alcohol can lead to liver cirrhosis in 30-40% of cases worldwide. This could even cause death (Osna et al., 2017). Hypogonadism, or a lack of testosterone, can result in liver cirrhosis in males. The conversion of blood testosterone to oestrogen causes this. It results in gonad atrophy and a decrease in sexual drive (Eshraghian et al., 2014).
f. Cigarette Smoking: It has been shown that ED conditions can be linked to smoking tobacco. It has been demonstrated that smoking for brief periods of time has no effect on testosterone levels or erection. If smokers smoke for prolonged periods of time, testosterone levels may decline (Ioakeimidis et al., 2017). 18,427 sexually active Australian men and women were studied by Wen and colleagues, aged 16 to 69, and discovered a greater incidence of ED with smoking more cigarettes. Individuals smoking more than 20 cigarettes per day have witnessed problems maintaining erections and lack sexual attraction as compared to non-smokers (Wen et al., 2017). Cigarette smoking can trigger a number of processes that lead to atherosclerosis, which is a result of ED (Muneer, Kalsi, Nazareth, Bmj, et al., 2014). High ROS levels leading to oxidative stress and ED are found to result from tobacco smoking (Wen et al., 2017). Enhanced endothelial function and a lower risk of CVD are some of the reversed results of stopping smoking (Muneer, Kalsi, Nazareth, Bmj, et al., 2014).
g. ED Induced via Drugs: ED can be caused by recreational drugs like opioids, cocaine, and methadone (L. Chen, Shi, Huang, et al., 2019; Hatzimouratidis et al., 2010). When cocaine activates endothelial cell cells, endothelin-1 is released. Endothelin-1, a potent vasoconstrictor produced by endothelial cells, reduces NO generation, which is a vasodilator (Schwartz et al., 2010). Opioid abuse can cause ED by decreasing GnRH levels or triggering excessive prolactin release in the brain. They also cause a negative feedback effect on the pituitary gland's release of luteinizing hormone, which in turn causes a decrease in testosterone levels (Quaglio et al., 2008; Venkatesh et al., 2014). Methadone increases brain prolactin release. Gonadotropin-releasing hormone release, the principal hormone that triggers testosterone manufacture, is inhibited by high prolactin levels. As a result, testosterone levels, which are critical for sexual function, drop dramatically (Yee et al., 2016). Moreover, ED can be caused by prescribed medications that are routinely used to treat other health problems like depression, mental illness, and cardiovascular diseases (CVDs) (L. Chen, Shi, Huang, et al., 2019; Muneer, Kalsi, Nazareth, & Arya, 2014). Patients who have taken antidepressants, antidepressants, and cardiac antipsychotics as well as diuretics, have experienced this condition. B blockers, methyldopa and verapamil are all antihypertensive drugs (L. Chen, Shi, Huang, et al., 2019; Muneer, Kalsi, Nazareth, & Arya, 2014). Tranylcypromine and other antidepressants include phenelzine (ortriptyline), sertraline (or imipramine), doxepin, paroxetine, and citalopram (L. Chen, Shi, Huang, et al., 2019). Cardiac drugs include digoxin and amiodarone (Muneer, Kalsi, Nazareth, & Arya, 2014) as well as beta-blockers such as clonidine, hydrochlorothiazide (methyldopa), methyldopa spironolactone and metronidazole (L. Chen, Shi, Huang, et al., 2019). Fluphenazine (L. Chen, Shi, Huang, et al., 2019), lithium, chlorpromazine and risperidone are all antipsychotic drugs. Diuretics include spironolactone, thiazide (Muneer, Kalsi, Nazareth, & Arya, 2014).
h. Psychological Factors: Men with ED are often afflicted by their symptoms and experience lower quality of life (Andersson et al., 2011). Anxiety and depression could cause ED. Rajkumar, and Kumaran conducted a study that found a link between anxiety and depression in 64 patients who had ED (Rajkumar et al., 2015). Out of 64 men who attended clinic, 15 (23.4%) had anxiety disorders and 8 (8.5%) suffered from comorbid depression disorder. ED may also cause anxiety and depression (Lockhat et al., 2013). Strong correlation exists between male ED and female sexual dysfunction (FSD). It has been demonstrated that ED in males has a major impact on the sexual well-being of women's relationships, and vice versa. Grewal and colleagues recruited 201 female subjects and 163 male partners in the study (Singh Grewal et al., 2014). The IIEF measured male partners and assessed female sexual function using the “Female Sexual Functioning Index (FSFI).” The study discovered that 106 males (or 65 percent) had ED. There were 50.9 percent with mild ED, 13.5 percent with mild-moderate ED, 0.6 percent with moderate ED, and none with severe ED. A favourable link was also discovered between IIEF & FSFI scores in the study (35.6 percent). When couples seek infertility therapy, Yeoh and his team discovered a link between male and female sexual functioning (Yeoh et al., 2014). There were 150 patients in all, 109 of them were men. According to the findings, 17 (11%) of female patients reported sexual dysfunction. The FSFI and IIEF total scores had a good connection (r= 0.57), according to the study. As a result, both wives and male companions must be included in the clinical assessment and therapy of ED (Singh Grewal et al., 2014; Yeoh et al., 2014).
B. ED Pathophysiology
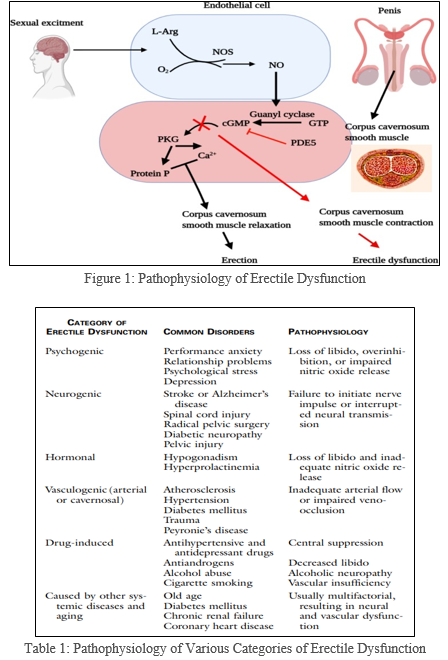
Detumescence and penile erection are both vital for erection. A few chemicals, synapses, and other courier particles communicate in an intricate manner to change the tone in the corpus cavernosum smooth muscle. Although the instrument basic these confounded natural cycles is yet obscure, it has been exhibited that the “nitric oxide/cyclic guanosine monophosphate” framework has a basic impact on interceding Erectile action. Erectile dysfunction is due to psychogenic or organic elements. Taub and his team discovered that the connection between contraction and relaxation in tissues from rabbits and humans was analysed by an equation of first-order linearity. The relationship is described as the inverted relation. Its slope is distinct from unity in tissues taken from two patients who have normal erectile functions. However, in tissues taken from 10 patients with organic erectile dysfunction, the slope was greater than unity. These preliminary findings have yet to be verified in larger groups of patients. They do suggest that patients suffering from erectile dysfunction might experience an overly negative relationship between muscular contracture and relax. Figure 1 illustrates the possible results of an imbalance of the relaxation of the smooth muscles in the body and contraction (Lerner et al., 1993).
