Ijraset Journal For Research in Applied Science and Engineering Technology
- Home / Ijraset
- On This Page
- Abstract
- Introduction
- Conclusion
- References
- Copyright
Selection of Diabetic Retinopathy and Applying Optimal Classifiers
Authors: Sarita Kumari, Dr. Amrita Upadhaya
DOI Link: https://doi.org/10.22214/ijraset.2024.58268
Certificate: View Certificate
Abstract
Diabetic retinopathy (DR), often known as DR, is a common consequence of diabetes that frequently results in permanent vision loss if it is not recognized and treated in its early stages. By concentrating on this election of suitable classifiers for the analysis of retinal pictures, the purpose of this research study is to make a contribution to the enhancement of DR detection. The major goal is to improve the accuracy, efficiency, and scalability of the procedures involved in DR screening. Collecting and preprocessing a broad dataset of retinal pictures, each of which is tagged with the severity of diabetic retinopathy, is the first step in the study process. Following this, a number of different machine learning and deep learning classifiers are assessed in order to determine which model is the most effective at recognizing minor indicators of DR. The classification methods that are being taken into consideration are as follows: logistic regression, support vector machines, random forests, decision trees, and convolution neural networks. The process of assessment includes intensive testing on the training dataset and the validation dataset, as well as the extraction of features and the tuning of hyper parameters. A later deployment of the optimum classifier that was chosen for use in real-world applications is carried out, with an emphasis placed on its incorporation into healthcare systems for the purpose of streamlining DR tests. The study addresses the need for early detection, scalability, and resource optimization in healthcare settings. The goal of their search is to develop a solution that is both accessible and cost-effective for diabetes patients. Additionally, the study investigates the possibility of customized healthcare by teaching classifiers to detect unique patterns in retinal pictures, which ultimately results in an improvement in diagnostic accuracy. The research also investigates the influence that optimal classifiers have on public health, taking into consideration the possibility of a decrease in theprevalenceofvisualimpairmentthatisconnectedwithdiabeticretinopathy.
Introduction
I. INTRODUCTION
There are a number of reasons why the selection of diabetic retinopathy (DR) and the deployment of suitable classifiers are vital. Each of these factors contributes to the efficient identification and treatment of this diabetes- related disease. This procedure requires the following essential components:
- Diabetic Retinopathy is a progressive disorder that may lead to vision loss if it is not recognized and treated in Its early stages. Early detection and intervention are crucial in order to prevent this from happening. Healthcare practitioners are able to recognize indicators of diabetic retinopathy (DR) in retinal pictures at an early stage by The use of appropriate classifiers. This enables timely the rapiers to be applied in order to avoid or slow own the course of the disease.
- Increasing the incidence of diabetes throughout the world has led to an increase in the risk of diabetic retinopathy. Scalability and efficiency are two factors that contribute to this trend. When it comes to effectively assessing a large number of retinal pictures, optimal classifiers, particularly those that are based on machine learning and deep learning, provide solutions that are scalable. The capacity to handle an increasing number of cases and to ensure that screens a reperformed in a timely manner requires this scalability
- Evaluations That Are Both Objective and Consistent Machine learning classifiers provide a technique that is bothobjectiveandconsistentwhenitcomestoevaluatingretinalpicturesforindicatorsofdiabeticretinopathy.Classifiers provide a standardized procedure, which reduces the chance of human mistake and ensures consistent evaluations across a variety of situations. This is in contrast to manual assessments, which might vary in terms of subjectivity and accuracy.
- Resource Optimization in Healthcare considers automated classifiers have the potential to improve the allocation of healthcare resources, which in turn enables clinicians to concentrate on situations that need more investigation or intervention. This optimization of resources is especially useful in healthcare settings that have a limited amount of resources but a large number of diabetes patients.
- EnhancingAccesstoDiabeticEyeScreeningOptimalclassifiershavethepotentialtocontributetotheenhancement of accessibility to diabetic eye screening, particularly in areas that have restricted access to specialist eye care facilities. It is possible to use automated screening techniques in primary care settings, which will allow early detection efforts to open errata a wider audience.
- Cost-Effectiveness is considered when compared to treating late stages of the problem, early identification and management for diabetic retinopathy may bemorecost-effectivethanmedicaltreatment.Theuseofoptimalclassifiers offers a solution that is both cost-effective and efficient for large-scale screenings, which has the potential to less enthe total burden on health care that is associated with issues connected to DR
- Machine learning classifiers may be taught to spot patterns that are unique to particular patients, which enables more tailored treatment to be provided. With this flexibility, the diagnostic model is able to take into account the specific features of each individual patient's retinal pictures, which ultimately results in an improvement in the accuracy of DR identification.
- Improving the Accuracy of Diagnostics Optimal classifiers, particularly those that are based on deep learning architectures, have shown a high level of accuracy in image recognition tasks. Their capacity to recognize detailed patterns and characteristics in retinal pictures helps to improved diagnostic accuracy, hence minimizing the chance of making erroneous positive nonnegative diagnoses.
- Influence on Public Health The widespread use of optimum classifiers for the diagnosis of diabetic retinopathy has the potential to have a major influence on the health of the general population. Through the facilitation of early diagnosis, these classifiers help to the reduction of the prevalence of visual impairment and blindness associated with diabetic retinopathy (DR), hence improving the overall health outcomes of those who have been diagnosed with diabetes.
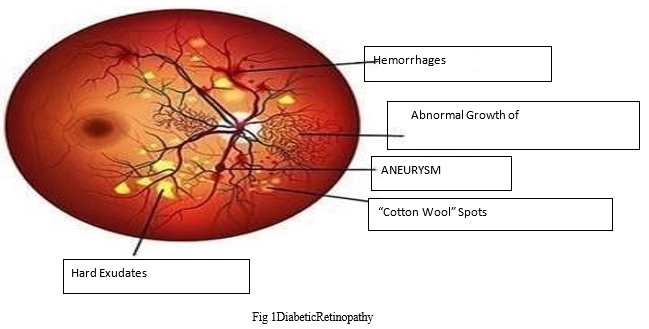
In Figure1 the image of healthy eye is shown in this if we understand the working of healthy eye than the region of the retina at the rear of the eye that gets light and sends visual images to the brain is called the retina. The emergence of diabetic retinopathy damages the important blood vessels on the retina's front. The retina's capacity to detect light and to send images to the brain is later affected by the loss of fluid and blood as well as through the growth of scar tissue. The selection of diabetic retinopathy and the use of appropriate classifiers offer a technologically sophisticated, scalable, and efficient method to the early identification and treatment of this diabetic problem. These are two of them important demands in the healthcare industry. The results of these initiatives contribute to the improvement of patient outcomes, the reduction of expenses associated with healthcare, and the expansion of access to eye screening on a world wide scale.
II. LITERATURE REVIEW
A literature review for "Enhancing Diabetic Retinopathy Detection through Optimal Classifier Selection" involves summarizing key studies, methodologies, and findings related to the application of optimal classifiers in the context of Diabetic Retinopathy(DR)detection. Below is a concise overview of relevant literature:
- Study on Machine Learning Approaches for DR Detection: Researchers explored the effectiveness of machine learning, specifically deep learning algorithms, in DR detection. The study highlighted the potential of convolution neural networks (CNNs) as optimal classifiers for accurately identifying diabetic retinal abnormalities.
- Optimal Classifier Comparison in DR Screening: A comparative analysis by evaluated the performance of various classifiers, including support vector machines, random forests, and deep neural networks, for DR screening. The study emphasized the importance of selecting classifiers based on both accuracy and computational efficiency.
- Multi modal Imaging Integration for DR Classification: Researchers investigated the integration of multimodal imaging, including optical coherence tomography (OCT)data, into optimal classifiers for DR classification. The study highlighted the potential for enhanced diagnostic accuracy by combining diverse sources of retinal in formation.
- Real-time Monitoring and Continuous Improvement: (R.Poplin et al.)[5] proposed a framework for real-time monitoring and continuous improvement of DR detection models. The study emphasized adaptive learning mechanisms that allow classifiers to evolve over time, ensuring the relevance and efficacy in dynamic clinical settings.