The classification of ED as organic or psychogenic (neurogenic hormone, cavernosal arterial, or drug-induced) or mixed organic and psychogenic. The following table 1 outlines the causes (Lue, 2000).
III. MALE ERECTILE DYSFUNCTION TREATMENT WITH PROMISING MEDICINAL PLANTS
Modern medical treatment innovations have made it possible to find more medication that can reduce ED. Some men prefer herbal supplements over other options. Although many herbs have the potential to improve men's sexual function and there is little evidence to support their use in treating ED, it is possible to use herbal medications (Maggi et al., 2013a).
There are many phytochemicals found in plants, such as alkaloids and terpenoids, steroids, polyphenols, and steroidal compounds (Yadav & Agarwala, 2011). Because of their potential healing properties, polyphenols are gaining more attention. Polyphenols have anti-inflammatory, antioxidant, antiviral, and anticancer properties (L. Chen, Shi, Huang, et al., 2019; Curti et al., 2017). There are many polyphenols in vegetables, fruits, teas, and nuts as well as wine, seeds, coffee, and wines (L. Chen, Shi, Huang, et al., 2019; Eleazu et al., 2017b). These polyphenols include catechins and procyanidins as well as tannins, phenolic acid, stilbenoids, phenolic, phenolic, and catechins. However, very little research has been conducted on polyphenols to provide ED relief. Polyphenols could also provide protective actions on the vaso-corticovascular epithelium in the face of ROS-induced injury (Eleazu et al., 2017b). These are the few herbs that can be used to treat male erectile disorder and as an aphrodisiac (Maggi et al., 2013b).
A. Dehydroepiandrosterone (DHEA)
DHEA is a supplement that mimics the natural steroid hormone within the body, can be utilized for treating ED in males. DHEA supplements mimic the effects of natural steroids. DHEA dosages vary based on the person. Up to eight weeks, men might require between 20 and 75 mg (mg) of DHEA. Some may require between 100 to 400 mg.
As people age, natural DHEA levels decrease. The body is capable of producing hormones that improve sexual function and energy levels through increasing the amount of the adrenal hormone. DHEA treatment was proven to enhance the sexual experience in a study published in the journal of Urology. However, the study was tiny. Other studies have produced mixed results. A report from 2012 found that DHEA does not help with ED. DHEA is available in tiny doses and is generally considered safe. Acne may be an adverse consequence (West & Krychman, 2015).
B. Horny goat weed (Epimedium)
This Chinese herb is used to treat sexual dysfunction. It may also be used by women to decrease the likelihood of having painful intercourse or losing libido. Researchers are still not sure how the supplement works. Scientists believe that it may alter hormone levels, which could in turn increase sexual performance. People have not been tested on the effects of horny goat weed. A study, published in “The Journal of Sexual Medicine,” examined the effects of Epimedium purified extract on rats (Yakubu & Afolayan, 2010). The extract had a superior influence on blood flow in rats than the placebo. This herb can affect the heart function. It can cause irregular heartbeats and should be avoided by people with heart disease. Other drugs may interact with the medication.
C. Ginkgo
Ginkgo biloba, an herb used by doctors for centuries to treat various diseases is an herb. Anxiety, dementia, as well as inadequate blood flow for the brain is only some of the symptoms. Ginkgo has been utilized to treat various ailments. Ginkgo can boost blood flow to female sexual organs of the male, as per certain research. Ginkgo is believed to dilate blood vessels, promoting blood flow to the sexual organs (Yeh et al., 2008). Columbia University claims that ginkgo can be used to treat sexual dysfunction caused by selective serotonin reuptake inhibitions (SSRIs), medication prescribed for depression. People who are taking blood thinners should avoid ginkgo as it can increase bleeding risk. Side effects include stomach upset, nausea, mouth irritation, stomach upset, and stomach upset.
D. L-arginine
L-arginine, an amino acid, was first isolated from animal hair in 1800 by scientists. When L-arginine is converted in the body, nitric oxide is produced.
Blood arteries dilate as a result of nitric oxide, allowing more blood to flow through them. This helps men get an erection by increasing blood flow (West & Krychman, 2015).
To treat ED, L-arginine can be coupled with glutamate or yohimbine hydrochloride. In a research published in “The Journal of Sexual and Marital Therapy,” subjects were given a combination of Pycnogenol and L-arginine. The therapy lasted three months, and 92.5 percent of the 40 males with ED had normal erections. Side effects of L-arginine include diarrhoea and cramping, as well as stomach upset.
E. Red Ginseng
Ginseng is a plant that Korean herbalists suggest for its effectiveness in treating the erectile dysfunction. Panax Ginseng is another name for red ginger. Red ginseng may be able to treat erectile dysfunction according to several theories. These theories require more research.
Researchers aren't sure the ways that red ginseng may help alleviate symptoms of erectile dysfunction. One theory suggests that red ginseng may influence hormones that are responsible for erectile function. Another theory is that red ginseng promotes blood flow by increasing the level of nitric oxygen. Red ginseng is extra efficient than placebo in reducing ED symptoms, according to a 2008 British Journal of Clinical Pharmacology review (de Andrade et al., 2007).
Human studies are typically smaller in size, which is why it's hard for scientists to come up with definitive conclusions regarding the health advantages associated with red Ginseng. The red ginseng plant can cause insomnia. It is generally considered safe to use on an intermittent basis.
F. Yohimbine
Yohimbine is an African tree bark supplement. Doctors recommended yohimbine for ED treatment before the advent of medications like Viagra.
Yohimbine triggers receptors in the body to release the hormones norepinephrine (epinephrine) and yohimbine. They can also block other compounds' effects that could constrict blood vessels in the penis. Because of its side effects, the “American Urological Association” does not recommend yohimbine for ED treatment. In animal studies, however, it was shown to increase libido as well as sexual motivation. This supplement may have negative side effects. Anxiety, high blood sugar, fast pulse, high BP, and are among the negative effects (Guay et al., 2002). Yohimbe should never be taken by men without first consulting their doctor.
G. Asteracantha longifolia (L.) nees
In traditional medicine, “Asteracantha longifolia (L.) Nees” is used to treat jaundice, rheumatoid arthritis, gout, oedema, kidney infections, and as an aphrodisiac. “A. longifolia was used to isolate isoflavone glycoside, stigmasterol, lupeol, fatty acids, and alkaloids” (Paick et al., 2010).
Traditional medicine has also utilised A. longifolia as an aphrodisiac. The aphrodisiac efficacy of A. longifolia ethanolic seed extract in albino male rats was investigated by Buvat and colleagues (Buvat et al., 2011). Diminished mount latency (ML) & enhanced mount frequency (MF) in treated male rats compared to controls were evidenced by oral dosing for 28 days. The scientists stated that the findings appear to support the usage of the herb to increase sexual desire. However, no clinical examinations have been directed to decide the viability, safety, and resistance of A. longifolia in guys with ED.