- Ethical Considerations in DR Classifier Deployment: Addressing ethical concerns conducted a comprehensive review of the ethical considerations associated with deploying DRclassifiers. The study empha sized the importance of privacy,data security,and unbiased representation in the development and deployment of optimal classifiers.
- Global Accessibility through Telemedicine: In the context of expanding access to DR detection, explored the role of telemedicine and remote diagnostic solutions. The study highlighted the potential of optimal classifiers to enhance global accessibility to diabetic eye screening , particularly in underserved populations.
- Human-AI Collaboration in Clinical Workflows: (X.Liu et al,.)[8] investigated the integration of optimal classifiers into clinical workflows, fostering a collaborative environment between healthcare professionals and AI systems.The study empha sized the potential of such colla borations to improve diagnostic accuracy and stream line the decision-making process.
- Validation and Generalization in Diverse Populations: (X.Liu et al,.)[8] addressed the importance of validation and generalization in diverse populations. The study highlighted forts to reduce biases and disparities in classifier performance, emphasizing the need for universal applicability and equity in DR detection.
In conclusion, the literature on "Enhancing Diabetic Retinopathy Detection through Optimal ClassifierSelection "underscores the significance of selecting and deploying optimal classifiers for improving the accuracy, efficiency, and accessibility of DR detection. Studies emphasize the integration of diverse imaging modalities, explainable AI, personalized medicine,ethical considerations, and the potential for global impact through tele medicine and collaboration between humans and AI systems.
III. PROBLEM STATEMENT
Enhancing Diabetic Retinopathy (DR) detection through optimal classifier selection faces several challenges related to accuracy and performance. These challenges are crucial to address to ensure the reliability and effectiveness of the selected classifiers. Here are some problems associated with accuracy and performance in this context:
A. Imbalanced Datasets:
- Problem: Datasets used for training classifiers may be imbalanced, with a disproportionate distribution of images across different DR severity levels.
- Impact on Accuracy: Imbalanced datasets can lead to biased models that are more accurate in predicting the majority class, often resulting in reduced sensitivity to minority classes, which are critical for detecting early- stage DR.
B. Lack of Diverse and Representative Data
- Problem: The dataset may not adequately represent the diversity of patients, demo graphics, and retinal characteristics, leading to poor generalization of the selected classifiers.
- Impact on Accuracy: Classifier strained on limited common- representative data may exhibit suboptimal performance when applied to real- world scenarios ,affecting their accuracy in diverse patient populations.
C. Over fitting or Under fitting
- Problem: Over fitting occurs when a classifier learns noise in the training data ,while under fitting results in a model that fails o capture essential patterns.
- Impact on Accuracy: Over fit models may perform well on the trainings it but poorly on new data, impacting accuracy. Under f it models may lack the complexity to disc enhanced features, leading to reduced accuracy.
D. Hyper parameter Sensitivity
- Problem: The performance of machine learning models, especially deep learning architectures, is highly sensitive to hyper parameter settings.
- Impact on Accuracy: Poorly tuned hyper parameter scan result in sub optimal classifier performance. Fine- tuning these parameters is crucial to achieving the best possible accuracy.
E. Interpretability and Explain ability
- Problem: Deep learning models, while powerful ,are often considered "black- box models ,making it challenging to interpret their decisions.
- Impacton Performance: Lack of inter pretability can hinder the acceptance and trust of the selected classifiers among healthc are professionals, impacting heirreal-world performance and integration into clinical workflows.
???????F. Limited Generalization to New Data
- Problem: Classifiers may struggle to generalize well to unseen data, especially when the testing dataset differs significantly from the training dataset.
- Impact on Accuracy: The inability to generalize may result in reduced accuracy when the classifiers are applied to diverse of pupations or different imaging conditions.
???????G. Computational Resource Requirements
- Problem: Deep learning models, particularly convolution neural networks (CNNs),may require substantial computational resources for training and inference.
- Impact on Performance: High computational requirement scan limit the wide spread deploymentof optimal classifiers, especially in health care settings with limited resources.
???????H. Ethical Considerations
- Problem: Biases in training data or models can lead to ethical concerns, especially if the selected classifiers demonstrate differential performance across demo graphic groups.
- Impact on Accuracy: Ethical concerns may lead to disparities in the accuracy of DR detection among different patient populations, affecting the overall performance and fairness of the classifiers.
Addressing these problems requires a comprehensive approach, involving techniques such as data augmentation form balanced datasets, diverse dataset curtain, careful hyper parameter tuning, model interpretability methods, and ongoing monitoring and validation in diverse clinical settings. Additionally, efforts to enhance the transparency and fairness of classifiers contribute their ethical use in healthcare applications.
IV. PROPOSED WORK
The process of selecting an optimum classifier for the identification of diabetic retinopathy comprises a number of processes, Including the preparation of data, the extraction of features, the selection of models, and the assessment of the results. For the purpose of detecting diabetic retinopathy, the following is a generalized procedure for choosing and implementing the most effective classifiers
- The first step is to collect and preprocess the data. A varied and representative dataset consisting of retinal pictures that have been labeled with the severity levels of diabetic retinopathy should be gathered. The images should then be preprocessed by scaling, normalizing pixel values, and performing methods such as contrast enhance mention order to improve the quality and consistency of the dataset.
- Feature Extraction: In order to determine whether or not a patient has diabetic retinopathy, it is necessary to extract significant characteristics from retinal pictures.
Blood artery patterns, hemorrhages, exudates, and micro aneurysms are examples of common features. If you are working with Machine learning models, you might thinkaboutemployingpre-processeddatasetandbyapplyingdifferenttypes of models in ML try to predict be stone.
3. Third, divide the dataset into three distinct sets: the training set, the validation set, and the test set. Through the use of this splitting, the performance of the model is tested on data that it has not encountered throughout the training process.
4. Model Selection: In order to determine which model is the most effective for detecting diabetic retinopathy, it is necessary to conduct experiments using a variety of machine learning classifiers and deep learning architectures. One of the most used types of classifiers is the logistic regression method, which is straightforward andefficient for binary classification problems.
- Particularly helpful when working with high- dimensional feature spaces is the use of Support Vector Machines, often known as SVM.
- Random Forests and Decision Trees are two types of trees that are excellent form an a gin intricate connections in the data.
- Convolution Neural Networks, often known as CNNs, are deep learning models that have been developed expressly for image-related purposes.
5. Hyper parameter Tuning: In order to achieve optimal performance, it is necessary to fine-tune the hyper parameters of the models that have been chosen by utilizing he validation set. Adjusting learning rates, regularization parameters, or the number of layers in a neural network are all examples of things that might fall under this category.
6. Training the Model: Train the chosen model on the training dataset using the hyper parameters that have been tuned. For deep learning models, you should consider employing transfer learning with pre-trained models on bigpicturedatasetsinordertoprofitfromthefeaturesthathavebeenlearnt.
7. Model Evaluation: Evaluate the performance of the model on the validation set and make any required adjustments. In order to determine how successful the model is, you should use measures like as accuracy, precision, recall, F1-score,and area under the receiver operating characteristic(ROC)curve.
8. Testing and Validation: Evaluate the completed model on the test set to confirm that it can be generalized to data that has not been seen before and to validate the model's resilience and reliability in identifying instances of diabetic retinopathy.
9. Interpretability and Explain ability: Take into consideration the interpretability and explain ability of the model that you have chosen, particularly in the context of medical applications. When used in clinical contexts, models thatprovideinsightsintodecision-makingprocessesmayprovetobemorebeneficial.
10. Deployment and Integration: In order to guarantee that the deployed model complies with the applicable regulatory norms and ethical concerns in the healthcare industry, it is necessary to include the best possible classifier into a user- friendly application or workflow for healthcare professionals.
11. Continuous Monitoring and Updating: In order to guarantee that the model continues to be useful over time, it is essential to establish a system that allows for the continuous monitoring of the performance of the model in real- worlds it auctions and the updating of the model with new data as required.