H. Cynomorium Coccineum Linn.
“In Saudi Arabia, Cynomorium coccineum Linn. is known as Som-El-Ferakh,” a black leafless parasitic plant with no chlorophyll. Qataris use it as a tonic and aphrodisiac (usually in combination with honey). The watery concentrate of Cynomorium coccineum expanded sperm count essentially, upgraded the level of live sperm and motility, and diminished the amount of deficient sperm (El-Rahman et al., 1999).
In comparison to the untreated controls, testicular histology revealed enhanced “spermatogenesis and seminiferous tubules” full of sperm in the treated group. In young rats, aqueous extract of the plant caused significant spermatogenesis (Abdel-Magied et al., 2001). Extract-treated mice had lower serum testosterone and FSH levels than control mice, but higher levels of interstial cell stimulating hormone.
I. Camellia Sinensis
Camellia sinensis, sometimes known as tea plant, has proven to show antilisterial and aphrodisiac effects. “The aphrodisiac effect of C. sinensis (black tea brewed)” were first established by Ratnasooriya and colleagues. Aqueous tea isolates were given orally to male rats for around 3 hours.
The tea extract increased sexual arousal and copulation, as well as improving penile erection. Furthermore, in male rats, oral treatment of aqueous tea extract thrice a day for three days boosted blood testosterone levels (Akin-Olugbade et al., 2006). “C. sinensis (black tea brewed) is safe and effective for treating sexual dysfunction and as a sex stimulant, according to the research.” Despite this, no human clinical examinations evaluating the effectiveness & safety of C. sinensis have been done.
J. Curcuma Longa Linn
Curcuma longa Linn, often identified as turmeric, is a spice used to treat skin illnesses, diabetes, cancer, autoimmune diseases, stomach discomfort, blood purifiers, and hunger stimulants (Koon et al., 2017). Curcumin, aka diferuloylmethane, is an active component from Curcuma longa that affects the penile erectile response. When albino male rats were administered pure curcumin or water-soluble curcumin, the activity of “cavernous tissue cGMP and heme oxygenase enzyme-1 (HO1), both implicated in the penile erectile response mechanism,” was significantly increased, according to a research (Omisanjo et al., 2017). However, no clinical trials have been conducted to see if curcumin has the similar impact in humans or to assess its safety and efficacy.

Conclusion
Sexual activity can take on many structures. It is a complicated association between the endocrine & nervous frameworks, the cardiovascular framework as well as various designs which have an essential impact on sexual fulfillment and delight. The male sexual reaction cycle is isolated into five stages that are interrelated and happen in a specific request. Psychoactive drugs, as well as various illnesses and substances that may result in sexual dysfunction. Sexual dysfunction can influence your life quality along with self-esteem and interpersonal relationships. This could also be issues for healthcare professionals regarding monitoring and compliance. Alternative remedies may be sought by patients with sexual dysfunction as an alternative to traditional therapy. Due to this problem and the growing number of patients seeking treatments to treat MSD it is now evident that there is a growing demand for studies on pharmacology on alternative, less expensive treatment options. The “renin-angiotensin system, nitric oxide synthase, insulin resistance, glucose oxidation-induced superoxide production, and acetylcholinesterase” are all pathophysiologic processes implicated in ED. The penile prosthesis as well as Alprostadil is among the top two commonly reported negative effects of PDE inhibitors. Researchers have been encouraged to investigate different medicinal plants as well as natural active ingredients that assist with ED treatments and alleviation. Only a few clinical studies have looked at the usefulness and safety of medicinal plants in the treatment of ED. Medicinal herbs have been shown to be useful in the treatment of male ED in animal and in vitro studies. The plants are being utilised in clinical studies to help develop new medications to help with ED therapy.
References
[1] Abdel-Magied, E. M., Abdel-Rahman, H. A., & Harraz, F. M. (2001). The effect of aqueous extracts of Cynomorium coccineum and Withania somnifera on testicular development in immature Wistar rats. Journal of Ethnopharmacology, 75(1), 1–4. https://doi.org/10.1016/S0378-8741(00)00348-2 [2] Abdullah, A., Umar, A., Abdulkadir, A., Opara, J., & Ajibol, A. (2018). Role of exercise, fitness, and nutrition in the prevention of male sexual dysfunction. EUROPEAN JOURNAL OF SPORTS & EXERCISE SCIENCE, 6(3). [3] Adaikan, P. G., Gauthaman, K., Prasad, R. N. V., & Ng, S. C. (2000). Proerectile pharmacological effects of Tribulus terrestris extract on the rabbit corpus cavernosum. Annals of the Academy of Medicine, Singapore, 29(1), 22–26. https://europepmc.org/article/med/10748960 [4] Akin-Olugbade, O., Parker, M., Guhring, P., & Mulhall, J. (2006). Determinants of Patient Satisfaction Following Penile Prosthesis Surgery. The Journal of Sexual Medicine, 3(4), 743–748. https://doi.org/10.1111/J.1743-6109.2006.00278.X [5] Anand Ganapathy, A., Hari Priya, V. M., & Kumaran, A. (2021). Medicinal plants as a potential source of Phosphodiesterase-5 inhibitors: A review. Journal of Ethnopharmacology, 267, 113536. https://doi.org/10.1016/J.JEP.2020.113536 [6] Andersen, I., Heitman, B., & Medicine, G. W. (2008). Obesity and sexual dysfunction in younger Danish men. The Journal of Sexual Medicine, 5(9), 2053–2060. https://www.sciencedirect.com/science/article/pii/S1743609515321470 [7] Andersson, E., Walén, C., Hallberg, J., … B. P.-T. journal of sexual, & 2011, undefined. (2011). A randomized controlled trial of guided internet?delivered cognitive behavioral therapy for erectile dysfunction. Journal of Sexual Medicine. https://doi.org/10.1111/j.1743-6109.2011.02391.x [8] Avasthi, A., Grover, S., & Sathyanarayana Rao, T. (2017). Clinical practice guidelines for management of sexual dysfunction. Indian Journal of Psychiatry, 59(1), 91–115. https://www.ncbi.nlm.nih.gov/pmc/articles/pmc5310110/ [9] Aydin, C., & Senel, E. (2020). Impotence literature: Scientometric analysis of erectile dysfunction articles between 1975 and 2018. Andrologia, 52(3). https://doi.org/10.1111/AND.13520 [10] Bayram, F., Elbuken, G., Korkmaz, C., Aydogdu, A., Karaca, Z., & Caklr, I. (2015). The Effects of Gonadotropin Replacement Therapy on Metabolic Parameters and Body Composition in Men with Idiopathic Hypogonadotropic Hypogonadism. Hormone and Metabolic Research, 48(2), 112–117. https://doi.org/10.1055/S-0035-1564252 [11] Bendre, S. v., Murray, P. J., & Basaria, S. (2025). Clomiphene citrate effectively increases testosterone in obese, young, hypogonadal men. Reproductive System & Sexual Disorders?: Current Research, 4(4). https://www.ncbi.nlm.nih.gov/pmc/articles/pmc4734653/ [12] Bhushan Patwardhan, Ashok D. B. Vaidya, & Mukund Chorghade. (2004). Ayurveda and natural products drug discovery on JSTOR. Current Science Association. https://www.jstor.org/stable/24109136 [13] Binmoammar, T. A., Hassounah, S., Alsaad, S., Rawaf, S., & Majeed, A. (2016). The impact of poor glycaemic control on the prevalence of erectile dysfunction in men with type 2 diabetes mellitus: a systematic review. JRSM Open, 7(3). https://doi.org/10.1177/2054270415622602 [14] Birowo, P., Deswanto, I. A., & Rasyid, N. (2019). Epidemiology of erectile dysfunction: A cross-sectional web-based survey conducted in an Indonesian national referral hospital. F1000Research 2019 8:817, 8, 817. https://doi.org/10.12688/f1000research.18930.1 [15] Boitard, C. (2012). Pancreatic islet autoimmunity. La Presse Médicale, 41(12), 636–650. https://www.sciencedirect.com/science/article/pii/S0755498212005568 [16] Burnett, A. L. (2006). The role of nitric oxide in erectile dysfunction: implications for medical therapy. Journal of Clinical Hypertension (Greenwich, Conn.), 8(12 Suppl 4), 53–62. https://doi.org/10.1111/J.1524-6175.2006.06026.X [17] Buvat, J., Montorsi, F., Maggi, M., Porst, H., Kaipia, A., Colson, M. H., Cuzin, B., Moncada, I., Martin-Morales, A., Yassin, A., Meuleman, E., Eardley, I., Dean, J. D., & Shabsigh, R. (2011). Hypogonadal Men Nonresponders to the PDE5 Inhibitor Tadalafil Benefit from Normalization of Testosterone Levels with a 1% Hydroalcoholic Testosterone Gel in the Treatment of Erectile Dysfunction (TADTEST Study). The Journal of Sexual Medicine, 8(1), 284–293. https://doi.org/10.1111/J.1743-6109.2010.01956.X [18] Chauhan, N. S., Sharma, V., Dixit, V. K., & Thakur, M. (2014). A review on plants used for improvement of sexual performance and virility. BioMed Research International, 2014. https://doi.org/10.1155/2014/868062 [19] Chen, J., Stimpson, S. E., Fernandez-Bueno, G. A., & Mathews, C. E. (2018). Mitochondrial reactive oxygen species and type 1 diabetes. Antioxidants and Redox Signaling, 29(14), 1361–1372. https://doi.org/10.1089/ars.2017.7346 [20] Chen, L., Shi, G., rui Huang, D., dan Li, Y. M., Chen chao Shi, M., Su, B. xiao, & Shi, G. jiang. (2019). Male sexual dysfunction: a review of literature on its pathological mechanisms, potential risk factors, and herbal drug intervention. Biomedicine & Pharmacotherapy, 112, 108585. https://www.sciencedirect.com/science/article/pii/S0753332218353289 [21] Chen, L., Shi, G. rui, Huang, D. dan, Li, Y., Ma, C. chao, Shi, M., Su, B. xiao, & Shi, G. jiang. (2019). Male sexual dysfunction: A review of literature on its pathological mechanisms, potential risk factors, and herbal drug intervention. Biomedicine & Pharmacotherapy, 112, 108585. https://doi.org/10.1016/J.BIOPHA.2019.01.046 [22] Connor, J. L., Kydd, R. M., & Dickson, N. P. (2015). Alcohol involvement in sexual behaviour and adverse sexual health outcomes from 26 to 38 years of age. PLoS ONE, 10(8). https://doi.org/10.1371/JOURNAL.PONE.0135660 [23] Corona, G., Wu, F. C. W., Forti, G., Lee, D. M., O’Connor, D. B., O’Neill, T. W., Pendleton, N., Bartfai, G., Boonen, S., Casanueva, F. F., Finn, J. D., Giwercman, A., Han, T. S., Huhtaniemi, I. T., Kula, K., Lean, M. E. J., Punab, M., Vanderschueren, D., Jannini, E. A., … Jiang, M. (2012). Thyroid hormones and male sexual function. International Journal of Andrology, 35(5), 668–679. https://doi.org/10.1111/J.1365-2605.2012.01266.X [24] Curti, V., di Lorenzo, A., Dacrema, M., Xiao, J., Nabavi, S. M., & Daglia, M. (2017). In vitro polyphenol effects on apoptosis: An update of literature data. Seminars in Cancer Biology, 46, 119–131. https://doi.org/10.1016/J.SEMCANCER.2017.08.005 [25] de Andrade, E., de Mesquita, A. A., de Almeida, C. J., de Andrade, P. M., Ortiz, V., Paranhos, M., Srougi, M., & Erdogrun, T. (2007). Study of the efficacy of Korean Red Ginseng in the treatment of erectile dysfunction. Asian Journal of Andrology, 9(2), 241–244. https://doi.org/10.1111/J.1745-7262.2007.00210.X [26] Defeudis, G., Gianfrilli, D., di Emidio, C., Pofi, R., Tuccinardi, D., Palermo, A., Lenzi, A., & Pozzilli, P. (2015). Erectile dysfunction and its management in patients with diabetes mellitus. Reviews in Endocrine and Metabolic Disorders, 16(3), 213–231. https://doi.org/10.1007/S11154-015-9321-4 [27] DeLay, K., J Haney, N., & Hellstrom, W. J. (2016). Modifying risk factors in the management of erectile dysfunction: a review. The World Journal of Men’s Health, 34(2), 89–100. https://synapse.koreamed.org/articles/1088815 [28] Diniz, A. F. A., Ferreira, R. C., de Souza, I. L. L., & da Silva, B. A. (2020). Ionic Channels as Potential Therapeutic Targets for Erectile Dysfunction: A Review. Frontiers in Pharmacology, 11. https://doi.org/10.3389/FPHAR.2020.01120 [29] Dong, J. Y., Zhang, Y. H., & Qin, L. Q. (2011). Erectile dysfunction and risk of cardiovascular disease: Meta-analysis of prospective cohort studies. Journal of the American College of Cardiology, 58(13), 