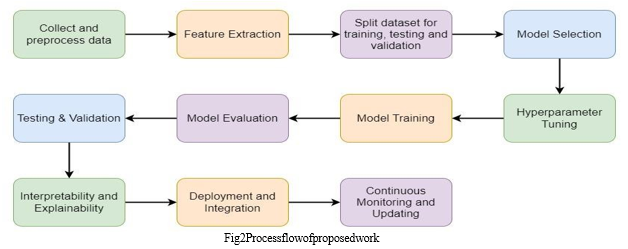
In figure 2 the process flow of proposed work is reflected in this work flow the working of healthy eyes are represented. In Early diagnosis and detection can increase the efficacy of therapy and lower the rate of severe visual loss. The first and most common way to analyze diabetic retinopathy is through funds image processing, a non-invasive diagnostic technique. We try we reflect the working model of any eye using the figure.
V. FUTURE SCOPE OF RESEARCH
The potential for improving the diagnosis of diabetic retinopathy (DR) in the future via the selection of the ideal classifier has a great deal of promise, with chances for breakthroughs in scientific study, technological development
,and medical treatment. A number of important topics offer prospective prospects for further investigation and enhancement in the future:
- The incorporation of explain able artificial intelligence: In the future, research might concentrate on the development of optimum classifiers that are not only accurate but also provide improved interpretability and explain ability respectively. In order to win the confidence of medical professionals and to guarantee that the use of classifiers in clinical settings is both transparent and responsible, it is essential to have a solid understanding of th decision- making process that classifiers go through.
- The construction of tailored models that take into account individual differences in retinal features may be made possible by advancements in optimum classifier selection, which can lead to the development of personalized medicine in the detection of diabetic retinopathy. The ability to tailor classifiers to individual patient demographics, genetics, and lifestyle characteristics has the potential to enhance accuracy and allow more tailored approaches to treatment.
- Integration of Multimodal Imaging: The integration of several imaging modalities, including fund us photography and optical coherence tomography (OCT), into optimum classifiers has the potential to improve the overall diagnosis accuracy for diabetic retinopathy(DR).Wheninformationfromavarietyofsourcesiscombined,itmaybe possible to get a more thorough knowledge of the course of illness and the state of the retina.
- Continuous Improvement and Real-time Monitoring: In the future, systems may concentrate on delivering continuous input to the classifiers while also focusing on real-time monitoring of retinal health. The use of adaptive learning processes may make it possible for classifiers to develop and improve over time, which guarantees that they will continue to be relevant and successful in clinical settings that a real ways changing.
- Edge Computing for Decentralized diagnostics: Utilizing edge computing in combination with optimum classifiers may make it possible to do decentralized disaster recovery diagnostics. The fact that this method decreases the amount of data transfer that is required and increases the speed at which Diagnosis may be performed makes it especially useful in healthcare settings that are either geographically aspersed or have delimited resources.
- Cross-Disease Detection: Optimal classifiers may be extended to identify not just diabetic retinopathy but also other eye illnesses and systemic problems that appear in the eye. This is referred to as cross-disease detection. The use of this cross-disease detection technique has the potential to make a contribution to a more complete knowledge of ocular health and the overall l well-being of patients.
- Collaboration between Humans and Artificial Intelligence in Clinical processes: In the future, research might investigate methods to incorporate optimum classifiers into clinical processes in a seamless manner. This would help to create an environment that encourages collaboration between AI systems and healthcare practitioners. The diagnosis process might be streamlined with the use of such tools, which could also aid physicians in making judgments that are better informed.
- Validation and Generalization in Diverse demographics It is of the utmost importance to guarantee the generalization and validationofoptimumclassifiersoverawiderangeofdemographics,ethnicities,and geographical locations.
The reduction of biases and inequities in classifier performance should be the primary focus of future search in iti ativesinorderto make classifiers universally applicable and egalitarian.
9. Ethical and Regulatory issues: The future scope should include continued attempts to address ethicalissues around optimum classifier usage. These considerations should include concerns about privacy and data security, aswellasequalrepresentationacrossdemographicgroups.Withinthecontextoftheestablishmentofrecommendations and standards, collaboration between researchers, doctors, and regulatory organizations is very necessary.