1378–1385. https://doi.org/10.1016/J.JACC.2011.06.024 [30] Drewes, S. E., George, J., & Khan, F. (2003). Recent findings on natural products with erectile-dysfunction activity. Phytochemistry, 62(7), 1019–1025. https://www.sciencedirect.com/science/article/pii/S0031942202006210 [31] Duca, Y., Calogero, A. E., Cannarella, R., Giacone, F., Mongioi, L. M., Condorelli, R. A., & la Vignera, S. (2019). Erectile dysfunction, physical activity and physical exercise: Recommendations for clinical practice. Andrologia, 51(5). https://doi.org/10.1111/AND.13264 [32] Eleazu, C., Obianuju, N., Eleazu, K., & Kalu, W. (2017a). The role of dietary polyphenols in the management of erectile dysfunction–Mechanisms of action. Biomedicine & Pharmacotherapy, 88, 644–652. https://doi.org/10.1016/J.BIOPHA.2017.01.125 [33] Eleazu, C., Obianuju, N., Eleazu, K., & Kalu, W. (2017b). The role of dietary polyphenols in the management of erectile dysfunction–Mechanisms of action. Biomedicine & Pharmacotherapy, 88, 644–652. https://doi.org/10.1016/J.BIOPHA.2017.01.125 [34] El-Rahman, El-Badry, Mahmoud, O. M., & Harraz, F. A. (1999). The effect of the aqueous extract of Cynomorium coccineum on the epididymal sperm pattern of the rat. Phytotherapy Research, 13(3), 248–250. [35] Eshraghian, A., Medicine, S. T.-A. of I., & 2014, undefined. (2014). Systematic review: endocrine abnormalities in patients with liver cirrhosis. Archives of Iranian Medicine, 17(10). http://aimjournal.ir/Abstract/725 [36] Esposito, K., Giugliano, F., Ciotola, M., de Sio, M., D’Armiento, M., & Giugliano, D. (2008). Obesity and sexual dysfunction, male and female. International Journal of Impotence Research , 20(4), 358–365. https://www.nature.com/articles/ijir20089 [37] Esposito, K., Giugliano, F., de Sio, M., Carleo, D., di Palo, C., D’Armiento, M., & Giugliano, D. (2006). Dietary factors in erectile dysfunction. International Journal of Impotence Resaearch 2006 18:4, 18(4), 374. https://www.nature.com/articles/3901438 [38] Fabricant, D. S., & Farnsworth, N. R. (2001). The value of plants used in traditional medicine for drug discovery. Environmental Health Perspectives, 109(Suppl 1), 69. https://doi.org/10.1289/EHP.01109S169 [39] Forouhi, N. G. W. N. J. (2010). Epidemiology of diabetes. Medicine, 38(11), 602–606. https://www.sciencedirect.com/science/article/pii/S1357303910002082 [40] Furukawa, S., Sakai, T., Niiya, T., Miyaoka, H., Alcohol, T. M.-, & 2016, undefined. (2016). Alcohol consumption and prevalence of erectile dysfunction in Japanese patients with type 2 diabetes mellitus: Baseline data from the Dogo Study. Alcohol, 55, 17–22. https://www.sciencedirect.com/science/article/pii/S0741832915300203 [41] Giuliano, F., Rampin, O., Benoit, G., & North, A. J. (1997). Neural control of penile erection. Urologic Clinics of North America, 22(4), 746–766. https://www.sciencedirect.com/science/article/pii/S0094014321006935 [42] Grossmann, M., & Wittert, G. (2012). Androgens, diabetes and prostate cancer. Endocrine-Related Cancer, 10(5), 47–62. https://erc.bioscientifica.com/view/journals/erc/19/5/F47.xml [43] Guay, A. T., Spark, R. F., Jacobson, J., Murray, F. T., & Geisser, M. E. (2002). Yohimbine treatment of organic erectile dysfunction in a dose-escalation trial. International Journal of Impotence Research, 14(1), 25–31. https://doi.org/10.1038/SJ.IJIR.3900803 [44] Haffner, S. M., Shaten, J., Stem, M. P., Smith, G. D., & Kuller, L. (1996). Low levels of sex hormone-binding globulin and testosterone predict the development of non-insulin-dependent diabetes mellitus in men. Academic.Oup.Com, 143(9). https://academic.oup.com/aje/article-abstract/143/9/889/105092 [45] Harnack, L. J., Rydell, S. A., & Sharma, M. (2001). Prevalence of Use of Herbal Products by Adults in the Minneapolis/ St. Paul Metropolitan Area. Complementary Health Practice Review, 7(1), 66–67. https://doi.org/10.1177/153321010100700130 [46] Hatzimouratidis, K., Amar, E., Eardley, I., Giuliano, F., Hatzichristou, D., Montorsi, F., Vardi, Y., Wespes, E., & European Association of Urology. (2010). Guidelines on male sexual dysfunction: erectile dysfunction and premature ejaculation. European Urology, 57(5), 804–814. https://doi.org/10.1016/J.EURURO.2010.02.020 [47] Ho, C. C. K., & Tan, H. M. (2011). Rise of herbal and traditional medicine in erectile dysfunction management. Current Urology Reports, 12(6), 470–478. https://doi.org/10.1007/S11934-011-0217-X [48] Hurisa, A. D., & Negera, G. Z. (2020). Erectile Dysfunction among Diabetic Patients in a Tertiary Hospital of Southwest Ethiopia. The Open Public Health Journal, 13(1), 240–245. https://doi.org/10.2174/1874944502013010240 [49] Ibrahim, A., Ali, M., Kiernan, T. J., & Stack, A. G. (2018). Erectile dysfunction and ischaemic heart disease. European Cardiology Review, 13(2), 98–103. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6331774/ [50] Ioakeimidis, N., Vlachopoulos, C., Angelis, A., Terentes-Printzios, D., Geor-Gakopoulos, C., Skliros, N., Pollalis, D., Rokkas, K., Tousoulis, D., Tsioufis, C., Dimitriadis, K., Kasiakogias, A., Konstantinidis, D., Kalos, T., Mant-Zouranis, M., Aragiannis, D., Anoussis, G., Fragoulis, C., & Kontantinou, K. (2017). P4428Association between cigarette smoking and testosterone levels in men with erectile dysfunction. European Heart Journal. https://academic.oup.com/eurheartj/article-abstract/38/suppl_1/ehx504.P4428/4090471 [51] Irwin, G. M. (2019). Erectile dysfunction. Primarycare.Theclinics.Com, 46(1), 249–255. https://www.primarycare.theclinics.com/article/S0095-4543(19)30009-0/abstract [52] I-S Hwang, T., Liu, P., Yang, C., H J Erpenbach, O. K., Koshida, K., Nishino, A., Yamamoto, H., Uchibayashi, T., Naito, K., Hisazumi, H., Hirano, K., Hayashi, Y., Wahren, B., Andersson, L., Adenomatoid Tumors L J Tammela, I. T., Karttunen, T. J., Mäkäräinen, H. P., Hellström, P. A., Mattila, S. I., … Kurita, T. (1992). Penile detumescence: characterization of three phases. Elsevier, 146, 