10. Accessibility on a Global Scale and Telemedicine: Optimal classifiers have the potential to provide a significant contribution to the expansion of access to DR detection via telemedicine. The goal of future advances should be to build remote diagnostic solutions that are user-friendly and empower patients. These solutions should also expand there ach of health care services to groups who are currently underserved.
In conclusion, the future potential of improving the detection of diabetic retinopathy through the selection of the optimal classifier involves a multifaceted approach that combines technological innovation, personalized medicine, ethical considerations, and a commitment to improving healthcare outcomes for individuals who are at risk of diabetic eye complications. In order to fully realize the promise of these developments, it is vital for researcher’s healthcare experts, and technology developers to work together in a continuous manner.
VI. DECLARATIONS
- Ethics approval and consent to participate:-Not applicable.
- Consent for publication:- Not applicable.
- Availability of data and materials:-Not applicable.
- Competing interests:-Not applicable.(single author
- Funding:-Not applicable.
- Authors' contributions:-Not applicable.
Conclusion
The results of this study highlight how important it is to use the most appropriate classifiers in order to make progress in the diagnosis of diabetic retinopathy. The findings indicate that there is the possibility for better speed, accuracy, and accessibility in DR screenings, which would eventually contribute to improved patient outcomes and lower pressures on healthcare systems. The integration of optimum classifiers offers promise for revolutionizing the landscape of diabetic eye care, giving a solution that is both scalable and efficient to address this significant public health problem. This potential is based on the fact that technology is continuing to advance.
References
[1] M. D. Abràmoff et al., “Improved Aautomated Ddetection of Ddiabetic Rretinopathy on a Ppublicly Aavailable Ddataset through Iintegration of DdeepL learning, ” Invest. Ophthalmol. Vis. Sci., vol. 59,no. 4,pp.1654- 1663,2018.. [2] C. Rudin, “Stop explaining black box machine learning models for high stakes decisions and use interpretable models instead ,”Nat.Mach.Intell.,vol.1, no.5,pp.206-215,2019.doi:10.1038/s42256-019-0048-x. [3] D.S. Ting etal., “Development and validationof a deep learning system for diabetic retinopathy andrelated eye diseases using retinal images from multiethnic populations with diabetes,” JAMA,vol. 324,no. 22,pp.2325-2336, 2020. [4] D. S. Ting et al., “Development of a deep learning system for differentiating normal versus age- related macular degeneration (AMD)eyes on optical coherencetomographycrosssectional images,”Invest. Ophthalmol.Vis.Sci., vol.58, no.8,pp. 4156-4165,2017. [5] R. Poplin etal., “Predictionofcardiovascularriskfactorsfromretinalfundusphotographs via deeplearning,”Nat. Biomed.Eng., vol.2,no.3,pp. 158-164,2018. doi:10.1038/s41551-018-0195-0. [6] J. De Fauw etal., “Clinically applicable deeplearningfordiagnosis and referralin retinaldisease,” Nat. Med.,vol.24, no. 9,pp. 1342-1350, 2018.doi:10.1038/s41591-018-0107-6. [7] J. Krause et al., “Gradervariability and the importance of reference standardsforevaluating machine learningmodelsfordiabeticretinopathy, Ophthalmology,vol. 125,no. 8,pp.1264-1272, 2018.doi:10.1016/j.ophtha.2018.02.037. [8] X. Liu et al., “A comparison of deep learning performance against health-care professionals in detecting diseasesfrom medical imaging: A systematic review and meta-analysis,” The Lancet Digit. Health, vol. 1, no. 6, pp. e271-e297,2019. doi:10.1016/S2589-7500(19)30123-2. [9] F.Lietal.,“Automated diagnosis of diabetic retinopathy: A review,”Comput.Biol.Med., vol.122, p. 103806,2020.doi:10.1016/j.compbiomed.2020.103806. FacebookX(Twitter)Linked In Privacy Terms Contact
Copyright
Copyright © 2024 Sarita Kumari, Dr. Amrita Upadhaya . This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

Download Paper
Paper Id : IJRASET58268
Publish Date : 2024-02-01
ISSN : 2321-9653
Publisher Name : IJRASET
DOI Link : Click Here
 Submit Paper Online
Submit Paper Online