10–14. https://www.sciencedirect.com/science/article/pii/S0022534717379508 [53] Johari, R., & Karki, M. (1999). Tribal folk medicinal plant resources of south Asia. Reports of the South Asia Conference. https://lib.icimod.org/record/6267 [54] Kalter-Leibovici, O., Wainstein, J., Ziv, A., Harman-Bohem, I., Murad, H., & Raz, I. (2005). Clinical, socioeconomic, and lifestyle parameters associated with erectile dysfunction among diabetic men. Diabetes Care, 28(7), 1739–1744. https://diabetesjournals.org/care/article-abstract/28/7/1739/27912 [55] Kamatenesi-Mugisha, M., & Oryem-Origa, H. (2005). Traditional herbal remedies used in the management of sexual impotence and erectile dysfunction in western Uganda. African Health Sciences, 5(1), 40–49. https://www.ajol.info/index.php/ahs/article/view/6896 [56] Kaminetsky, J. (2008). Epidemiology and pathophysiology of male sexual dysfunction. International Journal of Impotence Research , 20(1), 3–10. https://www.nature.com/articles/ijir200816 [57] Kapoor, D., Goodwin, E., Channer, K. S., & Jones, T. H. (2006). Testosterone replacement therapy improves insulin resistance, glycaemic control, visceral adiposity and hypercholesterolaemia in hypogonadal men with. European Journal of Endocrinology, 154(6), 899–906. https://eje.bioscientifica.com/view/journals/eje/154/6/1540899.xml [58] Karadag, H., Oner, O., Karaoglan, A., Orsel, S., Demir, A. U., Firat, H., Karadeniz, D., Aksu, M., Ardic, S., Zeren Ucar, Z., Sevim, S., Yilmaz, H., Itil, O., & Oya, &. (2014). Body mass index and sexual dysfunction in males and females in a population study. Psychiatry and Clinical Psychopharmacology , 24(1), 76–83. https://doi.org/10.5455/bcp.20130925023705 [59] Keller, J., Chen, Y. K., & Lin, H. C. (2012). Hyperthyroidism and erectile dysfunction: a population-based case—control study. International Journal of Impotence Research , 24(6), 242–246. https://www.nature.com/articles/ijir201224 [60] Kim, E. D., Owen, R. C., White, G. S., Elkelany, O., & O. Rahnema, C. D. (2015). Endovascular treatment of vasculogenic erectile dysfunction. Asian Journal of Andrology, 17(1), 40–43. https://www.ncbi.nlm.nih.gov/pmc/articles/pmc4291874/ [61] Kim, S., Cho, M. C., Cho, S. Y., Chung, H., & Rajasekaran, M. R. (2021). Novel Emerging Therapies for Erectile Dysfunction. The World Journal of Men’s Health, 39(1), 1–17. https://doi.org/10.5534/WJMH.200007 [62] Koon, C. S., Sidi, H., Kumar, J., Xi, O. W., Das, S., Hatta, M. H., & Alfonso, C. (2017). The Phosphodiasterase 5-Inhibitors (PDE-5i) for Erectile Dysfunction (ED): A Therapeutic Challenge For Psychiatrists. Current Drug Targets, 19(12), 1366–1377. https://doi.org/10.2174/1389450118666170215164747 [63] Krassioukov, A., & Elliott, S. (2017). Neural control and physiology of sexual function: effect of spinal cord injury. Topics in Spinal Cord Injury Rehabilitation, 23(1), 1–10. https://meridian.allenpress.com/tscir/article-abstract/23/1/1/85588 [64] La, J. R., Natalie H. Yafi, & Faysal A. (2018). Diet and men’s sexual health. Sexual Medicine Reviews, 6(1), 54–68. https://www.sciencedirect.com/science/article/pii/S2050052117300744 [65] Leisegang, K., & Finelli, R. (2021). Alternative medicine and herbal remedies in the treatment of erectile dysfunction: A systematic review. Arab Journal of Urology , 19(3), 323–339. https://doi.org/10.1080/2090598X.2021.1926753 [66] Lerner, S. E., Melman, A., & Christ, G. J. (1993). A Review of Erectile Dysfunction: New Insights and More Questions. The Journal of Urology, 149(5), 1246–1255. https://doi.org/10.1016/S0022-5347(17)36359-0 [67] Lockhat, Y., Ross, A., Ramlachan, P., Family, C. R.-S. A., & 2013, undefined. (2013). The prevalence of erectile dysfunction at a primary healthcare clinic in Durban, KwaZulu-Natal. South African Family Practice. https://www.ajol.info/index.php/safp/article/view/90398 [68] Lue, T. F. (2000). Erectile Dysfunction. New England Journal of Medicine, 342(24), 1802–1813. https://doi.org/10.1056/NEJM200006153422407 [69] Maggi, M., Buvat, J., Corona, G., Guay, A., & Torres, L. O. (2013a). Hormonal Causes of Male Sexual Dysfunctions and Their Management (Hyperprolactinemia, Thyroid Disorders, GH Disorders, and DHEA). Journal of Sexual Medicine, 10(3), 661–677. https://doi.org/10.1111/J.1743-6109.2012.02735.X/FULL [70] Maggi, M., Buvat, J., Corona, G., Guay, A., & Torres, L. O. (2013b). Hormonal Causes of Male Sexual Dysfunctions and Their Management (Hyperprolactinemia, Thyroid Disorders, GH Disorders, and DHEA). Journal of Sexual Medicine, 10(3), 661–677. https://doi.org/10.1111/J.1743-6109.2012.02735.X/FULL [71] Malviya, N., Malviya, S., Jain, S., & Vyas, S. (2016a). A review of the potential of medicinal plants in the management and treatment of male sexual dysfunction. Andrologia, 48(8), 880–893. https://doi.org/10.1111/AND.12677 [72] Malviya, N., Malviya, S., Jain, S., & Vyas, S. (2016b). A review of the potential of medicinal plants in the management and treatment of male sexual dysfunction. Andrologia, 48(8), 880–893. https://doi.org/10.1111/AND.12677 [73] Masuku, N. P., Unuofin, J. O., & Lebelo, S. L. (2020a). Promising role of medicinal plants in the regulation and management of male erectile dysfunction. Biomedicine and Pharmacotherapy, 130. https://doi.org/10.1016/J.BIOPHA.2020.110555 [74] Masuku, N. P., Unuofin, J. O., & Lebelo, S. L. (2020b). Promising role of medicinal plants in the regulation and management of male erectile dysfunction. Biomedicine & Pharmacotherapy = Biomedecine & Pharmacotherapie, 130. https://doi.org/10.1016/J.BIOPHA.2020.110555 [75] Masuku, N. P., Unuofin, J. O., & Lebelo, S. L. (2021). Advances in Nanoparticle Delivery System for Erectile Dysfunction: An Updated Review. Sexual Medicine, 9(5). https://doi.org/10.1016/J.ESXM.2021.100420 [76] Mills, K. T., Bundy, J. D., Kelly, T. N., Reed, J. E., Kearney, P. M., Reynolds, K., Chen, J., & He, J. (2016). Global disparities of hypertension prevalence and control. Circulation, 134(6), 441–450. https://doi.org/10.1161/CIRCULATIONAHA.115.018912 [77] Minh Tue Nguyen, H., Hellstrom, W. J., Gabrielson, A. T., & G Hellstrom, W. J. (2017a). Erectile dysfunction in young men—a review of the prevalence and risk factors. Sexual Medicine Reviews, 5(4), 508–520. https://doi.org/10.1016/j.sxmr.2017.05.004 [78] Minh Tue Nguyen, H., Hellstrom, W. J., Gabrielson, A. T., & G Hellstrom, W. J. (2017b). Erectile dysfunction in young men—a review of the prevalence and risk factors. Elsevier, 5(4), 508–520. https://doi.org/10.1016/j.sxmr.2017.05.004 [79] Mobley, D. F., Khera, M., & Baum, N. (2017a). Recent advances in the treatment of erectile dysfunction. Postgraduate Medical Journal, 93(1105), 679–689. https://doi.org/10.1136/postgradmedj-2016-134073 [80] Mobley, D. F., Khera, M., & Baum, N. (2017b). Recent advances in the treatment of erectile dysfunction. Postgraduate Medical Journal, 93(1105), 679–685. https://doi.org/10.1136/POSTGRADMEDJ-2016-134073 [81] MS Allen. (2019). Physical activity as an adjunct treatment for erectile dysfunction. Journal of Urology Nature Reviews. https://www.nature.com/articles/s41585-019-0210-6 [82] MT, Y., MA, A., AT, O., & AT, O. (2007). Male Sexual Dysfunction and Methods used in Assessing Medicinal Plants with Aphrodisiac Potentials. Pharmacognosy Reviews, 1(1). [83] Muneer, A., Kalsi, J., Nazareth, I., & Arya, M. (2014). Erectile dysfunction. BMJ (Clinical Research Ed.), 348. https://doi.org/10.1136/BMJ.G129 [84] Muneer, A., Kalsi, J., Nazareth, I., Bmj, M. A.-, & 2014, undefined. (2014). Erectile dysfunction. Bmj. https://www.bmj.com/content/348/bmj.g129.abstract [85] O’Flaherty, C., & Matsushita-Fournier, D. (2017). Reactive oxygen species and protein modifications in spermatozoa. Biology of Reproduction, 97(4), 577–585. https://academic.oup.com/biolreprod/article-abstract/97/4/577/4157784 [86] Ogurtsova, K., da Rocha Fernandes, J., D. Huang, Y., Linnenkamp, U., Guariguata, L., Cho, N. H., Cavan, D. S. J., & E. Makaroff, L. E. (2017). IDF Diabetes Atlas: Global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Research and Clinical Practice, 128, 40–50. https://www.sciencedirect.com/science/article/pii/S0168822717303753 [87] Omisanjo, O. A., Ikuerowo, S. O., Abdulsalam, M. A., Ajenifuja, S. O., & Shittu, K. A. (2017). Use of Exogenous Testosterone for the Treatment of Male Factor Infertility: A Survey of Nigerian Doctors. International Journal of Reproductive Medicine, 2017, 1–5. https://doi.org/10.1155/2017/4607623 [88] Osna, N., TM Donohue, & Kharbanda, k. (2017). Alcoholic liver disease: pathogenesis and current management. Alcohol Research?: Current Reviews , 32(2), 147–161. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5513682/ [89] Paick, J. S., Kim, J. J., Kim, S. C., Moon, K. H., Min, K. S., Park, K., Suh, J. K., & Yang, D. Y. (2010). Efficacy and Safety of Mirodenafil in Men Taking Antihypertensive Medications. The Journal of Sexual Medicine, 7(9), 3143–3152. https://doi.org/10.1111/J.1743-6109.2010.01926.X [90] Papagiannopoulos, D., Khare, N., & Nehra, A. (2015). Evaluation of young men with organic erectile dysfunction. Asian Journal of Andrology, 17(1), 11–16. https://www.ncbi.nlm.nih.gov/pmc/articles/pmc4291852/ [91] Patel, J. P., Lee, E. H., Mena-Hurtado, C. I., & Walker, C. N. (2017). Evaluation and Management of Erectile Dysfunction in the Hypertensive Patient. Current Cardiology Reports, 19(9). https://doi.org/10.1007/S11886-017-0889-Z [92] Patton, K., & Thibodeau, G. (2013). Mosby’s handbook of anatomy & physiology. https://books.google.com/books?hl=en&lr=&id=oAAyAgAAQBAJ&oi=fnd&pg=PP1&dq=Mosby%27s+Handbook+of+Anatomy+Physiology&ots=fRNdRe-c4M&sig=sde1V00diilDtqfyLoD8g334uFU [93] Piché, M. lou, Babineau, V., Robitaille, J., Lachance, É., & Ruchat, S. M. (2018). Lifestyle-Related Factors Associated with Reproductive Health in Couples Seeking Fertility Treatments: Results of A Pilot Study. International Journal of Fertility & Sterility, 12(1), 19. https://doi.org/10.22074/IJFS.2018.5135 [94] Pociot, F., & Lernmark, Å. (2016). Genetic risk factors for type 1 diabetes. The Lancet, 387(10035), 2331–2339. https://www.sciencedirect.com/science/article/pii/S0140673616305827 [95] Quaglio, G., Lugoboni, F., Pattaro, C., & Melara, B. (2008). Erectile dysfunction in male heroin users, receiving methadone and buprenorphine maintenance treatment. Drug and Alcohol Dependence. https://www.sciencedirect.com/science/article/pii/S0376871607004280 [96] Rajkumar, R., psychiatry, A. K.-C., & 2015, undefined. (2015). Depression and anxiety in men with sexual dysfunction: a retrospective study. Comprehensive Psychiatry. https://www.sciencedirect.com/science/article/pii/S0010440X15000346 [97] Ramírez, R., Pedro-Botet, J., García, M., Corbella, E., Merino, J., Zambón, D., Corbella, X., & Pintó, X. (2016). Erectile dysfunction and cardiovascular risk factors in a Mediterranean diet cohort. Internal Medicine Journal, 46(1), 52–56. https://doi.org/10.1111/IMJ.12937 [98] Rewers, M., & Ludvigsson, J. (2016). Environmental risk factors for type 1 diabetes. The Lancet, 387(10035), 2340–2348. https://www.sciencedirect.com/science/article/pii/S0140673616305074 [99] Rizzo, D. (2015). Fundamentals of anatomy and physiology. https://books.google.com/books?hl=en&lr=&id=dvioBAAAQBAJ&oi=fnd&pg=PR5&ots=WYr1XaIGf7&sig=ERPJUSIsHbYBShN-0Ub_V7CFpMs [100] Robert C. Dean, & Tom F. Lue. (2005). Physiology of penile erection and pathophysiology of erectile dysfunction and priapism. Urology Clinical North America, 32(4), 379. https://ci.nii.ac.jp/naid/10012788846/ [101] Schwartz, B. G., Rezkalla, S., & Kloner, R. A. (2010). Cardiovascular effects of cocaine. Circulation, 122(24), 2558–2569. https://doi.org/10.1161/CIRCULATIONAHA.110.940569 [102] Sharma, V., Thakur, M., Chauhan, N. S., & Dixit, V. K. (2010a). Effects of petroleum ether extract of Anacyclus pyrethrum DC. on sexual behavior in male rats. Zhong Xi Yi Jie He Xue Bao = Journal of Chinese Integrative Medicine, 8(8), 767–773. https://doi.org/10.3736/JCIM20100807 [103] Sharma, V., Thakur, M., Chauhan, N. S., & Dixit, V. K. (2010b). Immunomodulatory activity of petroleum ether extract of Anacyclus pyrethrum. Pharmaceutical Biology, 48(11), 1247–1254. https://doi.org/10.3109/13880201003730642 [104] Sherwood, L. (2006). Sherwood: Fundamentals of physiology: a human perspective - Google Scholar. https://scholar.google.com/scholar_lookup?title=Fundamentals%20of%20Physiology%3A%20A%20Human%20Perspective&publication_year=2006&author=L.%20Sherwood [105] Shiferaw, W. S., Akalu, T. Y., & Aynalem, Y. A. (2020). Prevalence of Erectile Dysfunction in Patients with Diabetes Mellitus and Its Association with Body Mass Index and Glycated Hemoglobin in Africa: A Systematic Review and Meta-Analysis. International Journal of Endocrinology, 2020. https://doi.org/10.1155/2020/5148370 [106] Sin, V. J. E., Anand, G. S., & Koh, H. L. (2021). Botanical Medicine and Natural Products Used for Erectile Dysfunction. Sexual Medicine Reviews, 9(4), 568–592. https://doi.org/10.1016/J.SXMR.2020.10.005 [107] Singh Grewal, G., Gill, J. S., Sidi, H., Gurpreet, K., Jambunathan, S. T., Suffee, N. J., Midin, M., Ruzyanei, N., Jaafar, N., & Das, S. (2014). Prevalence and risk factors of female sexual dysfunction among healthcare personnel in Malaysia. Comprehensive Psychiatry. https://doi.org/10.1016/j.comppsych.2013.01.009 [108] Uddin, S. M. I., Mirbolouk, M., Dardari, Z., Feldman, D. I., Cainzos-Achirica, M., DeFilippis, A. P., Greenland, P., Blankstein, R., Billups, K. L., Miner, M. M., Nasir, K., & Blaha, M. J. (2018). Erectile dysfunction as an independent predictor of future cardiovascular events: The multi-ethnic study of atherosclerosis. Circulation, 138(5), 540–542. https://doi.org/10.1161/CIRCULATIONAHA.118.033990 [109] Venkatesh, K., Mattoo, S., Medicine, S. G.-T. J. of S., & 2014, undefined. (2014). Sexual dysfunction in men seeking treatment for opioid dependence: a study from India. The Journal of Sexual Medicine. https://www.sciencedirect.com/science/article/pii/S1743609515301028 [110] Viigimaa, M., Vlachopoulos, C., Lazaridis, A., & Doumas, M. (2014). Management of erectile dysfunction in hypertension: Tips and tricks. World Journal of Cardiology, 6(9), 908–915. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4176800/ [111] Wassersug, R., & Wibowo, E. (2017). Non-pharmacological and non-surgical strategies to promote sexual recovery for men with erectile dysfunction. Translational Andrology and Urology, 6(Suppl 5), S776–S794. https://doi.org/10.21037/TAU.2017.04.09 [112] Wen, L., Rissel, C., Cheng, Y., health, J. R.-S., & 2017, undefined. (2017). Tobacco smoking and sexual difficulties among Australian adults: a cross-sectional study. Sexual Health. https://www.publish.csiro.au/sh/sh17005 [113] West, E., & Krychman, M. (2015). Natural Aphrodisiacs—A Review of Selected Sexual Enhancers. Sexual Medicine Reviews, 3(4), 279–288. https://doi.org/10.1002/SMRJ.62 [114] Widmaier, E., Raff, H., & Strang KT. (2008). Vanders Human Physiology: The Mechanism of Body Functions - Google Scholar. McGrew-Hill, 555–631. https://scholar.google.com/scholar?q=Vanders%20Human%20Physiology:%20The%20Mechanism%20of%20Body%20Functions [115] Williams, P., McBain, H., … K. M.-I. J. of, & 2014, undefined. (2014). Cardiovascular disease: The effect of erectile dysfunction on adherence to cardiovascular disease medication. Wiley Online Library, 8(2), 54–61. https://doi.org/10.1111/ijun.12032 [116] Yadav, R., & Agarwala, M. (2011). Phytochemical analysis of some medicinal plants. Journal of Phytology, 3(12), 10–14. https://www.researchgate.net/profile/Fatima-Hussen-2/post/How_can_I_isolate_the_active_constituents_of_a_plant/attachment/59d63f1bc49f478072ea9748/AS%3A273775847772169%401442284657308/download/1.+Phytochemical+analysis+of+some+medicinal+plants%281%29.pdf [117] Yafi, F. A., Jenkins, L., Albersen, M., Corona, G., Isidori, A. M., Goldfarb, S., Maggi, M., Nelson, C. J., Parish, S., Salonia, A., Tan, R., Mulhall, J. P., & Hellstrom, W. J. G. (2016). Erectile dysfunction. Nature Reviews Disease Primers 2016 2:1, 2(1), 1–20. https://doi.org/10.1038/nrdp.2016.3 [118] Yakubu, M. T., & Afolayan, A. J. (2010). Anabolic and androgenic activities of Bulbine natalensis stem in male Wistar rats. Pharmaceutical Biology, 48(5), 568–576. https://doi.org/10.3109/13880200903207094 [119] Yee, A., Danaee, M., Loh, H. S., Sulaiman, A. H., & Ng, C. G. (2016). Sexual dysfunction in heroin dependents: A comparison between methadone and buprenorphine maintenance treatment. PLoS ONE, 11(1). https://doi.org/10.1371/JOURNAL.PONE.0147852 [120] Yeh, K. Y., Pu, H. F., Kaphle, K., Lin, S. F., Wu, L. S., Lin, J. H., & Tsai, Y. F. (2008). Ginkgo biloba extract enhances male copulatory behavior and reduces serum prolactin levels in rats. Hormones and Behavior, 53(1), 225–231. https://doi.org/10.1016/J.YHBEH.2007.10.001 [121] Yeoh, S. H., Razali, R., Sidi, H., Razi, Z. R. M., Midin, M., Jaafar, N. R. N., & Das, S. (2014). The relationship between sexual functioning among couples undergoing infertility treatment: a pair of perfect gloves. Comprehensive Psychiatry, 55(SUPPL. 1), S1–S6. https://doi.org/10.1016/J.COMPPSYCH.2012.09.002 [122] Yousef Kamel Qawqzeh, Mamun Ibne Reaz, & Mohd Aluadin Mohd Ali. (2012). The Assessment of Atherosclerosis in Erectile Dysfunction Subjects Using Photoplethysmography. In Erectile Dysfunction (pp. 195–214). https://books.google.com/books?hl=en&lr=&id=EpifDwAAQBAJ&oi=fnd&pg=PA195&ots=M4N739couu&sig=JKbjjEHwDqUxOPiet0zNapbK9Rg [123] Zheng, Y., Ley, S. H., & Hu, F. B. (2017). Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nature Reviews Endocrinology, 14(2), 88–98. https://doi.org/10.1038/nrendo.2017.151 [124] Zhou, Q., & Melton, D. A. (2018). Pancreas regeneration. Nature, 557(7705), 351–358. https://www.nature.com/articles/s41586-018-0088-0
Copyright
Copyright © 2022 Ashish ., Dr. Gurdeep Singh. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET44012
Publish Date : 2022-06-09
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

